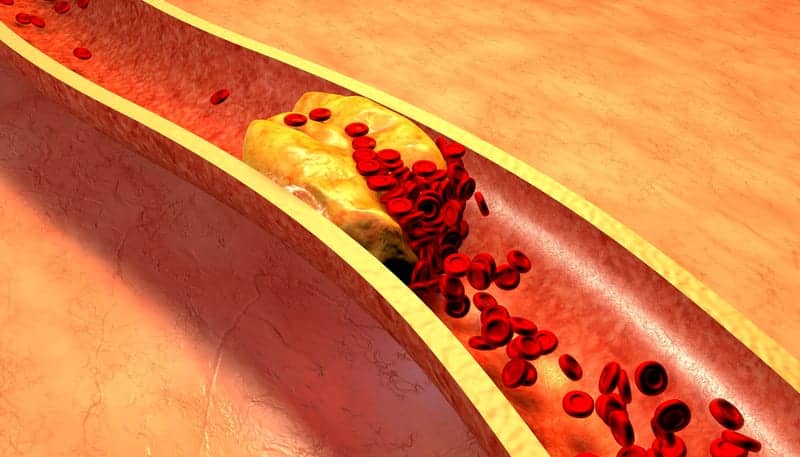
University of Helsinki researchers have found that sleep loss influences cholesterol metabolism.
A study, published in Nature, examined the impact of cumulative sleep deprivation on cholesterol metabolism in terms of both gene expression and blood lipoprotein levels. With state-of-the-art methods, a small blood sample can simultaneously yield information about the activation of all genes as well as the amounts of hundreds of different metabolites. This means it is possible to seek new regulating factors and metabolic pathways which participate in a particular function of the body.
“In this case, we examined what changes sleep loss caused to the functions of the body and which of these changes could be partially responsible for the elevated risk for illness,” explains Vilma Aho, researcher from the Sleep Team Helsinki research group, in a release.
The study established that the genes that participate in the regulation of cholesterol transport are less active in persons suffering from sleep loss than with those getting sufficient sleep. This was found both in the laboratory-induced sleep loss experiment and on the population level.
While analyzing the different metabolites, the researchers found that in the population-level data, persons suffering from sleep loss had fewer high-density HDL lipoproteins, commonly known as the good cholesterol transport proteins, than persons who slept sufficiently.
Together with other risk factors, these results help explain the higher risk of cardiovascular disease observed in sleep-deprived people and help understand the mechanisms through which lack of sleep increases this risk.
“It is particularly interesting that these factors contributing to the onset of atherosclerosis, that is to say, inflammatory reactions and changes to cholesterol metabolism, were found both in the experimental study and in the epidemiological data,” Aho says.
The results highlight the health impact of good sleep. The researchers emphasise that health education should focus on the significance of good, sufficient sleep in preventing common diseases, in addition to healthy food and exercise. Even a small reduction in illnesses, or even postponing the onset of an illness, would result in significant cost savings for society at large.
“The experimental study proved that just one week of insufficient sleep begins to change the body’s immune response and metabolism. Our next goal is to determine how minor the sleep deficiency can be while still causing such changes,” Aho states.
The Sleep Team Helsinki research group, led by Tarja Porkka-Heiskanen (Stenberg), MD, PhD, is studying the impact of sleep loss on immune defence and metabolism, particularly lipid and cholesterol metabolism. It has previously been established through epidemiological studies that people who sleep less than they should have a higher risk of contracting cardiovascular diseases, a higher risk of mortality from cardiovascular diseases, and a higher overall mortality over a set time span.
Cardiovascular diseases are known to be linked to both metabolism and the immune system. Sleep loss has been demonstrated to cause low-grade inflammatory state in the body, and this may contribute to the higher risk of disease. Carbohydrate metabolism has also been found to alter in sleep deficiency in ways that resemble type 2 diabetes.
However, the impact of sleep loss on lipid and cholesterol metabolism has been studied very little.
This study employed three data sets:
- Experimental SR study (N=21): An experiment conducted in cooperation with the Finnish Institute of Occupational Health under strictly controlled laboratory conditions, simulating a work week with restricted sleep.
- DILGOM (Dietary, Lifestyle and Genetic determinants of Obesity and Metabolic syndrome, N=518): A subset of the national FINRISK population study, collected to serve research into the risk factors for the metabolic syndrome.
- Cardiovascular Risk in Young Finns Study (YFS, N=2,221): A Finnish population study which followed the lifestyles and heart health of participants from childhood/youth. We used data from 2007, when participants were between the ages of 30 and 45.
These data sets were used in cooperation with the National Institute for Health and Welfare and the universities of Tampere and Turku, which were responsible for their collection and analysis. Metabolomic analyses were conducted at the University of Oulu. The research project also involved the Finnish Institute of Occupational Health and VTT Technical Research Centre of Finland.