
Barry Krakow, MD, and Laura Togami, general manager of Maimonides, review the latest PTSD Sleep Clinic pamphlet for new patients.
Is the Maimonides PTSD Sleep Clinic that opened in Albuquerque, NM, in March a vision of the future? Barry Krakow, MD, its founder, certainly hopes so.
The clinic exists inside Krakow’s already well-established Maimonides Sleep Arts & Sciences Ltd sleep center and nightmare treatment clinic, but is unique by focusing specifically on treating sleep disorders in patients with posttraumatic stress disorder (PTSD).
The occurrence of sleep disturbances such as nightmares and insomnia is, of course, one of the diagnostic criteria for PTSD, and the PTSD Sleep Clinic offers the cognitive behavioral therapy and imagery rehearsal therapy that researchers, including Krakow, have shown can ease nightmares in PTSD patients. However, they also take a holistic view of patients and ask what other factors might be disrupting the patients’ sleep, including sleep-disordered breathing, restless leg syndrome, or circadian rhythm disorders.
Incoming chronic insomnia patients routinely undergo a sleep study at Maimonides, and Krakow says approximately 70% end up having an apnea-hypopnea index (AHI) greater than 5 and another 20% have upper airway resistance syndrome. In other words, about 90% of insomnia patients present with some form of comorbid sleep-disordered breathing, a condition Krakow, along with fellow researcher Dominic Melendrez, termed “complex insomnia” in 2001. Krakow sees similar rates among incoming PTSD patients, which may explain why the standard approach to treating PTSD-related sleep disturbance was not working for them, and why many of these patients report so much frustration in working on their sleep problems with many well-intentioned PTSD therapists.
“We ask our new PTSD patients how they arrived at our clinic and it is not unusual to get the raised eyebrow or turned down lip that says, ‘Boy, you don’t know what it took to get here,'” Krakow says.
OUT OF THE BOX THINKING
Krakow believes that the conventional approach to treating PTSD-related sleep problems is failing many patients because the doctors they are seeing are locked into the conventional belief that PTSD-related sleep problems will resolve by themselves as soon as the primary problem, the psychological trauma, is successfully treated.
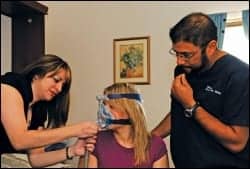
Jessica Sanchez, RPSGT, Maimonides lead tech (left), and Victor Ulibarri, RPSGT (right), prepare a patient for a PAP-NAP, a technique designed to help PTSD patients ease into PAP therapy.
“The problem we face is that many doctors seem misdirected by the concepts we call conventional wisdom,” Krakow says. “Conventional wisdom leads to inertia in the way people think, and it eventually leads them to a barrier about new wisdom, new ideas, and new knowledge.”
Thinking outside of the box, in contrast, forces one to question every assumption and belief. What if a patient’s inability to sleep well is a comorbid condition instead of merely a secondary symptom of the PTSD? What if many nights of disturbed sleep could actually cause physiological changes in some patients predisposed toward sleep-disordered breathing and lead to them developing this condition?
“Thinking outside of the box comes with a certain level of emotional risk, and you have to come to a place where emotionally you are ready to do that,” Krakow says. “In the late 1980s and early 1990s, I noticed that conventional wisdom in a number of areas was leading to bad outcomes and actually hurting people. The obvious question arose: why were standard treatments not working for so many of these patients? And why were so many PTSD patients who complained about their nightmares not receiving treatment for them?”
The conclusion Krakow drew was that both patients and doctors were not even thinking about treating the nightmares because they were locked into thinking about nightmares as just a symptom and not a treatable problem in its own right.
“For 20 years, I have been fortunate to hold in my mind’s eye this one particular out of the box perspective about nightmares, and that has helped me a great deal in trying to observe other things in sleep medicine that have not quite reached the ‘tipping point,'” Krakow says. “What drives me is knowing that there is a treatment called imagery rehearsal therapy that works for nightmares yet realizing that the vast majority of psychiatrists and psychologists don’t use it and don’t think there is any reason to use it because nightmares are still perceived as a secondary symptom. It allows me to keep saying, ‘Well, if that is one thing where people follow conventional wisdom and it doesn’t work, I wonder whether there are more things that are being followed that don’t work.'”
For example, Krakow has just published two research articles on people with chronic insomnia who do not respond to prescription sleeping pills and found that 70% suffer from complex insomnia, but he states, “We’re still not close to the tipping point on the recognition of high rates of sleep breathing problems, especially UARS, in these types of patients.”
INSIDE THE CLINIC

Linda Trujillo, RPSGT, nightmare treatment health educator (right), follows up with Susan Smith in the PTSD Sleep Clinic.
Having learned about Krakow and his methods through his books, his media appearances, his Web site, his blog, his online videos, or his social media presences on Twitter and Facebook, patients are finding their way to him from faraway places in and outside the United States, and some are paying out of pocket for treatment they can’t find elsewhere. However, Krakow primarily started the clinic as a model to learn and measure what could be achieved by integrating sleep medical treatments for trauma survivors rather than simply as a way to meet patient demand.
“We would love to see the PTSD Sleep Clinic grow so big that it is one of the major aspects of what we do because there are so many people who suffer from posttraumatic stress,” he says. “But in addition to that, we would be very excited to do workshops around the country, in particular with other sleep centers that would like to open up their own PTSD Sleep Clinic or their own nightmare clinic or both. Obviously, the people who will be most interested in this approach are the people who have some type of behavioral sleep medicine program in their operations now or they are anticipating a behavioral sleep medicine program. But there may be other doctors, such as a sleep facility that has a psychiatrist working there who knows about PTSD and would like to open up a PTSD Sleep Clinic.”
Adopting imagery rehearsal therapy is in many ways a natural fit for physicians focused on behavioral sleep medicine treatment, and they have been rapid adopters, Krakow says. However, he also reaches out to all clinicians in all disciplines, psychiatric hospitals, military mental health centers, companies that want to improve employees’ sleep, and, perhaps most important, patients themselves.
“Every day I’m involved with patient care because I run a sleep center, and I have been humbled by the knowledge that patients are much more intelligent than we were led to believe in medical school,” Krakow says. “The participatory medicine side of patient care made me realize that as much as I enjoy engaging with psychiatrists, psychologists, and other sleep doctors, there’s no predicting how close or far they may be from a tipping point in their embrace of new sleep medicine ideas and treatments. But a patient has a very different motivation. Every patient is eager to have the answers and not have the condition anymore that is driving them crazy. Whether it is sleep deprivation, nightmares, sleep apnea, PTSD sleep disturbances, or whatever, these people desire the information in a very passionate way.”
New patients at the PTSD Sleep Clinic fill in a free online survey to assess the degree to which their disturbing dreams are interfering with their quality of life along with extensive details about their sleep. If the results of the survey indicate that they may benefit from seeing a sleep specialist, they can ask their physician for a referral to a local sleep medicine specialist or choose to come to New Mexico for treatment at Krakow’s clinic.
At the Maimonides PTSD Sleep Clinic, they often start with a clinic appointment to learn imagery rehearsal therapy. In addition, they routinely undergo at least one sleep study to look for underlying sleep disorders that could complicate their PTSD treatment. Like some sleep centers, Maimonides takes care to offer a patient-centered sleep lab setting with a welcoming and relaxing atmosphere to reduce the feeling of being in a sterile environment.
The behavioral therapy is closely integrated with treatment of any physiological problems so that the overall balance for the majority of patients is equally weighted between treatment of the mind and the body. Although the clinic strives to find a medication-free resolution to the disturbed sleep, if a sleep movement disorder is detected, Krakow will prescribe medication to reduce these involuntary movements, which then allows the cognitive behavioral therapies to work better.
If the polysomnogram detects sleep-disordered breathing—as it does in a majority of cases—the patient is prescribed and fitted with a bi-level PAP, or, more typically, an auto bi-level PAP or adaptive servo ventilation (ASV) device.
Krakow is a believer in evidence-based medicine, and all the treatments offered in his PTSD Sleep Clinic are evidence-based. However, until more research is done on sleep-disordered breathing patients with the types of psychological conditions he sees, he is sticking with his clinical experience in what works with his patients—and for himself. Krakow also uses an ASV device.
“I’ve tried seven or eight devices since I went on PAP in 2002,” he says. “I was on a dental appliance for about 4 years prior to that.”
LONG DAY’S JOURNEY INTO SLEEP
It was not being diagnosed with sleep-disordered breathing, however, that led Krakow to sleep medicine. That came later. Rather he came to the field through his love of writing.
Board-certified in internal medicine, Krakow had been working in emergency medicine in Albuquerque while also writing fiction and journalism pieces. He wrote two novels and cowrote four screenplays and one book on golf instruction. “Fortunately, my day job put food on the table,” he says.
However, in 1988, when a newspaper editor asked him to write an article about the work of a couple of researchers at the University of New Mexico who were seeking participants for a study on nightmares, something clicked. He soon began working with Joseph Neidhardt, MD, and Robert Kellner, MD, the researchers he’d originally been sent to write about, on a book about nightmare treatment. Published in 1992, Conquering Bad Dreams and Nightmares formally introduced imagery rehearsal therapy to the fields of sleep medicine and dream studies.
“The nightmare work really got my attention and led me into other areas of medicine and one area was, of course, mental health. The other area of medicine that emerged was sleep, and I started going to the sleep conferences and just fell in love with the field. I was excited about how much psychiatry and mental health overlapped with sleep medicine, and that made the choice easy. And, ever since 1990, my work has focused on mental health patients with sleep disorders.”
Krakow became board-certified in sleep medicine in 1994 and says he could have opened up a PTSD Sleep Clinic 10 or even more years ago. However, the resources were just not there yet to put it all together. Two instrumental factors helped pave the way. First, he and his wife Jessica Krakow (the CEO of Maimonides Sleep Arts & Sciences, Ltd) cowrote Turning Nightmares into Dreams, an audio series and workbook for chronic nightmare patients. Then, in 2007, Sound Sleep, Sound Mind was published, a book that encompasses Krakow’s vision of “Sleep Dynamic Therapy.”
“Once that book was written, we were able to start the nightmare treatment clinic and give patients more resources to appreciate the complex nature of their sleep problems. After a couple of years of developing this clinic, we realized that the concept of the PTSD Sleep Clinic was a more natural, meaningful, and accurate name for what we were offering to our patients,” he says.
LISTENING TO MAKE THINGS BETTER
What Krakow brings to treatment development is creativity and a somewhat unique ability to really listen to patients and then take that feedback and modify the planned treatment, says Patricia Haynes, PhD, a treatment development researcher at the Southern Arizona VA Health Care System and University of Arizona Department of Psychiatry and Psychology.
“Barry is constantly coming up with new ideas and new strategies and new ways to develop treatments,” Haynes says. “There are a lot of doctors who are great at listening, but Barry listens and then modifies his treatment to be better.”
Krakow’s hope is that the PTSD Sleep Clinic may influence others to make treatments better for trauma patients.
“We are persuaded that many people with PTSD have sleep problems and the sleep problems are not being fully addressed,” Krakow says. “It is nice to see that some trauma survivors are pushing for more treatment options, but it would be important to see more doctors recognizing the value of a sleep medicine center in helping to treat PTSD patients.”
Lena Kauffman is a freelance writer in Ann Arbor, Mich. She can be reached at [email protected].






