The use of CPAP for the entire sleep period is likely to be critical to the normalization of MSLT scores
It has been estimated that approximately 2% to 4% of adults are affected by obstructive sleep apnea (OSA).1,2 Most patients are prompted to seek medical consultation because of loud snoring, stopped-breathing episodes during sleeping, and/or excessive daytime somnolence (EDS). For example, in a recent study3 of consecutive patients evaluated for OSA, it was found that 25% of patients had chief complaints of loud snoring, 42% complained of stopped-breathing episodes, and 31% had complaints of EDS.
The degree to which patients’ complaints are reversed by a therapeutic intervention may predict patient satisfaction and treatment compliance. In this context, treatment of OSA with continuous positive airway pressure (CPAP) has been somewhat controversial. Many studies have documented that patients use CPAP for only part of the night. Engleman et al4 found no improvement on multiple sleep-latency test (MSLT) scores among patients with mild to moderate OSA. Similar results were reported for a study5 in which the maintenance-of-wakefulness test was used. In contrast, an earlier study6 documented a partial improvement in MSLT scores among patients with moderate OSA. More recently, a study7 comparing therapeutic and subtherapeutic CPAP quantified changes on a modified maintenance-of-wakefulness test and demonstrated a positive impact of CPAP at therapeutic settings. These reports are consistent with the findings of Kribbs et al,8 who documented that MSLT scores improved from 3.1 minutes at baseline to 5.5 minutes at follow-up among a sample of patients with moderate OSA. In this study, the follow-up period was an average of 75.8 days (range=30 to 237) of CPAP treatment. These results, while of significance, highlight the potential limitations of CPAP therapy. The use of CPAP for the entire sleep period is likely to be critical to the normalization of MSLT scores. For example, studies in normal subjects have demonstrated that shortening time in bed (and, thus, total sleep time) results in systematic increments in their level of sleepiness, when determined by the MSLT. Specifically, a study9 in which subjects were allowed to spend 8 hours, 4 hours, 2 hours, or no time in bed yielded a systematic shortening of their sleep latencies on the MSLT on the following day that correlated with the amount of time that they had spent in bed. In this context, patients who use CPAP for only part of the night are left untreated for the portion of the night spent without CPAP. Thus, a recurrence of sleep fragmentation and oxygen desaturations is experienced by these patients. The partial recurrence of OSA limits the benefits that may otherwise be derived from CPAP.
The aim of this study was to evaluate the response to CPAP therapy as manifested by modified MSLT scores under one of two CPAP use conditions. Random assignment of OSA patients was made to either a group using CPAP for less than 6.5 hours per night or a group using CPAP for more than 7.5 hours per night. Both groups were evaluated during the first week of CPAP treatment.
Subjects
Eligible subjects were clinic patients who were diagnosed with OSA based on 8-hour clinical polysomnography (CPSG). Of the patients diagnosed with OSA, who had a respiratory event index (REI) >10, only those who elected CPAP therapy were eligible for entry into this study. For entry into the study, subjects were required to have a regular nocturnal sleep schedule and were to be without any current psychiatric diagnosis. Subjects were required to be free of any illicit drugs and free of any medications that act on the central nervous system. Subjects continued to use all other prescribed medications. Subjects received a CPAP education session given by a trained technician. During this session, mask fitting and an actual trial of CPAP (with the patient seated in a comfortable recliner) were completed to ascertain patient’s acceptance of this form of therapy. Participation in the study was discussed with prospective participants following the CPAP education session. Informed consent was obtained from all participating subjects.
Procedures
Subjects were instructed to refrain from caffeine and/or alcohol consumption for at least 5 hours prior to arrival at the laboratory. Before subjects arrived at the laboratory for their CPAP titration at 9 pm, their group assignments (less than 6.5 hours or more than 7.5 hours) were randomly determined. Subjects completed an overnight 8-hour CPSG for CPAP titration purposes. CPAP was initiated at a setting of 5 cm H2O and the pressure was increased by 1 cm H2O at intervals of 10 to 15 minutes until respiration and sleep continuity were normalized. The therapeutic pressure setting was determined on the morning following titration by a board-certified sleep medicine physician.
After arising, subjects remained in the laboratory for a modified MSLT. Nap opportunities were given at 9:30 am, 9:55 am, 10:20 am, 10:45 am, and 11:05 am. The naps were concluded after three consecutive epochs of stage-1 non–rapid–eye-movement (NREM) sleep, the first epoch of any other stage of sleep, or 20 minutes of wakefulness.
Following the modified MSLT, subjects were given a CPAP machine set at their prescribed pressure settings and equipped with a microprocessor that recorded compliance. Subjects were informed of their group assignment and were encouraged to use their CPAP machines every night while at home for nights two through seven.
On the eighth night of the study, subjects returned to the laboratory for an additional CPSG and modified MSLT. Subjects assigned to the <6.5-hours group were recorded for 6 hours (1 am to 7 am), while subjects assigned to the >7.5-hours group were recorded for 8 hours (11 pm to 7 am). The morning after the follow-up CPSG, the CPAP machines were downloaded to obtain compliance data for the nights spent at home. The night recordings and modified MSLTs were scored in 30-second epochs according to the criteria of Rechtschaffen and Kales.10
Results
The two groups had significant evidence of sleep-related breathing disorders at the time of diagnosis. The group assigned to <6.5 hours of use per night had an apnea index (AI) of 29 and a hypopnea index (HI) of 20, while the group assigned to >7.5 hours of use per night had an AI of 32 and a HI of 20. Their prescribed CPAP pressures were also comparable (11.5±2.2 and 11.1±2.5 cm H2O, respectively), and resulted in an improvement of sleep-disordered breathing (REI <10). During the six nights at home, the <6.5-hours group averaged 5.4±1.5 hours of CPAP therapy per night, while the >7.5-hours group averaged 8.1±0.6 hours of CPAP therapy per night (P<.01).
In both groups, the CPAP use at home per night was comparable to the amount of CPAP therapy received on the follow-up CPSG. On the second visit to the laboratory, a week later, the two groups differed in sleep efficiency as a result of their scheduled time in bed. The <6.5-hours group spent significantly less time in bed on the return CPSG and had a sleep efficiency of 92%, while the >7.5-hours group achieved a sleep efficiency of only 86%.
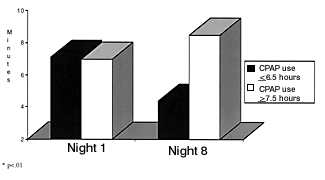
The modified MSLT scores were analyzed; they showed that, while both groups were comparable at baseline (<6.5-hours group=7.1±4.4 minutes and >7.5-hours group=7±3.2 minutes), they differed at the follow-up visit. The >7.5-hours group had a significantly higher modified MSLT score (8.5±5.2 minutes), compared with the <6.5-hours group (4.4±4.4 minutes, P<.05; see figure).
The initial and follow-up modified multiple sleep-latency test
scores of subjects with obstructive sleep apnea (P<.01);
CPAP=continuous positive airway pressure.
Discussion
The modified MSLT has been previously used among clinic populations with complaints of EDS.11 The modified MSLT procedure has also been used in evaluating the effects of naps of different durations on the subsequent propensity to fall asleep among patients with narcolepsy and healthy sleep-deprived or alert subjects. The results of this study12 showed that the modified MSLT effectively differentiated various levels of sleepiness. Based on these experiences, the modified MSLT was considered a viable alternative for the objective evaluation of sleep propensity among OSA patients, in particular, because the modified MSLT would further facilitate subject participation.
In the present study, the adherence to the two different CPAP schedules resulted in a differential pattern of polysomnographically determined sleep propensity. Clinical practice and research reports on CPAP compliance, however, have systematically shown that actual CPAP use by patients is less than ideal. These studies6,13 usually report CPAP compliance at less than 5.5 hours per night. During the first week of CPAP therapy, Rosenthal et al14 evaluated CPAP compliance in a population of severe-OSA patients (REI=67±44). Compliance was found to be only 4.2 hours per night. A more recent study,15 which evaluated CPAP compliance among a population of mild OSA patients (REI=18±6), found the rate of compliance to be 4.1 hours per night during the first week of treatment. The same rate of CPAP compliance was found when these patients were evaluated a year after the initiation of treatment. These studies were important in helping to determine the amount of time that subjects were asked to use CPAP every night. The <6.5-hours group was intended to parallel the compliance rates documented by other researchers. While it is not possible to know, based on the design of this study, whether patients stayed in bed for longer periods of time, we were able to monitor their actual CPAP use.
An additional issue of interest is the rate of change on MSLT scores as a result of the initiation of CPAP therapy. A study by Lamphere et al16 investigated the resolution of sleepiness in three groups of OSA patients who received CPAP therapy and were evaluated using the MSLT at different time intervals. Patients who received CPAP therapy for 2 weeks were found to have higher MSLT scores than patients who had received CPAP therapy for only a night (6 minutes). Both of these scores were significantly higher than baseline values (3.4 and 3 minutes, respectively). These results demonstrate that the recovery of alertness requires more than a night of normalized breathing during sleep. Further improvement was noted in the group that was evaluated after 6 weeks, but this did not reach significance when compared with the group evaluated at the 2-week follow-up. These results illustrate that, while the normalization of breathing is immediate, the change in MSLT scores is delayed by at least several days.
A previous study17 evaluating adherence to CPAP therapy and its effects on MSLT scores demonstrated that the enforcement of CPAP use can accelerate the improvement of MSLT scores. In that study, patients were randomly assigned to one of two groups following CPAP titration: one had an enforced CPAP-compliance schedule and the other had an unenforced CPAP-compliance schedule. Subjects in the enforced-compliance group were asked to sleep in the laboratory for 5 days and were monitored while using CPAP for 8 hours each night. Subjects in the unenforced-compliance group were provided with CPAP machines set at their prescribed pressures and were told to follow their regular sleep schedules at home for 5 days. They were told to use their CPAP machines for their entire sleep periods, but were not instructed to make any changes in their habitual sleep schedules. While their CPAP compliance was differential (8 hours per night versus 6.6 hours per night for the laboratory and home groups, respectively), the study was flawed because of the inherent bias introduced by having the laboratory group monitored significantly more closely. Nevertheless, on the sixth night after titration, both groups returned to the laboratory. Upon their return to the laboratory, both groups slept for 8 hours and had MSLTs the following day. The results showed that the change in MSLT scores after 6 nights on CPAP was comparable to the one documented for the present study.
A limiting factor in the treatment of OSA patients with CPAP is the lack of consistent data revealing predictors of compliance. Some research reports18 have suggested that snoring, severity of sleepiness, and the REI may be predictors of CPAP compliance, but no overall consensus is available. An additional limiting factor might be related to the CPAP instrumentation itself. Such a possibility has not been fully evaluated. It is possible that, for some individuals, nasal symptomatology and the effects of using the interface for several hours result in sleep disruption that limits their ability to meet the ideal level of compliance.
Leon Rosenthal, MD, is a staff physician at Sleep Medicine Associates of Texas, Dallas.
Acknowledgment
The data presented in this report were collected at the Henry Ford Sleep Disorders Center, Detroit. The collaboration of Peter Guido, MD, Ryan Day, Mary Lou Syron, Joe Fortier, and Keith Nykamp made this work possible.
References
1. Young T, Palta M, Dempsey J, et al. The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med. 1993;328:1230-1235.
2. Jennum P, Sjol A. Epidemiology of snoring and obstructive sleep apnoea in a Danish population, age 30-60. J Sleep Res. 1992;1:240-244.
3. Day R, Gerhardstein R, Lumley A, et al. The behavioral morbidity of obstructive sleep apnea. Prog Cardiovasc Dis. 1999;41:341-354.
4. Engleman H, Martin S, Deary I, et al. Effect of CPAP therapy on daytime function in patients with mild sleep apnoea/hypopnoea syndrome. Thorax. 1997;52:114-119.
5. Engleman H, Kingshott R, Wraith P, et al. Randomized placebo-controlled crossover trial of continuous positive airway pressure for mild sleep apnea/hypopnea syndrome. Am J Respir Crit Care Med. 1999;159:461-467.
6. Engelman H, Martin S, Deary I, et al. Effect of continuous positive airway pressure treatment on daytime function in sleep aponea/hypopnoea syndrome. Lancet. 1994;343:572-575.
7. Jenkinson C, Davies R, Mullins R, et al. Comparison of therapeutic and subtherapeutic nasal continuous positive airway pressure for obstructive sleep apnoea: a randomized prospective parallel trial. Lancet. 1999;353:2100-2105.
8. Kribbs N, Pack A, Kline L, et al. Effects of one night without nasal CPAP treatment on sleep and sleepiness in patients with obstructive sleep apnea. Am Rev Respir Dis. 1993;147:1162-1168.
9. Rosenthal L, Roehrs TA, Rosen A, et al. Level of sleepiness and total sleep time following various time in bed conditions. Sleep. 1993;16:226-232.
10. Rechtschaffen A, Kales A. A Manual of Standardized Terminology, Techniques and Scoring System for Sleep Stages of Human Subjects. Washington, DC: US GPO; 1968.
11. Stepanski E, Zorick F, Wittig R, et al. Modified MSLT procedure [abstract]. Sleep. 1994;23:164.
12. Helmus T, Rosenthal L, Bishop C, et al. The alerting effects of short and long naps in narcoleptic, sleep deprived, and alert individuals. Sleep. 1997;20:251-257.
13. Kribbs NB, Pack AI, Kline LR, et al. Objective measurement of patterns of nasal CPAP use by patients with obstructive sleep apnea. Am Rev Respir Dis. 1993;147:887-895.
14. Rosenthal L, Nykamp K, Guido P, et al. Compliance with CPAP during the first week of treatment [abstract]. Sleep Research. 1997;26:489.
15. Rosenthal L, Gerhardstein R, Lumley A, et al. CPAP therapy in patients with mild OSA: implementation and treatment outcome. Sleep Medicine. 2000;1:215-220.
16. Lamphere J, Roehrs T, Wittig R, et al. Recovery of alertness after CPAP in apnea. Chest. 1989;96:1364-1367.
17. Rosenthal L, Helmus T, Syron M, et al. The effect of a structured environment on the recovery of alertness in OSA patients treated with CPAP [abstract]. Sleep Research. 1996;25:349.
18. McArdle N, Devereux G, Heidarnejad H, et al. Long-term use of CPAP therapy for sleep apnea/hypopnea syndrome. Am J Respir Crit Care Med. 1999;159:1108-1114.