Treating OSA via surgical manipulation of the airway should be considered in the overall planning for young patients since apnea is a chronic disease process and its effects can be life-threatening.
Maxillofacial advancement surgery to treat obstructive sleep apnea (OSA) has been well documented.1-17 These surgical techniques have been useful to treat patients with proven skeletal discrepancies that can create apneas. Such discrepancies comprise mandibular deficiency, maxillary deficiency, genial deficiency, or any combination of the above. Patients benefiting from advancement surgery have one of these discrepancies, or they would not benefit from stable jaw relationships after advancement. By widening and/or advancing these skeletal components, the soft tissue envelope that surrounds the airway changes shape and becomes less likely to collapse.
Two types of surgical advancement techniques used to treat OSA are titratable techniques such as distraction osteogenesis and nontitratable techniques such as corrective jaw surgery. Both types enlarge the airway in three dimensions by manipulating the skeleton that supports the surrounding soft tissue drape. As the skeleton is advanced, the tissue drape enlarges the space of the airway and tightens the flaccid tissues, making them less likely to collapse.
Nontitratable Techniques
Nontitratable surgical techniques, such as first maxillary and/or mandibular osteotomies, allow the bones to be advanced and stabilized at the time of surgery. These are the most commonly used corrective jaw surgery techniques. In these procedures, the upper and/or lower jawbone is cut so that the bone can be advanced or widened. Next, bone plates are secured to the bone to stabilize the osteotomy; 6 to 8 weeks later, the bone has healed enough to be fully functional. Bone movements are limited by the ability of soft tissues to stretch. The movements are very precise and can predictably achieve a functional occlusion and an aesthetic result (Figure 1); however, if the advancement is too large (past the elastic limit of the soft tissues), then there is a good chance that the bone movement will relapse. If relapse occurs, the patient will wind up with a malocclusion or further functional problems, which necessitates additional surgery.
 Figure 1a. Pretreatment lateral cephalogram. Note mandibular retrognathia, genial deficiency, and maxillary deficiency. |
 Figure 1b. Preoperative orthodontic setup is to maximize the skeletal movements without compromise of the aesthetic. |
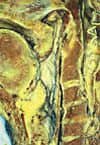 Figure 1c. Final result showing a large increase in posterior airway space after moving the maxilla, mandible, and chin with standard corrective jaw surgery. The mandible was advanced 11 mm. |
Although the occlusal and aesthetic results are predictable,2 it is very difficult to predict whether the movement will cure the sleep apnea. Even the most severe apnea patients can be treated if they have a skeletal deficiency. The surgical movement is limited by the aesthetic envelope.17 More important, once sleep apnea patients have been treated with this technique and their bones are stable, a positive result must be confirmed with a new sleep study. If the result is not curative, then more surgery may be needed, or patient care may still need to be supplemented with CPAP treatment or a mandibular appliance. Although corrective jaw surgery is an effective cure for this disease, it may not be as predictable in some cases.1
Distraction Osteogenesis
Distraction osteogenesis is another technique that advances both the maxilla and mandible. This surgical technique was first used to lengthen limbs and was applied to treat the craniofacial skeleton in children with severe skeletal deformities that were not amenable to standard corrective jaw surgery.2,10,11 Many of these tracheostomy-dependent children could be decannulated once their craniofacial skeletons were aligned with distraction because their skeleton obstructed their airway.
Distraction osteogenesis allows for the slow expansion of the bone and associated soft tissues. The expansion is not completed until the apnea ceases. Distraction osteogenesis has been a great technique in the management of pediatric airway compromise and micrognathia. It is slowly becoming a surgical adjunct in lieu of tracheostomy and even lip-tongue adhesion surgery in the infant.2
Specifically, distraction osteogenesis creates osteotomies as in standard corrective jaw surgery; however, instead of placing solid bone plates across the osteotomy gaps, expansion devices known as distractors are placed. These devices can be slowly separated and will create tension across the osteotomy gap. The tension encourages the bone to grow across the gap. It also creates a slow tissue expansion around the jaws. It stretches the muscles, nerves, and blood vessels, and because the expansion devices can be incrementally advanced, the cure for the apnea can be titrated.
The disadvantage of distraction surgery is that it takes significantly longer to accomplish than standard surgical techniques. Once the bone is cut, the bone must heal for up to 7 days so that a clot forms. Only after the clot has formed may there be any bone movement. The average bone movement is 1 mm per day during this distraction period. Once the apnea is gone, bone movement is ceased, and the bone is permitted to continue to heal in what is known as a consolidation phase. In this phase, the bone will calcify enough so that the distractors can be removed during a second surgical procedure. The average consolidation phase lasts at least twice as long as the distraction period.
Distraction is extremely technique-sensitive. The distractors must be placed along the correct movement vector. Precise movement of the bones is difficult and may not accurately establish a good functional occlusion. Newer distractor designs permit movement-vector adjustment, but generally are more cumbersome.
The nature of the skeletal discrepancy that has created the airway obstruction must be considered when choosing which advancement technique to use. If the surgical movement of the skeleton is greater than a centimeter, distraction osteogenesis maintains a more stable surgical result. The literature on surgical manipulation to treat sleep apnea indicates that most patients need more than one centimeter advancement. Therefore, distraction osteogenesis may be a better choice in most cases.1-17
Distraction osteogenesis may also be considered for younger patients and patients with scar tissue. Chil-dren tolerate distraction osteogenesis better than adult patients; however, children must tolerate the adjustment of the distractor. Distractor adjustment is similar to the use of palatal expanders to widen the palate for orthodontic treatment. Care must be taken to avoid the developing dentition when placing these distractors in children. Scar tissue in patients with previous surgical treatment (cleft palate, trauma, or cancer) will not expand easily. Distraction will help expand such inelastic tissue (Figure 2).
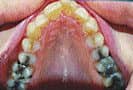 Figure 2a. Child with radiation-induced micrognathia and sleep apnea. Tonsils and adenoids had already been removed. |
 Figure 2b. Endpoint of titration of the mandible once sleep apnea was cured. Note large change in airway space posteriorly. Distraction vectors are parallel to the occlusal plane. The occlusion was intentionally left as class III and functional so that the skeletal bases would be aligned. The radiation had also compromised her dentition and she will eventually lose these teeth, which will need to be replaced. The aesthetics are im-proved, not compromised. |
Sometimes a patient may need a combination of both titratable and nontitratable techniques. In such a combination procedure, first the distraction will be performed to advance the bones and soft tissue while achieving the necessary stability. Formal jaw surgery will follow to establish a functional occlusion.
Conclusion
As we follow these surgically treated patients over the long term, we find that their sleep apnea remain cured. This result is achieved only for apneas treated with surgical advancement due to skeletal causes of obstruction. Since apnea is a chronic disease process and its effects can be life-threatening, surgical manipulation of the airway should be considered in the overall treatment planning of young patients. Although surgical treatment may initially be perceived as “aggressive” in the management of this disease, it may be psychosocially less conservative when contrasted with alternatives such as a lifetime of nightly wearing a nasal mask or a dental appliance. Furthermore, patients who do not comply with the prescribed use of these appliances may suffer severe, long-term dental effects and other possible detrimental effects.
Stephanie J. Drew, DMD, is an oral maxillofacial surgeon at The New York Center for Orthognathic and Maxillofacial Surgery, West Islip, NY; [email protected].
References
1. Goh YH, Lim KA. Modified maxillomandibular advancement for the treatment of obstructive sleep apnea: a preliminary report. Laryngoscope. 2003;113:1577-1582.
2. Rhee ST, Buchman SR. Pediatric mandibular distraction osteogenesis. J Craniofac Surg. 2003;14:803-808.
3. Woodson BT, Hanson PR, Melugin MB, Gama AA. Sequential upper airway changes during mandibular distraction for obstructive sleep apnea. Otolaryngol Head Neck Surg. 2003;128:142-144.
4. Sher AE. Upper airway surgery for obstructive sleep apnea. Sleep Med Rev. 2002;6:195-212.
5. Bettega G, Pepin JL, Orliaguet O, Levy P, Raphael B. Surgery and obstructive sleep apnea syndrome: indications and precautions. Rev Stomatol Chir Maxillofac. 2002;103:181-187.
6. Prinsell JR. Maxillomandibular advancement surgery for obstructive sleep apnea syndrome. J Am Dent Assoc. 2002;133:1489-1497.
7. Gilon Y, Raskin S, Heymans O, Poirrier R. Surgical management of maxillomandibular advancement in sleep apnea patients. Int J Adult Orthodon Orthognath Surg. 2001;16:305-314.
8. Fibbi A, Ameli F, Brocchetti F. Combined genioglossus advancement (ACMG): inferior sagittal mandibular osteotomy with genioglossus advancement and stabilization with suture in patients with OSAS. Acta Otorhinolaryngol Ital. 2002;22:153-157.
9. Li KK, Guilleminault C, Riley RW, Powell NB. Obstructive sleep apnea and maxillomandibular advancement: an assessment of airway changes using radiographic and nasopharyngoscopic examinations. J Oral Maxillofac Surg. 2002;60:526-530.
10. Monasterio FO, Drucker M, Molina F, Ysunza A. Distraction osteogenesis in Pierre Robin sequence and related respiratory problems in children. J Craniofac Surg. 2002;13:79-83.
11. Li KK, Powell NB, Riley RW, Guilleminault C. Distraction osteogenesis in adult obstructive sleep apnea surgery. J Oral Maxillofac Surg. 2002;60:6-10.
12. Gregg JM, Zedalis D, Howard CW, Boyle RP, Prussin AJ. Surgical alternatives for treatment of obstructive sleep apnoea. Ann R Australas Coll Dent Surg. 2000;15:181-184.
13. Mehra P, Downie M, Pita MC, Wolford LM. Pharyngeal airway space changes after counterclockwise rotation of the maxillomandibular complex. Am J Orthod Dentofacial Orthop. 2001;120:154-159.
14. Hendler BH, Costello BJ, Silverstein K, Yen D, Goldberg A. A protocol for uvulopalatopharyngoplasty, mortised genioplasty, and maxillomandibular advancement in patients with obstructive sleep apnea: an analysis of 40 cases. J Oral Maxillofac Surg. 2001;59:892-897.
15. Maurer JT, Hirth K, Mattinger C, Hormann K. Combined surgical and prosthetic therapy of severe obstructive sleep apnea—a case report. Laryngorhinootologie. 2001;80:278-281.
16. Li KK, Troell RJ, Riley RW, et al. Uvulo-palatopharyngoplasty, maxillomandibular advancement, and the velopharynx. Laryngoscope. 2001;111:1075-1078.
17. Li KK, Riley RW, Powell NB, Guilleminault C. Patient’s perception of the facial appearance after maxillomandibular advancement for obstructive sleep apnea syndrome. J Oral Maxillofac Surg. 2001;59:377-380.