 |
The updated American Academy of Sleep Medicine (AASM) practice parameters for actigraphy signal the increasing acceptance of this modality as a diagnostic tool. Adding to the recognition of actigraphy is a recent surge in research documenting the usefulness of the application in not only sleep medicine but other applications as well. Maximizing the usefulness of actigraphy requires an understanding of its functionality, applications, and recently revised practice parameters.
There is little question about the increasing prevalence of actigraphy in the sleep disorders marketplace today. With the rise in awareness of the various sleep disorders in both the general and medical communities, actigraphy has risen to the forefront as a viable diagnostic methodology. However, actigraphy isn’t just for sleep anymore.
In past years, actigraphy has been used to assess circadian cycle-related disorders, such as advanced and delayed sleep phase syndromes, shift work sleep disorder, jet lag, and blindness-associated non-24-hour sleep-wake syndrome. Now, the popularity of this recording modality has quickly spread. A recent Google™ search of the term “actigraphy” rendered hits describing the application’s use from the diagnostics for hepatic encephalopathy, to a monitor for activity tolerance in COPD patients enrolled in pulmonary rehabilitation, to an adjunct interoperative monitoring device for anesthesia, to the measure of physical activity in wheelchair users.
|
Want information about actigraphy manufacturers? ReadSleep Review’s online buyer’s guide.
|
ACTIGRAPHY 101
At its core, the actigraph is a device that combines a recording device with an accelerometer. An actigraph is generally worn on a limb and records its movements. Actigraphy use in sleep disorders medicine is primarily for the documentation of a patient’s sleep-wake through the correlation of periods of activity and inactivity. Simply put, as the body goes through the circadian cycle, activity increases with the level of awakening, and then decreases during sleep. The actigraph records a “tic” for each movement, and the frequency of occurrence and amplitude of exertion are correlated with the sleep-wake cycle.
ACCELEROMETRY
Several types of accelerometers are produced. These range from capacitive, piezoelectric, piezoresistive, and magnetoresistive, to heat transfer. 1 Their applications are broadly distributed in our everyday environment. For example, the automotive industry uses accelerometers as impact detection components for airbag systems. A more novel and recent application is Nintendo™ Corp’s game-controlling wand, named Wii. These handheld units combine the user’s arm and/or hand accelerating and decelerating motion to augment the finger controllers as an additional parameter of control. 2 The typical accelerometer used in actigraphy is piezoelectric.
Actigraphy: Applications and Illustrations |
|
 |
|
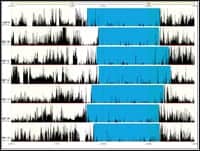
| With actigraphy, activity is represented by a tic-mark on the graph. These tics denote not only the frequency of activity occurrence, but the level of exertion (as represented in the amplitude). With an increase in occurrence and exertion, the reviewer can approximate these levels with sleep and wake. This can be seen in the illustration of a normal patient. | |
 |
|
| The illustration shows a reading from a patient with insomnia. This graphic reveals an inability to maintain a regular schedule. Moreover, the inability to maintain sleep has led this patient to getting sleep at times that otherwise would be considered undesirable—or even inappropriate. | |
 |
|
| Shift workers often encounter sleep-wake issues as a result of cyclic dysfunction. The illustration of the shift-work patient’s pattern of sleep drastically changes with sleep occurring nocturnally on day 3, followed by 3 consecutive days of diurnal sleep. Moreover, the patient “makes up” sleep on day 8. Finally, when the patient is asleep, there is evidence of fragmentation, as demonstrated by areas of considerable activity. | |
For accelerometers, acceleration is defined as “the time rate of change of velocity with respect to magnitude or direction; the derivative of velocity with respect to time.” 3 When graphically plotted, acceleration is the slope of velocity versus time. The accelerometer captures either the changes in acceleration and deceleration in terms of g-force—or the gravitational equivalent of 32 feet per second at sea level. To provide a reference, earth’s gravity = 1g; a sneeze produces an approximate 3g force; and human unconsciousness occurs at a range of 7g to 10g.
RECORDING: ACTIGRAPHY VERSUS POLYSOMNOGRAPHY
Polysomnography has been and remains the gold standard of obtaining a diagnostic picture of a patient’s sleep-wake pathology. 4 By virtue of the multiple-channel recording capabilities, the polysomnograph retains the greatest degree of physiologic review. Unfortunately, though, it is impractical for long-duration use for a variety of reasons, not the least of which involves file sizes, recorder sizes, and sensor-attachment issues. By contrast, the more compact actigraph measures the activity of the limb on which it is worn in a single channel. 5 While lacking the robust multichannel capabilities, actigraphy makes up for this deficit in its long-term recording and ambulatory features.
Depending on the settings, most actigraphy units can record up to 21 days, which is more suitable for the investigation of insomnia, sleep phase shifts, and shift work analysis. Moreover, models introduced to the marketplace in recent years have been enhanced to target specific areas of interest with the correlation to sleep-wake cycles. Specifically, newer actigraphs can record additional channels, such as light lumen levels, core body temperature, and caloric expenditure.
Many of the current systems are produced in a form that resembles a watch and can be comfortably worn for long periods of time. As additional recording capabilities have been included in newer releases, so have the units’ improved aesthetics. At the recent Association of Professional Sleep Societies’ meeting in Minneapolis, one manufacturer’s president was seen wearing a new model that more closely resembled a fashionable Nike-style sports watch, rather than the chunky little black-box style of just a few years past.
PRACTICE PARAMETER UPDATE
In January of this year, the AASM published an updated version of its original 2003 Practice Parameters for the use of actigraphy. In putting this document together, members of the AASM performed an extensive literature search that looked at research involving actigraphy in the assessment and management of sleep disorders. This review then provided the background for evidence-based recommendations for the use of actigraphy in the clinical environment.
In addition to the previously recognized applications for circadian cycle-related sleep-wake disorders, the new document recommended:
- that actigraphy be performed as an adjunct measure in multiple sleep latency tests for the documentation of a stable sleep pattern and adequate sleep times prior to the test.
- when polysomnography is unavailable, actigraphy can be used as a means to estimate the total sleep time in patients with obstructive sleep apnea syndrome. When combined with a validated method of monitoring respiratory events, actigraphy may improve accuracy in assessing OSA severity by identifying the time in bed.
- the use of actigraphy for the measure of sleep and circadian rhythm patterns for treatment outcomes documentation in older nursing home residents or older adults in the community for whom polysomnography is not a viable option.
- actigraphy application in the infant, pediatric, and special needs populations where polysomnography is not a viable option.
The importance of this document is clear—the AASM has recognized the proliferation of actigraphy’s usage in the research environment. It also has answered the community’s request for evidence-based recommendations and guidelines. These efforts will lead to the eventual acceptance by commercial carriers of the value of this testing modality, allowing them to see actigraphy usage is no longer an experimental process. 6
“Because there is substantial evidence to indicate actigraphy is indicated for evaluation and management of specific common sleep disorders, we are hopeful that clinicians and insurers will become more aware of its usefulness and more familiar with its application,” says Timothy Morgenthaler, MD, of the Mayo Clinic in Rochester, Minn, and a member of the American Academy of Sleep Medicine’s Standards of Practice Committee. “We believe that applying these recommendations will result in a higher quality of patient care in certain circumstances.”
Allen Boone, RPSGT, is the associate clinical director of sleep services for SleepMed Inc, Columbia, SC. He is also a member of Sleep Review‘s editorial advisory board. The author extends a special note of appreciation to Mark Reed and Jodi Bump, RN, of Mini Mitter®, a Respironics Company®, for their assistance with this article. Boone can be reached at .
REFERENCES
- Texas Instruments. Accelerometers and how they work. www2.usfirst.org/2005comp/manuals/acceler1.pdf.
- wii.nintendo.com.
- Acceleration. Dictionary.com. Dictionary.com Unabridged (v 1.1). Random House Inc. dictionary.reference.com/browse/acceleration. Accessed May 24, 2007.
- Ancoli-Israel S. Actigraphy. In: Kryger M, Roth T, Dement W, eds. Principles and Practice of Sleep Medicine. 4th ed. Philadelphia: Elsevier Saunders; 2005:1459-1465.
- Morgenthaler T, Alessi C, Friedman L., et al. Practice parameters for the use of actigraphy in the assessment of sleep and sleep disorders: an update for 2007. Sleep. 2007;30:519-529.
- Aetna Clinical Policy Bulletin: actigraphy testing, www.aetna.com/cpb/medical/data/700_799/0710.html. Accessed May 24, 2007.






