Considering the numerous adverse effects of sleep disorders, it is imporant to properly assess sleep problems in all age groups.

An estimated 20% to 25% of children/youth experience some form of sleep disturbance,4 while 50% of adults 65 or older report sleep-related complaints.5 The clinical signs and symptoms observed in children/youth are variable within age groups, and frequently differ from those exhibited by adults.6,7 For instance, symptoms of insufficient sleep may seem paradoxical in preadolescents, because instead of lethargy, those in this age group who have sleep disorders frequently exhibit inattentiveness, hyperactivity, and aggressive behaviors.4,8,9 Conversely, the most common symptom observed in adults is excessive daytime sleepiness. The presence of sleep disorders is not specific to age, yet the presentation of sleep irregularities and the consequences to an individual’s health change as a result of the natural aging process.
Despite the increased risk for physiological and psychological problems, accidents, loss of worker productivity, and increased medical resource utilization associated with sleep disorders,10 assessment of sleep problems is inadequate across all age ranges. Indeed, 61% of adults indicate never being asked about sleep problems by a physician; and less than a third of adults over the age of 65 have ever been assessed for sleep problems.11 Moreover, children are routinely diagnosed with ADD/ADHD and prescribed medication without considering the possibility of a sleep disorder. Ignorance regarding the characteristics of sleep disorders and their effects is ubiquitous, spanning all age groups. Information regarding distinguishable characteristics in epidemiology, symptoms, and psychological effects of sleep problems is insufficient across the life span. We investigated sleep disorders in children/youth (ages 0-16), adult (ages 17-64), and geriatric (ages 65+) populations and compared findings among the groups.
Our Approach
We assembled a team comprised of professionals from a broad spectrum of specialty areas and constructed a 92-item questionnaire and a 12-item questionnaire for children/youth to assess both the children/youth and caregiver perspectives. A 111-item questionnaire was constructed for use in our older populations. The 92-item and 111-item questionnaires were composed of the same questions; however, age-appropriate questions that were nonapplicable to children/youth were added to the version used for people age 17 and over. The 12-item questionnaire was used solely to assess if the children/youth perspectives of their sleep and sleep habits coincided with the caregiver’s perspectives. We used questionnaires to assess sleep habits, sleep observations, past medical and psychological history, prior treatment approaches for sleep disorders, social data, and medications. We used the questionnaire in conjunction with other standard patient questionnaires, nocturnal polysomnography studies, multiple sleep latency tests (MSLT), the Epworth Sleepiness Scale (ESS), and medical chart reviews of people referred to our institution for evaluation of sleep disorders. Additionally, postnocturnal polysomnography follow-up questionnaires were administered to obtain data on changes in symptoms and compliance with treatment approaches. We constructed a database comprised of 421 measures to track data from participants.
Results
We compared age-appropriate data for 570 people who were referred for evaluation of sleep problems based on traditionally defined age classifications. They included 33 children/youth (mean age: 10.89, range: 1-16), 422 adult (mean age: 46.37, range: 17-64), and 115 geriatric (mean age: 71.75, range: 65-88) participants. The length of time that participants had sleep problems prior to use of nocturnal polysomnography was reported by children/youth as 5.21 years, by adults as 9.63 years, and by the geriatric population as 8.34 years. There were no differences in the proportion of men and women in each of the age classifications. While there are numerous sex differences within age categories,12 this paper will focus on differences among age groups irrespective of sex.
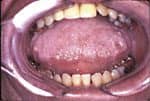
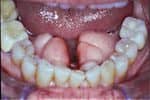
When comparing data among groups, we found numerous significant differences. Examples of significant findings include: children/youth were significantly more likely to exercise daily (X28=43.653, P=.000), to experience difficulties concentrating (X22=17.757, P=.000), to have been diagnosed with ADD/ADHD (X22=28.723, P=.000) and/or another form of psychological disorder (X22=16.643, P=.000), and to have a family history of a SD (X22=9.257, P=.010) than were the adult and geriatric populations. Adults were significantly more likely to snore (X22=12.132, P=.002), grind their teeth during sleep (X22= 12.852, P=.002), wake with a choking sensation (X22=16.075, P=.000), have an accident or near accident due to sleepiness (X22=11.561, P=.003), and experience stress (X21=18.246, P=.000) and headaches (X22=37.740, P=.000). Those in the geriatric group were significantly more likely to report always having to use the restroom during the night (X28=21.744, P=.005), waking rested (X22=23.279, P=.000), and taking naps during the day (X22=16.485, P=.000) than their younger counterparts. Furthermore, the geriatric population reported that sleepiness had the least effect on both their work/school performance (X28=32.711, P=.000) and social lives (X28=31.742, P=.000).
Data from nocturnal polysomnography revealed significant differences in diagnosis types and sleep architecture when comparing the groups (see Tables 1 and 2).
 Table 1. Significant differences in diagnoses types: traditional age classifications.
|
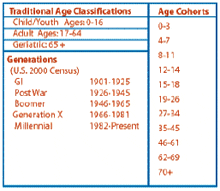
Investigating differences in patterns of sleep disorder symptomatology, physical and psychological problems, and sleep study results yielded many differences when comparing children/youth, adult, and geriatric populations; however, we found that these broad classifications are not always specific enough to discern changes in sleep throughout the life span. Using these classifications, a 6 year old is grouped with a 16 year old, and there are obvious fundamental differences that occur between these ages. Thus, we are currently further investigating sleep disorders and related symptoms by defining three separate methods of age categorization. In Type 1, Traditional Age Classifications are used (child/youth, adult, and geriatric). Type 2, Generation Classifications, as defined by the USA 2000 census, further delineates five distinct groups. Type 3, the most detailed system, classifies participants into 11 different age cohort groups based on developmental, social, psychological, and environmental influences to obtain a clearer understanding of changes in sleep throughout the aging process (see Table 3).
Table 3. Definitions of age
Table 5. Age cohort differences.
We found numerous differences when analyzing data by the more specific age classification methods. For example, when analyzing by traditional classifications, adults as a whole were the most likely to report an accident or near accident due to sleepiness. Analysis by more specific criteria showed that adults in Generation X were significantly more likely to report this than any other generation (X24=15.180, P=.004). Furthermore, significantly more people in the Millennial Generation, the youngest sample, reported concentration difficulties (X24=13.012, P=.011), irritability (X24=22.676, P=.000), and depression (X24=13.266, P=.010). When comparing medical problems and histories, such as heart failure, acid reflux, and hypertension, it is expected that the geriatric or older generations would have the most health problems. While this was true for most medical system problems, there were no differences in the number of people with digestive system problems when comparing by traditional categories or generations. Surprisingly, the Millennial Generation had significantly more nervous system problems (X24=11.688, P=.020), such as autism or Down’s syndrome, and were significantly more likely to have been diagnosed with a psychological disorder (X24= 31.521, P=.000) than any other group. The next generation with the highest prevalence of psychological diagnoses was the Baby Boomer Generation. The Millennial Generation was significantly more likely to have a family history of sleep disorders than any other generation (X24=18.414, P=.001). This finding was consistent with results when comparing groups by traditional classifications; however, the percentage of people with a family history of sleep disorders steadily declined among older generations. Only 7% of those in the GI Generation, compared to 59% in the Millennial Generation, had a family history of sleep disorders.
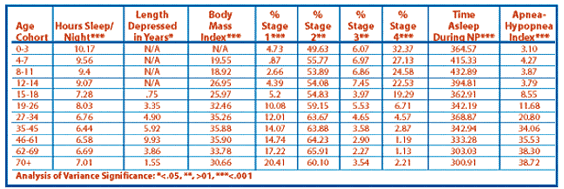
When groups were compared by age cohort, we found that proportionally more adults (92%) in the 35 to 45 age range reported snoring (X210=33.794, P=.000), while only 34% of those in the 15 to 18 age range reported snoring as a symptom of their sleep disturbance. Significantly more participants in the 27 to 34 group reported waking with a choking sensation (X210=28.172, P=.002); however, there were no differences among age cohorts in reporting cessation of breathing during sleep. More people in the 19 to 26 age group reported experiencing bizarre dreams (X210=35.902, P=.000), while more 15 to 18 year olds reported experiencing difficulties concentrating (X29=25.634, P=.002). This finding illustrates which portion of the Millennial Generation was most likely to report concentration problems. As previously mentioned, Generation X was the group most likely to have an accident or near accident from excessive fatigue. Analysis by age cohort revealed that those in the 27 to 34 age range of this population were significantly more likely to report this type of accident than any other group (X28=16.102, P=.041). Interestingly, proportionally more 12 to 14 year olds reported experiencing headaches (X210=44.978, P=.000), and were the least likely to report feeling rested upon awakening (X210=38.239, P=.000). When traditional classifications were used, adults were more likely to report headaches and were the least likely to feel rested. These findings underscore the importance of using more specific methods of age classifications. When using more detailed classification systems, findings that may not be revealed when comparing by broader divisions become apparent. See Tables 4 and 5 (page 63) for further significant differences in diagnoses and data from nocturnal polysomnography.
Table 4. Significant differences in diagnoses type: age cohort.
Discussion
Our analyses revealed both similarities and differences when comparing people with sleep disorders by specific age classifications. We found opposite, unexpected patterns, further emphasizing the critical need to explore age-specific characteristics in sleep disorders. For instance, there were significant differences in levels of obesity when comparing our population by the traditional age classifications. Adults were more likely to be obese than the children/youth or geriatric populations; however, when analyzing by generation, we found that obesity was much more prevalent in both the Boomer and X Generations of the adult sample. Without normal sleep, the pituitary gland does not release growth hormones effectively. Thus, while sleep disordered breathing has been linked to obesity in both children/youth and adults, children with sleep disorders also may be underweight and/or short in stature. By identifying specific age groups that are prone to obesity or weight irregularities, more preventative measures may be directed toward these groups.
Proportionally more children/youth in our sample had a nervous system disorder/abnormality and/or psychological disorder. When this is considered in conjunction with the increased family history of sleep disorders in this group, it seems that only a limited set of children/youth are being properly referred for diagnosis and treatment of sleep problems. This is alarming given the increased rates of psychological diagnoses in this population. We speculate that many children given a diagnosis of ADD/ADHD may have an underlying, undiagnosed SD and are, thus, unnecessarily medicated. This is unfortunate for many reasons. One of the most glaring is that the medications prescribed for ADD/ADHD may intensify sleep disorders. Across all age ranges, 34% of participants had been formally diagnosed with a psychological disorder; 52% of those with psychological disorders had depression, and an additional 34% had multiple diagnoses, such as anxiety disorder and depression. Across all ages, there may be an increase in the desire for the “quick fix” of pharmacological therapy, rather than being properly assessed for an underlying problem. Given that selective serotonin reuptake inhibitors, a common form of antidepressants, may further disrupt sleep, it seems imperative that increased awareness of the psychological effects of sleep disorders be attained. This could help prevent unnecessary medication of psychological problems while undiagnosed sleep disorders prevail and lead to further negative health risks.
Analyses also revealed differential diagnoses. Proportionally more geriatric participants were diagnosed with OSA, poor sleep efficiency, nocturnal hypoxemia, restless leg syndrome, and/or an abnormal sleep architecture. It was interesting to find that those in the 46 to 70+ age range were equally likely to be diagnosed with an abnormal sleep architecture. This finding clarifies the results of the traditional analysis that demonstrated the geriatric population was the most likely to receive this diagnosis, thus illustrating that starting at the age of 46 rather than 65, people are more prone to developing an abnormal architecture. Furthermore, while OSA was most common in the geriatric sample, age cohorts revealed that those ages 62 to 69 were more likely to receive this diagnosis, despite those in the 70+ group having the highest apnea-hypopnea index average. According to self-report, adults reported more snoring than did younger populations; nevertheless, a diagnosis of primary snoring was more prevalent in the children/youth population. Interestingly, children/youth spent less time in REM than did adults and the geriatric populations. Contrary to literature on normal populations indicating that children would be expected to experience greater levels of REM, our adult population spent significantly more time in this stage. Conversely, children/youth spent significantly more time in stages 3 and 4 of sleep. When analyzing by age cohort, differences in sleep architecture were found in all stages of sleep except REM.
Considering the numerous adverse effects of sleep disorders, it is important to properly assess and recognize sleep problems and their manifestations in all age groups. By raising awareness of sleep problems across the life span, more timely diagnosis and treatment may be obtained and hopefully reduce the many negative physiological and psychological implications of insufficient/disrupted sleep.
Pennie S. Seibert, PhD, is director of research, Idaho Neurological Institute at Saint Alphonsus Regional Medical Center, and professor, Psychology Department, Boise State University, Idaho; Tiffany A. Whitmore and Brian M. Dufty are co-coordinators of research, Idaho Neurological Institute; Nichole Whitener, RN, CNRN, is program coordinator, Idaho Neurological Institute; Fred P. Grimsley, RPSGT, CRT, is manager of the Sleep Disorders Center; and Janat O’Donnell, MD, ADSM, is a pulmonologist and medical director of the Sleep Disorders Center, all at Saint Alphonsus Regional Medical Center, Boise, Idaho.
References
1. Overview of the Findings of the National Commission on Sleep Disorders Research (1992). The Sleep Well Home Page. July 22, 1998. Available at: http://www.stanford.edu/ ~dement/overview-ncsdr.html. Accessed October 22, 2004.
2. Anstead M. Pediatric sleep disorders: new developments and evolving understanding. Curr Opin Pulm Med. 2000;6:501-506.
3. Chervin RD, Archbold KH, Panahi P, Pituch KJ. Sleep problems seldom addressed at two general pediatric clinics. Pediatrics. 2001;107:1375-1380.
4. Mindell JA, Owens JA, Carskadon MA. Developmental features of sleep. Child Adol Psychiatry Clin North Am. 1999;8:695-725.
5. Ayalon L, Liu L, Ancoli-Israel S. Diagnosing and treating sleep disorders in the older adult. Med Clin North Am. 2004;88:737-750.
6. Hoban JA, Chervin RD. Assessment of sleepiness in children. Semin Pediatr Neurol. 2001;8:216-228.
7. Pearl PL. Childhood sleep disorders: diagnostic and therapeutic approaches. Curr Neurol Neurosci Rep. 2002;2:150-157.
8. Chervin RD, Archbold KH. Hyperactivity and polysomnographic findings in children evaluated for sleep-disordered breathing. Sleep. 2001;24:313-320.
9. Picchietti DL, England SJ, Walters AS, Willis K, Verrico T. Periodic limb movement disorder and restless legs syndrome in children with attention-deficit hyperactivity disorder. J Child Neurol. 1998;13:588-594.
10. Smith R, Ronald J, Delaive K, Walld R, Manfreda J, Kryger MH. What are obstructive sleep apnea patients being treated for prior to this diagnosis? Chest. 2002;121:164-172.
11. 2003 Sleep in America Poll. National Sleep Foundation Web site. Available at: www.sleepfoundation.org. Accessed November 5, 2004.
12. Seibert PS, Whitmore TA, Jones CJ, O’Donnell JE, Grimsley FP, Zimmerman CG. Characterizing sleep disorders: male-female variations and similarities. Paper presented at: 18th Annual Meeting of the Associated Professional Sleep Societies; June 5-10, 2004; Philadelphia.