Bed growth, patient volume growth, and per patient revenue all show declines in 1Q16.
Bed Growth Similar to Third Quarter 2015
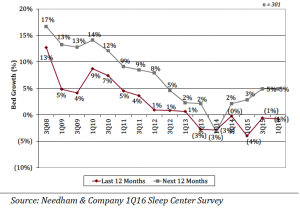
Over the last 12 months (LTM), average beds per respondent decreased slightly by 1% to 7.7 beds. But over the next 12 months (NTM), average beds per respondent are expected to increase by 5% from 7.7 beds to 8.1 beds. We note that 8% of respondents indicated that they have fewer beds now than they did 12 months ago. Bed growth was the same as our prior survey (3Q15), in which LTM bed growth was -1% and NTM bed growth was also 5%.
LTM, NTM Patient Volume Growth Slowed
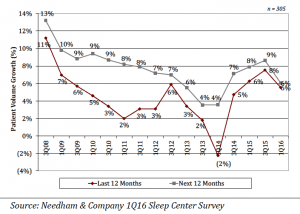
Over the LTM, respondents report patient volume growth of 6%. But over the NTM, respondents expect patient volume growth of 6%. Both the LTM and NTM growth rates slowed from 8% and 9%, respectively, in our prior survey (3Q15). The historical and expected patient volume growth rates are different from the historical and expected bed growth rates (which were -1% and 5%, respectively). We continue to believe that the divergence is due to increased use of home sleep testing (HST) by the sleep centers.
For the first time, we asked sleep centers “During a typical 7-day week, approximately how many patients have appointments at your sleep center?” Respondents answered as follows:
- Less than 30 patients per week: 44.0%
- Between 30 and 60 patients per week: 32.7%
- Between 60 and 90 patients per week: 8.4%
- Between 90 and 120 patients per week: 3.6%
- Over 120 patients per week: 8.4%
- Unsure: 2.9%
Per Patient Revenue Decreases Versus 1 Year Ago
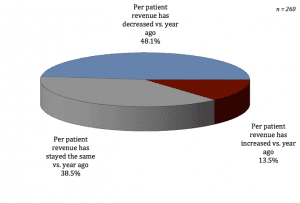
For the first time, we asked sleep centers, “How would you describe per patient revenue today compared to the same date 1 year ago?” Just under half (48.1%) reported that per patient revenue has decreased versus a year ago; 38.5% reported that per patient revenue had stayed the same versus a year ago; 13.5% reported that per patient revenue has increased versus a year ago.
Portion of Tests Done Via HST Same as Third Quarter 2015
The results of the survey show that on average 20% of OSA tests are done with HST rather than in-lab tests. This is in line with 20% reported in our 3Q15 survey. Over time, we expect this to continue to grow.
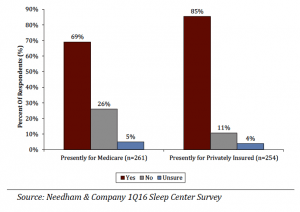
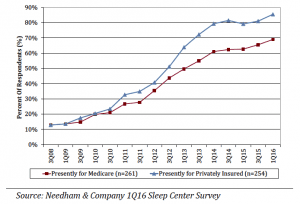
Currently, 85% of sleep centers offer HST for patients with commercial insurance compared to 69% that offer home testing for patients with Medicare. This was up from 81% and 66%, respectively, in our prior survey (3Q15) as sleep centers continue to adopt HST.
In two other questions about HST, 33% of respondents indicated that HST had negatively affected their expansion plans (versus 29% in our 3Q15 survey), and 51% of respondents indicated that they expect to increase involvement in HST (versus 55% in our 3Q15 survey).
APAP Use Stable, Bi-Level Use Decreased

What Percentage of Your Sleep Patients Use an Auto-Setting Flow Generator? Time Series (click to enlarge)

What Percentage of Your Sleep Patients Use a Bi-Level Flow Generator? Time Series (click to enlarge)
On average, respondents report that 19% of their patients use auto-setting flow generators (APAP) (in line with 19% in our 3Q15 survey), while 12% of their patients use bi-level flow generators (down from 14% in our prior survey). Over the longer term, utilization of APAP has steadily increased while utilization of bi-level devices has been relatively stable. Increased use of APAP is probably the result of increased use of HST, since APAPs do not require the patients to be titrated to determine the proper pressure setting. It’s less clear what is driving the recent decrease in use of bi-level devices though the results from the SERVE-HF trial could have reduced use of high-end servo-ventilation bi-levels.
Alternative Therapies
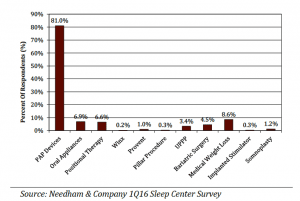
For the first time, we asked, “In the past 12 months, what percentage of your OSA patients has tried the following therapies?” Responses revealed that the majority (81%) of sleep apnea patients have tried PAP devices. Use of PAP devices was followed by use of medical weight loss (nonsurgical) by 8.6% of patients, use of oral appliances by 6.9% of patients, use of positional therapy by 6.6% of patients, and use of bariatric surgery by 4.5% of patients. The complete results to this question in descending order are as follows:
- PAP devices (81.0%)
- Medical weight loss without surgery (8.6%)
- Oral appliances (6.9%)
- Positional therapy (6.6%)
- Bariatric surgery (4.5%)
- Uvulopalatopharyngoplasty (UPPP) with or without tonsillectomy (3.4%)
- Somnoplasty (1.2%)
- Provent (1.0%)
- Implanted airway stimulation device (0.3%) (tie)
- Pillar Procedure (0.3%) (tie)
- Winx (0.2%)
The total surpasses 100%, as some patients may have tried (or currently use) more than one therapy.
In a separate question, we asked what percent of patients start their OSA therapy with an oral appliance. On average, 4.4% of patients start their OSA treatment with an oral appliance. This compares to 5.7% in our 3Q15 survey. We specified that these are patients who have never tried a CPAP device.
ASV Use for Complex Sleep Apnea Continues Decline
Since use of the adaptive servo-ventilator (ASV) devices peaked at 79% of complex sleep apnea patients in 1Q14, use of the ASV devices has steadily declined to 55% of patients in 1Q16. We suspect that the decline has been driven by the results from ResMed’s SERVE-HF trial that were disclosed in May 2015, although the trial was focused on patients with heart failure and central sleep apnea rather than complex sleep apnea. The ASV flow generator segment is important in our view because, while unit volumes are low, the products have very high prices and margins.
Number of HMEs Asking for Changes to Branded Prescriptions Slightly Higher
Around 22% of respondents indicated that they have been asked to make changes to branded prescriptions by HMEs due to competitive bidding. This represents an increase from 14% in our prior survey. On average, respondents indicated that 19% of the HMEs to which they refer patients have asked for changes to branded prescriptions. This is an increase from 13% in our prior survey.
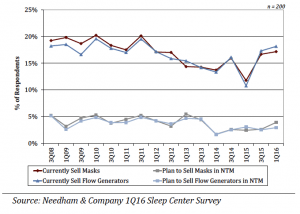
On average, sleep centers reported writing brand-specific prescriptions for 69% of mask prescriptions and for 54% of flow generator prescriptions. The rate of branded prescriptions had been relatively stable in recent years.
Continued Increase in Sleep Centers Selling CPAP
In this survey, 18% of sleep centers report selling CPAP equipment, up slightly from 17% in our 3Q15 survey. Roughly 4% expect to start selling in the next 12 months. Over time, the portion of sleep centers selling CPAP equipment has varied but has been increasing recently.
RVUs Per Year
For the first time, we asked sleep centers, “On average, approximately how many RVUs do your sleep centers’ physicians work per year?” Relative value units (RVUs) are a measure of value used in the United States Medicare reimbursement formula for physician services. Most of the respondents (68.9%) indicated they were unsure. Of those that selected from the multiple choice options, the answers ranged as follows:
- Less than 3,000 RVUs (5.8%)
- Between 3,000 and 4,000 RVUs (7.9%)
- Between 4,000 and 5,000 RVUs (6.3%)
- Between 5,000 and 6,000 RVUs (3.2%)
- Between 6,000 and 7,000 RVUs (3.2%)
- More than 7,000 RVUs (4.7%)
This averages to 4,449 RVUs per sleep physician, using “1,500” as the average for those who selected “less than 3,000 RVUs.”
About the Survey
Sleep Review and Needham & Company conducted a survey of US sleep centers. The survey received 283 responses received between January 23, 2016 and February 19, 2016. Sleep center directors/supervisors/managers (37% of respondents) and registered polysomnographic technologists (29% of respondents) were the most common types of respondents. Every US geographic region and 44 different US states were represented, with the Midwest (31% of respondents) most heavily represented.
Mike Matson, CFA, is senior research analyst at Needham & Company LLC. He is an expert on the medical technologies and diagnostics sector. Sree Roy is editor of Sleep Review.









Quite interesting results