The guideline lowers the blood pressure cutoff. Sleep clinicians should pay attention to how sleep apnea therapies impact hypertension, and vice versa.
The new hypertension guideline from the American College of Cardiology and the American Heart Association was released in November 2017. Since its release, the way physicians diagnose and treat high blood pressure has changed. Have you seen this new guideline yet?1
What is exciting for dental sleep medicine specialists is the section (5.4.4) in the guideline dedicated to sleep apnea. Let’s take a look at what the guideline says about sleep apnea and what dentists can do to help.
How Has the Hypertension Diagnosis Changed?
The new guideline lowers the blood pressure cutoff for a hypertension diagnosis from 140/90 mm Hg to 130/80 mm Hg. And instead of using the term “prehypertension,” it recommends using “stage 1 hypertension” for levels of 130 to 139 mm Hg systolic or 80 to 89 mm Hg diastolic pressure, and “elevated” for 120 to 129 mm Hg systolic and diastolic of less than 80.
Despite the new levels in this guideline, it does not mean patients who have now been classified with hypertension will face dramatic new risks. It also does not mean that physicians will need to immediately begin medication treatment for many new patients. This new classification and guideline is intended to prevent strokes, heart attacks, and other cardiac problems through earlier action, possibly including a combination of lifestyle changes for all patients and medications for some to control high blood pressure.
What Does the Guideline Say About Sleep Apnea?
Obstructive sleep apnea (OSA) is a risk factor for several cardiovascular diseases, including hypertension, coronary, and cerebrovascular diseases. Studies have shown that the presence of OSA is associated with an increased risk of hypertension. It has also been hypothesized that treatment for OSA will have more pronounced effects on blood pressure reduction in resistant hypertension.
The guideline specifically mentions CPAP therapy as a successful form of treatment. But we can still look to oral appliances to play an important role as well. Studies that have looked at the effects of CPAP on blood pressure (BP) have demonstrated only small improvements in BP. The results were dependent on the patient’s compliance with CPAP use, severity of OSA, and presence of daytime sleepiness.2
As you know, many patients are noncompliant to CPAP therapy, which is often when an oral appliance can be prescribed and used. It helps to provide these patients with an alternative to not only treating their sleep apnea, but also possibly improving their BP.
What Does This Mean for Dentists?
This means we need to be extra cautious for our patients. Now that the level for hypertension has lowered, we need to pay attention to how that affects sleep apnea and vice versa.
Through the guideline, we can accept that CPAP therapy is an option, but what about oral appliance therapy? The number of individuals with hypertension is now at almost 50%. This higher number means we need to pay closer attention to OSA and how it affects hypertension.
An important goal for sleep apnea treatment is to lower a person’s blood pressure as well. In a study from the journal JAMA, researchers completed a systemic review and analysis of several published studies that look at different treatment techniques and their impact on reducing high blood pressure. They found that oral appliances work just as well as CPAP in reducing blood pressure.3 And a study published in the journal Sleep also found that oral appliance therapy can reduce high BP in patients.4
So, as a dentist, what can you do with this information? You can talk to your patients, include information on the health questionnaire you employ, and provide educational materials. This will help you to continue to provide your patients with the care they need and deserve.
It is also important that you continue to advance your education. By attending seminars, lectures, and online courses, you can remain up-to-date with important information on OSA and hypertension.
Mayoor Patel, DDS, MS, is the owner of Atlanta’s Craniofacial Pain and Dental Sleep Center of Georgia.
References
1. Reboussin DM, Allen NB, Griswold ME, et al. Systematic review for the 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: a report of the American College of Cardiology/American Heart Association task force on clinical practice guidelines. J Am Coll Cardiol. 2018 May 15;71(19):2176-98.
2. Iftikhar IH, Hays ER, Iverson MA, et al. Effect of oral appliances on blood pressure in obstructive sleep apnea: a systematic review and meta-analysis. J Clin Sleep Med. 2013;9(2):165–74.
3. Bratton DJ, Gaisl T, Wons AM. CPAP vs mandibular advancement devices and blood pressure in patients with obstructive sleep apnea: a systematic review and meta-analysis. JAMA. 2015;314(21):2280-93.
4. Gotsopoulos H, Kelly JJ, Cistulli PA. Oral appliance therapy reduces blood pressure in obstructive sleep apnea: a randomized, controlled trial. Sleep. 2004 Aug 1;27(5):934-41.




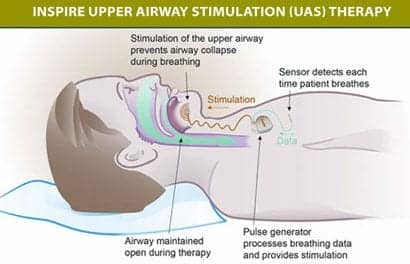


This does not include the new device for Sleep Apnea. Inspire Sleep therapy is FDA approved and I have one. It is a remarkable advancement in Sleep Apnea treatment and has taken my AHI from 28.5 to 4.
I was diagnosed with OSA in 1986. I was given UPPP surgery which removed my tonsils and adenoids along with part of my upper palate to remove “obstruction”. The surgery was not successful. In 2006 I had another sleep study which showed I still suffered from OSA. CPAP was next. I was not compatible with CPAP either. Another sleep study in 2017 showed OSA with an AHI of 45. At that point, Inspire therapy was suggested. I underwent the implant in April of 2018. I no longer stop breathing in my sleep. My former snoring which would have shook buildings is nearly non-existent.
THANK GOD for Inspire!
A major shortcoming in this discussion is the lack of information about the implant device Inspire. I was diagnosed with severe OSA in 1995 through an overnight in-clinic sleep test. My AHI was 50. I went through a multitude of different CPAP models until January 2016 when I had Inspire implanted. So, I’ve been using the Inspire device for 2 and a half years, and my AHI is 3. Now when I travel or go backpacking, I only have to pack my remote for activating and deactivating my Inspire. Not every OSA sufferer will qualify for Inspire, but I did and it has greatly improved my life. btw, the implant procedure is outpatient surgery.
I have never had hypertension but want to mention that Inspire has been a very successful treatment for my severe Obstructive Sleep Apnea. I was unable to tolerate a CPAP machine and did not receive significant benefit from an oral device. As a matter of fact, the “retainer-like” device added to residual nerve damage pain from a previous injury. I was hit in the right temple by a Major League foul ball causing damage to my eye, sinuses, and cheek. Long story short, my Inspire device was like a miracle!