By Roberta M. Leu, MD
It is well known that adults with obstructive sleep apnea (OSA) can suffer from neurocognitive dysfunction including excessive daytime sleepiness, impaired vigilance, problems with memory and decision making, and mood changes.1 Over the last three decades, there has been increasing attention on how neurocognitive deficits manifest in pediatric patients with obstructive sleep apnea and milder forms of sleep-disordered breathing (SDB) such as snoring. The case of a young boy who presented with snoring despite adenotonsillectomy highlights some of the behavior and learning challenges seen in children with obstructive sleep apnea and the improvements that can be seen with treatment.
PATIENT CASE
A 5-year, 10-month-old boy with a history of eczema and allergic rhinitis presented to our Pediatric Sleep Clinic for snoring despite adenotonsillectomy.
He had reportedly “always snored.” Initially, he was managed on fluticasone nasal spray and montelukast without improvement in his snoring. At the age of 5, he underwent an adenotonsillectomy. His family reported that he continued to snore afterwards. His mother would prop him up on two pillows to sleep at night, hoping to decrease episodes of witnessed apneas and gasping for air. She noted that after apneic events, he would briefly awaken, look around, reposition himself, and fall back to sleep. In the mornings, his mother had to pick him up out of bed and stand him up in order to wake him.
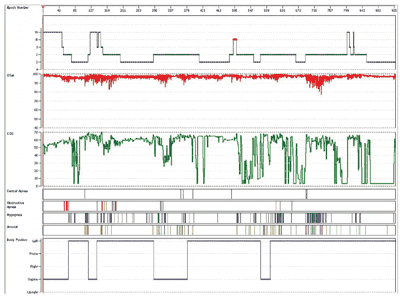
Figure 1. Hypnogram and trend plots of Spo2, ETco2, central apneas, obstructive apneas, hypopneas, arousals, and body position for the patient’s diagnostic polysomnogram.
At school, he was not doing well. His kindergarten teacher reported that he would fall asleep in class. When he was awake, he did not appear to be listening or paying attention and could “not sit still.” He had difficulty with reading and comprehension. On a 6 point grading scale with 6 being the best grade and 1 being the worst, he earned 2s and 3s, translating to “average” or “below average” scores. After school, he would nap from 4 to 5:30 pm and still be able to fall asleep between 8 and 8:30 pm. He woke up for school at 6:30 am. On weekends, he slept from 10:30 pm to 8:30 am and would still doze off throughout the day. His brothers described him as “sluggish” and “grouchy.” His mother felt that during periods of alertness, he was “hyper” and “impulsive.”
His physical exam was notable for intermittent mouth breathing, hypertrophied inferior nasal turbinates with clear rhinorrhea, decreased airflow through each naris, and a Friedman tongue position score of 3. Both his body mass index and blood pressure were normal for his age.
Polysomnography showed that he had severe obstructive sleep apnea with an apnea/hypopnea index of 29 per hour of sleep, SpO2 <90% for 0.7% of the study time, SpO2 nadir of 76.7%, ETco2 values of >50 mm Hg for 58.3% of the study time, and an increased arousal index of 16.1 per hour of sleep.
He soon returned for a CPAP titration. He was titrated from 5 to 9 cm of H2O pressure. No obstructive apneas or central apneas were observed on the titration. CPAP at 7 cm of H2O pressure eliminated snoring, hypopneas, and maintained SpO2 values in the mid-90s and above. In this sleep lab, ETco2 values on the majority of patients (both with and without sleep-disordered breathing) run high despite appropriate methods of trouble-shooting. Even so, the ETco2 values on the CPAP titration showed improvement compared to the PSG study (ETco2 values measured >50 mm Hg for 10% of the study time).
A week after starting CPAP therapy, his family reported that he was no longer sleeping during the day. His slightly older brother insisted, “He is much better. More awake. He can play with us now.” At 1 month follow-up, his mother stated that not only was he alert during the day, his teacher had also commended him for improvement in his behavior. He was no longer “sluggish.” He was paying attention and his reading comprehension improved. By the end of the school year, he was beginning to spell and his grades had improved to 5s and 6s.
DISCUSSION
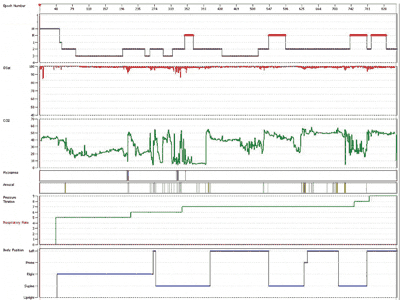
Figure 2. Hypnogram and trend plots of Spo2, ETco2, hypopneas, arousals, pressure titration, and body position for the patient’s CPAP titration study. There were no apneas on the CPAP titration study.
Obstructive sleep apnea is characterized by intermittent partial to full upper airway obstruction, resulting in episodic hypoxemia, hypoventilation, and sleep fragmentation. Although definitions of OSA by PSG testing differed in studies of children ranging in age from 2 to 18 years, most prevalence reports range from 1% to 4%.2 Obstructive sleep apnea has a bimodal peak. The first peak occurs in prepubescent children aged 2-8 years and mirrors the timing of rapid tonsillar and adenoid tissue growth relative to the size of the oropharynx. The second peak occurs in teens with the onset of obesity. With the United States’ current childhood obesity epidemic, the prevalence of pediatric OSA may be climbing. This is of particular concern due to comorbidities associated with OSA such as neurocognitive impairments.
Although more severe OSA has been associated with worse memory and learning measurements,3 the adverse neurocognitive consequences of obstructive sleep apnea are not limited to those with severe OSA. Across the range of sleep-disordered breathing, from snoring to mild OSA and moderate/severe OSA, children with SDB are reported to have signs of neurocognitive impairment.4-6 Similarly, neurocognitive problems are not limited to OSA in a specific age group. They have been described in preschool, grade school, and teenaged children with OSA.4,7,8
Whether it is from parent/teacher report, validated questionnaires, or formal batteries of tests, studies have shown that children with OSA have neurocognitive problems with increased daytime sleepiness,9 mood, behavior, and executive function. Negative effects on mood include anxiety, depression, and emotional lability.4,6 Adverse effects on behavior include problems with behavior regulation, aggression, oppositional behavior, internalizing (ie, behaviors [such as being withdrawn] that manifest from a child keeping emotions inside) and externalizing problems (ie, behaviors [such as lashing out] that manifest from a child directing their emotional response outwards), social problems, and hyperactivity.4,6,8-12 Deficits in executive function include problems with attention, learning, memory, verbal and motor fluency, planning, and academic achievement.3-5,7-9,11 Interestingly, when children who ranked in the bottom 10th% of their class13 and children described as inattentive/hyperactive14 were screened, they were found to be more likely to have signs and symptoms of OSA. Inattention and hyperactivity are becoming such well-known daytime symptoms of OSA that in the 2011 clinical practice guideline for the diagnosis, evaluation, and treatment of attention-deficit/hyperactivity disorder (ADHD), the American Academy of Pediatrics recommended that screening for sleep apnea should be done in the evaluation of a child for ADHD.15
In the last decade, research has begun to shed light on what causes these neurocognitive deficits in children with OSA, and why these impairments are seen variably in children with OSA. Signs of systemic inflammation, intermittent hypoxia, and endothelial dysfunction have been found to be more common in children with OSA and neurocognitive impairment compared to those without.16-18 It has been theorized that systemic inflammation caused by OSA can result in neuronal injury.16 Intermittent hypoxia in rats has been shown to result in increased cell death in the cortex and hippocampus, key areas of the brain involved in cognitive function and memory.19 It is possible that inflammation, intermittent hypoxia, and endothelial dysfunction all play interconnected roles in causing neurocognitive deficits. For example, inflammation can result in endothelial dysfunction. The endothelial dysfunction could result in regional neuronal apoptosis by causing regional impairments in cerebral vascular blood flow and subsequent hypoxia.
Theories aside, the most important question is, if we diagnose it, can we fix it? Fortunately, the answer appears to be “yes.” Multiple studies have documented improvement in behavior symptoms after children with OSA were treated by adenotonsillectomy.7,9,10,20,21 This improvement is not limited to those with severe OSA. Even in children with “mild” OSA (defined in the study as an apnea/hypopnea index of 1-5 events/hour), neurocognitive improvements have been observed after treatment of OSA.21
Whether the neurocognitive deficit can be completely reversed is yet to be answered. In rat pups that were subjected to intermittent hypoxia, Gozal et al found that hypoxia introduced at certain developmental stages resulted in more neuronal apoptosis than in others.19 Brain maturation has certain “critical periods” during which insult to the brain can be more damaging to neurobehavioral, psychological, and intellectual outcomes.22 However, whether a young brain is more vulnerable to insult or better able to overcome insult due to plasticity is still hotly debated.23
Although the patient highlighted in the case above did not have formal neurocognitive testing, he exhibited obvious signs of neurocognitive dysfunction including excessive daytime sleepiness, inattention, hyperactivity, restlessness, impulsiveness, grouchiness and poor academic performance. With treatment of the OSA, he appeared to have rapidly improved in noticeable ways to both his family and teacher. Additionally, he developed the necessary academic skills to advance to his next grade level with confidence. These neurocognitive improvements after treatment of his OSA demonstrate for us the important impact that managing a child’s obstructive sleep apnea can have on day-to-day family and school function.
Roberta M. Leu, MD, is director of pediatric sleep medicine and assistant professor of pediatrics at Emory University, Division of Pulmonary, Allergy/Immunology, Cystic Fibrosis, and Sleep. Emmanuel J. Porquez, BS, RPSGT/RST, is an experienced polysomnographer with a passion for educating students and sleep technologists in the field of pediatrics. Over the past 10 years, he has lectured in pediatric courses, physician board reviews, technician’s board reviews, technician’s A-Step programs, and pediatric scoring classes as well as authored various webinar lectures. Porquez is an employee of Children’s Healthcare of Atlanta. Questions for the authors can be submitted to [email protected].
REFERENCES
- Jackson ML, Howard ME, Barnes M. Cognition and daytime functioning in sleep-related breathing disorders. Prog Brain Res. 2011;190:53-68.
- Lumeng JC, Chervin RD. Epidemiology of pediatric obstructive sleep apnea. Proc Am Thorac Soc. 2008;5(2):242-252.
- Rhodes SK, Shimoda KC, Waid LR, et al. Neurocognitive deficits in morbidly obese children with obstructive sleep apnea. J Pediatr. 1995;127(5):741-744.
- Beebe DW, Ris MD, Kramer ME, Long E, Amin R. The association between sleep disordered breathing, academic grades, and cognitive and behavioral functioning among overweight subjects during middle to late childhood. Sleep. 2010;33(11):1447-1456.
- Bourke R, Anderson V, Yang JS, et al. Cognitive and academic functions are impaired in children with all severities of sleep-disordered breathing. Sleep Med. 2011;12(5):489-496.
- Rosen CL, Storfer-Isser A, Taylor HG, Kirchner HL, Emancipator JL, Redline S. Increased behavioral morbidity in school-aged children with sleep-disordered breathing. Pediatrics. 2004;114(6):1640-1648.
- Landau YE, Bar-Yishay O, Greenberg-Dotan S, Goldbart AD, Tarasiuk A, Tal A. Impaired behavioral and neurocognitive function in preschool children with obstructive sleep apnea. Pediatr Pulmonol. 2012;47(2):180-188.
- Beebe DW, Wells CT, Jeffries J, Chini B, Kalra M, Amin R. Neuropsychological effects of pediatric obstructive sleep apnea. J Int Neuropsychol Soc. 2004;10(7):962-975.
- Stradling JR, Thomas G, Warley AR, Williams P, Freeland A. Effect of adenotonsillectomy on nocturnal hypoxaemia, sleep disturbance, and symptoms in snoring children. Lancet. 1990;335(8684):249-253.
- Ali NJ, Pitson D, Stradling JR. Sleep disordered breathing: effects of adenotonsillectomy on behaviour and psychological functioning. Eur J Pediatr. 1996;155(1):56-62.
- Mulvaney SA, Goodwin JL, Morgan WJ, Rosen GR, Quan SF, Kaemingk KL. Behavior problems associated with sleep disordered breathing in school-aged children—the Tucson Children’s Assessment of Sleep Apnea study. J Pediatr Psychol. 2006;31(3):322-330.
- Bourke RS, Anderson V, Yang JS, et al. Neurobehavioral function is impaired in children with all severities of sleep disordered breathing. Sleep Med.2011;12(3):222-229.
- Gozal D. Sleep-disordered breathing and school performance in children. Pediatrics. 1998;102(3 Pt 1):616-620.
- Chervin RD, Archbold KH, Dillon JE, et al. Inattention, hyperactivity, and symptoms of sleep-disordered breathing. Pediatrics. 2002;109(3):449-456.
- Wolraich M, Brown L, Brown RT, et al. ADHD: clinical practice guideline for the diagnosis, evaluation, and treatment of attention-deficit/hyperactivity disorder in children and adolescents. Pediatrics. 2011;128(5):1007-1022.
- Gozal D, Crabtree VM, Sans Capdevila O, Witcher LA, Kheirandish-Gozal L. C-reactive protein, obstructive sleep apnea, and cognitive dysfunction in school-aged children. Am J Respir Crit Care Med. 2007;176(2):188-193.
- Gozal D, Kheirandish-Gozal L, Bhattacharjee R, Spruyt K. Neurocognitive and endothelial dysfunction in children with obstructive sleep apnea. Pediatrics. 2010;126(5):e1161-1167.
- Row BW, Kheirandish L, Neville JJ, Gozal D. Impaired spatial learning and hyperactivity in developing rats exposed to intermittent hypoxia. Pediatr Res. 2002;52(3):449-453.
- Gozal E, Row BW, Schurr A, Gozal D. Developmental differences in cortical and hippocampal vulnerability to intermittent hypoxia in the rat. Neurosci Lett. 2001;305(3):197-201.
- Mitchell RB, Boss EF. Pediatric obstructive sleep apnea in obese and normal-weight children: impact of adenotonsillectomy on quality-of-life and behavior. Dev Neuropsychol. 2009;34(5):650-661.
- Mitchell RB, Kelly J. Behavioral changes in children with mild sleep-disordered breathing or obstructive sleep apnea after adenotonsillectomy. Laryngoscope. 2007;117(9):1685-1688.
- Anderson V, Spencer-Smith M, Wood A. Do children really recover better? Neurobehavioural plasticity after early brain insult. Brain. 2011;134(Pt 8):2197-2221.
- Anderson V, Spencer-Smith M, Leventer R, et al. Childhood brain insult: can age at insult help us predict outcome? Brain. 2009;132(Pt 1):45-56.






