Actigraphy is making its way back into the mainstream through its ease of use and ability to integrate easily within already existing systems and protocols.
In the investigation of sleep and its related disorders, there are situations that warrant an increased duration for recording data. Instead of an investigation confined to an 8-hour period of time, it may require days in order to gather enough data to complete a physiological picture. But it is impractical to try to polysomnographically record a patient for days on end (under conventional methodology), much less to get that many charges reimbursed.
But what if a recording device was made that was not only easy to wear, but could record for days on end? Actigraphy was first devised in the early 1970s. The basic principle of actigraphy is to correlate gross periods of time with either sleep or wake. The premise of the correlation is rather simple. When one is awake, there is considerable body and limb movement. On the other hand, when one sleeps, there should be a very minimal amount of discreet body movements.
There is little question that the “gold standard” for sleep medicine diagnostics is the polygraph. Unfortunately, though, there are situations where the polygraph becomes an impractical instrument. As the need for detecting apneas decreases, so does the number of channels needed in the recording device.
Imagine that a patient has come to a sleep disorders center complaining of insomnia. After reviewing the patient’s questionnaires and interviewing the patient, the sleep medicine physician concludes that there is little evidence for obstructive sleep apnea hypopnea syndrome or any other pathology that would negatively impact this patient’s sleep pattern. But this patient cannot sleep. Moreover, the patient has reported an inconsistent pattern of occurrence. Now what do you say? Actigraphy. The term has become more popular over the past few years to the point that one can hardly attend a sleep meeting without hearing the term mentioned. But what exactly is it?
The actigraph is a small device that records movements of the wearer. The device itself is basically an accelerometer coupled to a recording unit, the combination of which is commonly attached to a wristband. This setup can be comfortably worn for long periods of time.
To understand actigraphy, one must first understand the term “resolution.” When a sleep disorders patient is recorded on a polysomnograph,1 the recording generally runs anywhere from 6 to 10 hours.2 Within that 6- to 10-hour period, sleep stages are gauged on a resolution of 10 mm/sec (or a 30-second epoch), as this is the standard paper/tracing speed. And as anyone who records on paper will tell you, an 8-hour study can use as much as 960 feet of paper (the necessary length for calibration purposes not included). At the advent of computerized polysomnography, scorers faced the problem of keeping visual continuity on apneic events that exceeded the length of the screen (a 45-second-long apnea). Shortly thereafter, software engineers devised a means by which the data recorded on the storage media could be redisplayed under 10 mm/sec. Instead, scorers were given the opportunity to change the display from a 30-second epoch to as much as 300 seconds per screen view. By changing the time resolution with multiple epochs on screen, the viewer is afforded a greater level of clarity with respect to the respiratory and electromyography channels (a feature that was impossible on paper records without compromising the staging data). Additionally, this resolution change allowed the scorer to view these channels not only for each individual episode, but for a frequency of occurrence or potential pattern.
Actigraphy works in very much the same way. Rather than holding the resolution to look at time in terms of seconds, actigraphy looks at time in minutes and hours. By compressing the data, actigraphy can look at both larger periods of recording time and at a more specific recording site. As these units have a very specific function in monitoring motion, there are very few channels contained within. In recent years, other correlating data channels have been added to the recording units. One of the first items to be added to the digital actigraph was a light sensor; as the motion was detected, a correlation to light level could be assessed. Other recently added parameters include temperature and noise levels.2 Core body temperature is a critical component for the determination of an individual’s circadian cycle, thus correlation between temperature and the time of day, coupled with motion detection, provides the interpreter with considerable detail.
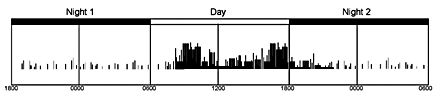
Figure 1. Normal progressions through the circadian cycle as seen with actigraphy. Note the movement indicators increase in correlation with the time of day and level of wakefulness. Likewise, there is a correlated decrease of indicators with the onset of sleep.
The actigraph is designed around the use of an accelerometer.1 In principle, the accelerometer measures the degree and intensity of the motion and then records the occurrence. For example, arm movements required to pick up objects or pull a door open are of a greater force than that which might be seen with a phasic twitch while in REM sleep. These units measure variable levels of motion from 0.05 g and up. Sampling rates are usually set at a frequency of 10 samples/second. Not only do these accelerometers measure acceleration, but deceleration as well. Once the motion has been made, the recording device of the actigraph denotes the action with a “tick” mark (see Figure 1, Night 1). During a patient’s sleep, there should be a very minimal amount of discreet body movements, in terms of both intensity and acceleration and deceleration. Conversely, a greater number of tick marks results in an increased number of movements, which happens to be the feature of alert wakefulness (see Figure 1, Day). Collectively, the recorded data is typically displayed in graphs representing a 24-hour or longer period of time. Yet with the versatility of the analysis software and its ability to redisplay the time resolution, isolated areas of the recording can be enlarged (or “exploded”) for a more definitive review of the data.
By stacking the graphs on the x-axis and keeping the y-axis timelines concentric, the active and inactive areas of a normal sleeper’s study should be in alignment on a day-to-day basis; however, in patients whose chief complaint is insomnia, the areas of activity will not align. The recordings of these patients often reveal times of activity late into the night, followed by infrequent inactive periods during what would otherwise be considered times of normal wakefulness.
Graphics
Another area of interest is in the graphics produced from a patient with pain association. These graphs tend to show a highly fragmented period in which the patient would otherwise be asleep. Reflecting the patient’s effort to make up for the previous night’s sleep loss, daytime hours reveal inconsistent periods of inactivity. Whether or not these sedentary periods are times in which the patient is “just resting” or they are truly asleep can be difficult to distinguish; nevertheless, normal daily waking function is impaired and can be attributed to the previous night’s disruption.
Recordings of patients afflicted with dementia illustrate the profound disruption in the circadian rhythm. The resulting graphics detail a highly irregular sleep-wake pattern that is marked by very short sleep periods, frequent arousals and awakenings, and an overall inability to maintain sleep any longer than in terms of minutes.
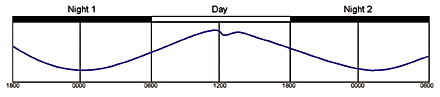
Figure 2. Normal progressions of sleep and wake through the circadian cycle.
The Role of the Actigraph
The primary role of actigraphy is in the study of the patient’s circadian rhythm1 (see Figure 2). And as such, this type of recording can be extended for days, possibly into weeks, in order to provide sufficient data. While a considerable amount of information can be obtained from the polysomnograph, the principal focus is broad in recording parameters and narrow in time duration. This is not to diminish the importance of the polysomnograph’s capabilities; however, the volume and depth of data over long periods of time are not necessary for circadian rhythm detections. An actigraph, on the other hand, offers a limited channel capability, yet can record as many as 44 days if necessary. In addition, the actigraph provides the patient with a smaller (newer models are the size and shape of a common wristwatch), portable recording device. And while the internal mechanics are highly sophisticated, the external appearance is simple and less obtrusive to wear.
Applications
The actigraph, by virtue of its portability, lends itself well to areas of study where the patient is less than accessible. A recent online search of actigraphy yielded multiple hits for sites with the National Aeronautics and Space Administration (NASA), in particular, STS-107, the last ill-fated mission of the Columbia shuttle. Listed within the assignment profile of Commander Laurel Clark, MD, as one of the many areas of interest for this particular mission, was “sleep-wake actigraphy and light exposure during space flight.”3 While NASA has successfully recorded multiple-physiological parameter sleep recordings, such as those in the 1998 Neurolab flights (STS-904 and STS-955), the use of actigraphy has become more popular for a variety of reasons. Again, as the issues of circadian rhythm and long-duration space flight have moved to the forefront, traditional polysomnograph methodology has become too cumbersome to be efficient. With its relatively small size and weight, an actigraph offers a viable method for recording sleep-wake/circadian rhythm in an environment in which light/darkness/ zeitgebers can be present in excess or absent. Potentially, the use of space flight could further elaborate the theories and outcomes produced in Nathaniel Kleitman’s 1953 Mammoth Caves sleep studies.
While the thrust of a complaint with insomnia is directed at the lack of sleep during the night, the overall effects carry through the 24-hour period. By viewing the actigraphy data over a 24-hour period, the physician is provided with a broad assessment of a full day’s normal activities rendered in the patient’s normal environment. In many cases, insomnia can occur on an infrequent day-to-day basis. Actigraphy offers a cost-effective method for studying patients for days on end. Not to discount short-duration (<10 hours) usage, actigraphy recordings via lower limb application can render reliable data needed for the diagnosis of restless legs syndrome and periodic limb movement disorder.2
Other applications of interest with actigraphy include treatment efficacy, evaluation of sleep phase alternations (jet lag), and post-offer employment screenings. Industrially, actigraphy provides both the employee and employer an assessment of potential sleepiness risk within nontraditional workplaces. If these issues can be addressed prior to placement, employee health and welfare can be maintained while lowering the employer’s accident liability. An example of such an application is in the trucking industry, specifically those operators who perform under a “just in time” delivery system. These systems tend to operate in a 24-7 environment, in which the individual drivers may be called out at any time of the day or night. Actigraphy in the trucking environment can be used to assess the resting periods during the “off hours,” thus confirming efficient use and quantification of break periods. It can also alert the drivers of otherwise unknown sleep disturbances that could have a negative effect on performance and safety.
Actigraphy offers the sleep medicine physician a viable tool as an adjunct to the traditional laboratory setting. As the population has grown increasing mobile, actigraphy adapts in its portability and comfort. For the sleep technologist, this device is easy to use as it integrates easily within already existing systems and protocols.
It appears that actigraphy is making its way into the mainstream. No longer is it the tool of academia, but rather a practical assessment tool with a clinical application. The benefits of actigraphy are now coming to the forefront.
Allen Boone, RPSGT, is director, Integrated Sleep Resources Inc, Jacksonville, Fla.
References
1. Ancoli-Israel S, Cole R, Alessi C, Chambers M, Moorcraft W, Pollack C. The role of actigraphy in the study of sleep and circadian rhythms. American Academy of Sleep Medicine Review Paper. Sleep. 2003;26:342-392.
2. Edwards K. Actigraphy. In: Lee-Chiong T, Sateia M, Carskadin M, eds. Sleep Medicine. Philadelphia: Hanley & Belfus; 2002:689-696.
3. Space Shuttle Columbia and her crew. National Aeronautics and Space Administration Web site. Available at: http://www.nasa.gov/columbia/crew/profile_laurelc.html. Accessed March 1, 2004.
4. Available at: http://www.neurolab. jsc.nasa.gov/timeline.htm. Accessed March 1, 2004.
5. Clinical trial of melatonin as hypnotic for space crew (Sleep-2). Shuttle Press Kit Web site. Available at: http://www.shuttlepresskit.com/STS-95/experiment45.htm. Accessed March 1, 2004.






