 |
Excessive daytime sleepiness (EDS) in adolescents presents a wide spectrum of differential diagnoses, in terms of both primary sleep disorders as well as those occurring secondary to medical and psychiatric conditions.1 The case of a 17-year-old male who fell asleep at the wheel and crashed his car stresses the need to take a full sleep and medical history in young adolescent males.
BACKGROUND
Probably the most widely encountered sleep problem in adolescence is that of insufficient sleep. Studies across populations have consistently shown that school-going adolescents sleep less during the week with extended sleep at weekends and during vacation.1 Inadequate sleep not only leads to EDS but also can have long-term effects on neurocognitive functioning, academic and work performance behavior, mood, and, more importantly, driving. In adolescents and young adults, motor vehicle crashes are a leading cause of death. Crashes caused by the driver falling asleep were most likely to occur in drivers between the ages of 16 and 29 years.2-5 Crashes in the 25 years or younger age group generally take place at night and involve males driving alone and going off-road.5
Despite insufficient sleep being a major problem in adolescence, it is essential to consider other causes of EDS and take a formal sleep history when faced with this problem. For instance, 7% of the adolescent population is said to suffer from the delayed sleep phase syndrome, which may be exacerbated by environment and lifestyle.1 The symptoms of narcolepsy often appear during adolescence and young adulthood, although the diagnosis may be delayed for many years due to poor recognition of the syndrome. Excessive caffeine intake and substance abuse also may contribute to sleep problems although the prevalence of this is currently unknown.
|
Subscribe to Sleep Report to receive updates about fatigue and drowsiness research |
PATIENT CASE
A 17-year-old man presented to the clinic with his mother after crashing his car. He had fallen asleep at the wheel and been referred urgently by his general practitioner.
He had driven for 1 hour in the late afternoon without a break, prior to crashing. He denied feeling tired prior to the event and denied suicidal ideation. There was no history of substance or alcohol misuse nor of food consumption at the time. No serious injuries were sustained as a result of the accident.
On further questioning, he had been excessively sleepy since the age of 14 years. On several occasions, he had fallen asleep standing up, during class, and during exams. He stated that he could fall asleep within seconds if not concentrating on a task. His naps lasted for a few minutes only, and he always awakened refreshed. At lunchtime, he took a nap of 20 minutes and again in the evening on a regular basis. Nocturnal sleep was not disrupted. He described marked hypnagogic hallucinations at least once a month, both visual and auditory, but denied sleep paralysis and cataplexy. His Epworth Sleepiness Score (ESS) was 18/24 and his mother scored him at 17/24. The Epworth Sleepiness Score is a subjective questionnaire-based measure of sleepiness with a maximum score of 24.6 He retired between 10 and 11 pm every night and got out of bed at 8:30 to 11 am. However, being a student at university, he admitted to an irregular sleep/wake schedule on occasion.
Specific questioning about snoring revealed that he snored minimally but that it had been a feature since childhood. No apneas had ever been witnessed by co-sleepers or parents. He had a dry mouth in the morning and nocturia. There was no history of parasomnias and no family history of sleep disorders. His significant medical history revealed an allergy to peanuts, which had previously led to anaphylactic reactions. Despite this, he did not carry an Epipen™ with him. He was a nonsmoker and denied alcohol or recreational drug use. There was no significant family history of illness.
On examination, he was tall and slim, but not marfanoid. He had a height of 1.91 meters and a weight of 85.7 kg, giving him a BMI of 24 kg/m2. His blood pressure was 120/70 mm Hg sitting. Cardiorespiratory and neurological examinations were normal. Examination of upper airway and nose revealed a narrow arched palate, the presence of allergic rhinitis, massive tonsillar hypertrophy, bilateral mucopurulent nasal discharge, a polypoidal middle turbinate, and obstruction at the palatal level due to massive tonsillar hypertrophy.
DIAGNOSIS
The patient underwent overnight polysomnography in our sleep laboratory (Figure 1). Results showed a total sleep time of 6 hours and 45 minutes. He had a sleep efficiency of 84.7%. His awake Spo2 was 96% on average and his nadir desaturation was 90%. His apnea/hypopnea index (AHI) was recorded as 55.6 events per hour consistent with severe sleep-disordered breathing. There was no early onset REM sleep, no periodic limb movements, and no abnormal movements consistent with a parasomnia.
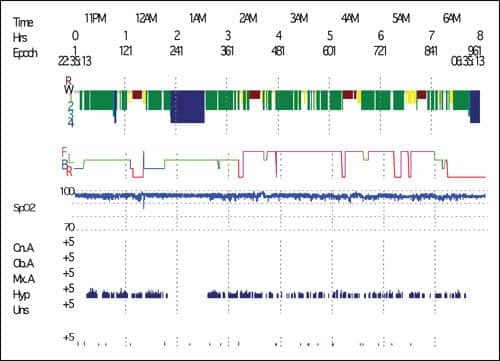 |
| Figure 1. Polysomnography showing severe sleep-disordered breathing. |
TREATMENT
He was diagnosed as having severe obstructive sleep apnea/hypopnea syndrome (OSAHS) due to lymphoid tissue overgrowth and was commenced urgently on continuous positive pressure therapy (CPAP). While he was on treatment, his ESS came down to 11/24.
He was referred to the ENT surgeons who performed a tonsillectomy and removed the uvula, which showed a benign squamous papilloma. He stopped CPAP postoperatively. His ESS came down to 5/24 with resolution of all symptoms. His postsurgical PSG revealed complete resolution of his sleep-disordered breathing (Figure 2). Additionally, the patient was issued with an Epipen for emergency use and referred to an allergologist.
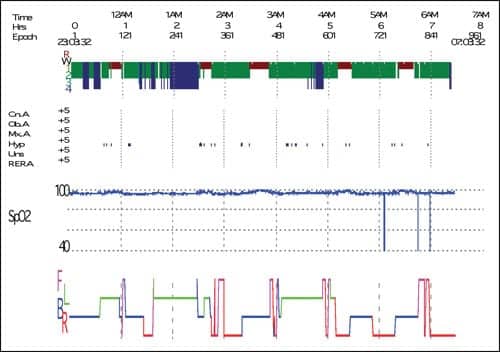 |
| Figure 2. Polysomnography post ENT surgery showing resolution of sleep-disordered breathing. |
DISCUSSION
The obstructive sleep apnea/hypopnea syndrome is defined on the basis of symptoms of daytime sleepiness and objective measures of disordered breathing during sleep. Sleep-disordered breathing in OSAHS is characterized by episodes of pharyngeal obstruction, which are termed apneas if complete and hypopneas if partial. Apnea is defined as a cessation of airflow for at least 10 seconds. Apneas/hypopneas are often, but not always, associated with an electroencephalographic arousal at their termination and with a drop in oxygen saturation.7 Controversy remains regarding a standardized definition of hypopnea, but the definition adopted by the American Academy of Sleep Medicine (AASM) is a 50% reduction in thoracoabdominal movement for at least 10 seconds from the preceding stable baseline when asleep.7
OSAHS affects approximately 2% to 4% of the middle-aged population. In adolescents, the true prevalence of SDB and OSAHS is unknown. There is a lack of studies in this area, in addition to the lack of consensus about minimum diagnostic criteria.
In younger children, an AHI of 1 event or greater per hour is considered diagnostic of SDB; this threshold may not be appropriate in older children and adolescents. One study has shown that an AHI of up to 3.6 events/hour is normal in young boys.8
The more common causes of OSAHS in the teenage group are likely to reflect those of both children and adults. In prepubertal children, the most common cause of SDB is adenotonsillar hypertrophy, whereas obesity appears to account for the majority of SDB in adults.9 However, there are a large number of other factors that contribute to the expression of SDB in these populations, including subtle craniofacial changes, possible problems with neuromuscular control of the pharynx, hormonal status, and the impact of acquired conditions, environment, and lifestyle in adults.
History and clinical examination alone (including blood pressure and BMI) can predict the presence of OSAHS in only 50% of adult patients attending a sleep disorders clinic.10 Definitive diagnosis requires overnight investigation of breathing patterns, and this applies to pediatric and adolescent groups as well.
In terms of treating OSAHS, CPAP is considered the first choice in patients with moderate-to-severe OSAHS.11,12 However, CPAP treatment effectiveness is limited by variable adherence to therapy, which has been found to range between 46% and 83% in adult OSAHS patients.13
Although surgery per se is not routinely advocated in the treatment of OSAHS14, in the case presented, it effected a cure. If SDB is secondary to lymphoid tissue hyperplasia, current guidelines advocate surgery.15 However, the evidence on which this is based is limited, and at present, there is only one randomized controlled trial in children that examined radio-frequency ablation of adenotonsillectomy (AT) tissue versus surgical removal.16 There are no such trials in adults, and there have been no trials in either population comparing CPAP versus AT.14 AT is considered curative in children (75%–100%, including the obese), but it has also been established that severe OSAHS preoperatively and persistent postoperative snoring are risk factors for persistent OSAHS.9,15 The high cure rate quoted has recently been challenged and the need for additional treatments that complement AT proposed.9,16 Therefore, follow-up is recommended. In adults, there has been only one prospective trial on AT to date, which included only nine subjects.17
Despite this lack of formal evidence, it is important to consider surgery on an individual basis if patients have a potentially correctable structural issue resulting in OSAHS.
The investigation and management of EDS in adolescence are not always straightforward, and as this case illustrates, primary sleep disorders can go undetected for many years with potentially lethal consequences. Every patient who presents with EDS should have a structured sleep and medical interview with investigation and treatment directed at reversible causes. What is also clear is that much more work needs to be done in the area of adolescent sleep medicine.
Renata L. Riha, MD, BMedSc, RPSGT, MBBS, FRACP, FRCPE, is a consultant in Sleep and Respiratory Medicine at the Royal Infirmary, Edinburgh, and an Honorary Senior Lecturer at the University of Edinburgh. She qualified in medicine at the University of Queensland and completed her specialist training in respiratory and sleep medicine in Australia. She is a Fellow of the Royal Australasian College of Physicians and a Fellow of the Royal College of Physicians in Edinburgh where she also did her MD in the genetics of the obstructive sleep apnea/hypopnea syndrome. She is active in sleep research as well as pursuing clinical work. She can be reached at [email protected].
REFERENCES
- Millman RP. Excessive sleepiness in adolescents and young adults: causes, consequences, and treatment strategies. Pediatrics. 2005;11:1774-1786.
- Horne JA, Reyner LA. Sleep related vehicle accidents. BMJ. 1995;310:565–567.
- Maycock G. Sleepiness and driving: the experience of UK car drivers. J Sleep Res. 1996;5:229–237.
- Knipling RR, Wang JS. Crashes and Fatalities Related to Driver Drowsiness/Fatigue. NHTSA Research Notes. Washington, DC: National Highway Traffic Safety Administration; 1994.
- Pack AI, Pack AM, Rodgman E, Cucchiara A, Dinges DF, Schwab CW. Characteristics of crashes attributed to the driver having fallen asleep. Accid Anal Prev. 1995;27:769–775.
- Johns MW. Reliability and factor analysis of the Epworth Sleepiness Scale. Sleep. 1992;15:376–381.
- Sleep-related breathing disorders in adults: recommendations for syndrome definition and measurement techniques in clinical research. The Report of an American Academy of Sleep Medicine Task Force. Sleep. 1999;22:667–689.
- Acebo C, Millman RP, Rosenberg C, Cavallo A, Carskadon MA. Sleep, breathing, and cephalometrics in older children and young adults. Part I—normative values. Chest. 1996;109:664–672.
- Praud JP, Dorion D. Obstructive sleep disordered breathing in children: beyond adenotonsillectomy. Pediatr Pulmonol. 2008;43:837-843.
- Hoffstein V, Szalai JP. Predictive value of clinical features in diagnosing obstructive sleep apnea. Sleep. 1993;16:118-122.
- Lam B, Sam K, Mok WY, et al. Randomised study of three non-surgical treatments in mild to moderate obstructive sleep apnoea. Thorax. 2007;62:354-359.
- Sanders MH, Montserrat JM, Farré R, Givelber RJ. Positive pressure therapy: a perspective on evidence-based outcomes and methods of application. Proc Am Thorac Soc. 2008;5:161-172.
- Weaver TE, Grunstein RR. Adherence to continuous positive airway pressure therapy: the challenge to effective treatment. Proc Am Thorac Soc. 2008;5:173-178.
- Sundaram S, Bridgman SA, Lim J, Lasserson TJ. Surgery for obstructive sleep apnoea. Cochrane Database Syst Rev. 2005 Oct 19;(4):CD001004.
- Won CH, Li KK, Guilleminault C. Surgical treatment of obstructive sleep apnea: upper airway and maxillomandibular surgery. Proc Am Thorac Soc. 2008;5:193-199.
- Kuhle S, Urschitz MS, Eitner S, Poets CF. Interventions for obstructive sleep apnea in children: a systematic review. Sleep Med Rev. 2009;13:123-131.
- Verse T, Kroker BA, Pirsig W, Brosch S. Tonsillectomy as a treatment of obstructive sleep apnea in adults with tonsillar hypertrophy. Laryngoscope. 2000;110:1556-9.





