 |
Pediatric obstructive sleep apnea syndrome (POSAS) is a serious condition that causes snoring and interrupted sleep patterns and is associated with even graver sequelae such as behavioral, attentional, cardiovascular, and cognitive problems. Enlargement of the tonsils and adenoids is a common cause of POSAS. Tonsillectomy and adenoidectomy is generally the surgical procedure of choice for managing POSAS. It not only can resolve snoring and promote restful, healthy sleep for pediatric patients, but also may enhance their quality of life, result in improved behavior and grades, and relieve the problem of bedwetting. Although the basic procedure for tonsillectomy has not changed substantially through the decades, newer techniques such as Coblation provide a safer and more efficient approach that offers children an improved quality of life.
BACKGROUND
Obstructive sleep apnea syndrome is a chronic condition in which the upper airway is periodically obstructed during sleep, causing oxygen desaturation, frequent awakening, and excessive daytime sleepiness. In children, the syndrome can precipitate a cascade of associated disorders, including hyperactivity, attention-deficit disorder, impaired cognition, cardiovascular and metabolic conditions, and failure to thrive.
|
Want more case reports? Search Sleep Review’s online archives .
|
POSAS affects an estimated 1% to 3% of children,1,2 with equal occurrence among boys and girls3 but a higher prevalence among African American children4 and those who were born preterm.5,6 Although continuous positive airway pressure is generally considered the gold standard treatment for adults, it is not well tolerated by children. Tonsillectomy and adenoidectomy has been found to be remedial in most pediatric patients and is one of the most common surgeries performed under general anesthesia in children: as many as 600,000 children undergo tonsillectomy and adenoidectomy in the United States every year.
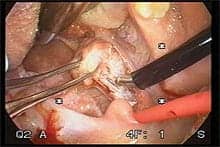 |
| Figure 1. Coblation tonsillectomy uses low-temperature bipolar radio frequency for more positive patient outcomes than standard electrocautery tonsillectomy. |
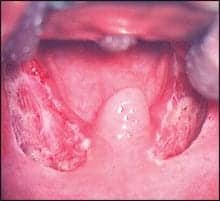 |
| Figure 2. Tonsillar fossae following Coblation tonsillectomy show faster healing with less damage to adjacent tissue than is typically seen with other surgical techniques. |
Despite the prevalence of pediatric adenotonsillectomy procedures, parents may resist the surgery because it is painful for the child, involves a lengthy recovery, and may cause postoperative complications. However, when the surgery is performed with Coblation®, a low-temperature bipolar radio-frequency ablation technique that is less invasive than standard electrocautery tonsillectomy (Figure 1), children tend to experience less pain and a quicker return to normal diet and activities,7,8 fewer postoperative complications,9,10 reduced damage to adjacent tissue,11 and faster healing (Figure 2).12
The Coblator II Surgery System uses a controlled bipolar radio frequency-based plasma process. Coblation has been shown to gently break down soft tissue at relatively low temperatures (40º C to 70º C) with little or no bleeding, postoperative nausea, or throat swelling.10,11 It differs from other electrocautery and radio-frequency techniques in that a glow discharge via a conductive medium such as saline, rather than heat or radio frequency, is the mediator of the treatment.
The technology on which Coblation is based is currently used not only for tonsillectomy,13 but in other procedures that require fine tissue excision, such as disc decompression in the spine,14 turbinate reduction in otolaryngic surgeries,15 and tendon and cartilage debridement in sports medicine.16
SIGNS AND SYMPTOMS
POSAS produces both daytime and nighttime symptoms. During sleep, symptoms include snoring, gasping, restlessness, sleepwalking, frequent awakening, and bedwetting.
Daytime signs that a child is experiencing POSAS include noisy or mouth breathing, unusual sleepiness, irritability, rhinorrhea, headache, enlarged tonsils and adenoids, behavioral disturbances, academic problems, and failure to thrive.
In addition, POSAS may involve cardiovascular symptoms. Children with POSAS often have high blood pressure,17 elevated levels of C-reactive protein, which is associated with cardiovascular disease,18 and left ventricular hypertrophy.19 These symptoms suggest a connection between POSAS and cardiovascular disorders.
PATIENT CASE
An otherwise healthy 9-year-old boy was referred by his primary care physician based on a 2- to 3-year history of snoring, mouth breathing, interrupted sleep patterns, and gasping for air during sleep. The child had experienced at least four episodes of tonsillitis per year for the previous 3 years, and enlarged adenoids were also suspected. His parents reported that he had occasional bedwetting accidents and his school behavior and grades were deteriorating. The primary physician had expressed concern about the possibility of attention-deficit disorder and learning disabilities.
PHYSICAL EXAMINATION
The physical exam noted open mouth breathing with +4 tonsils extending to the midline; other head and neck findings were normal. Polysomnography revealed a respiratory disturbance index (RDI) of 17 and lowest oxygen saturation of 86%.
DISCUSSION
The patient underwent tonsillectomy and adenoidectomy with Coblation. No intraoperative or postoperative complications were reported, and he was discharged home the same day. The patient was seen for a follow-up visit 1 week postoperatively. At that time, his parents reported that he had required Tylenol with Codeine for 4 days and had resumed a normal diet within 72 hours. At the 6-month postoperative visit, his parents reported that the boy was sleeping quietly, his grades and behavior had improved significantly, and the bedwetting episodes had ceased.
CONCLUSION
Compared with traditional electrocautery surgical methods, Coblation adenotonsillectomy results in faster healing, minimal destruction of surrounding tissue, less postoperative pain, and better resolution of both clinical and behavioral symptoms.7-12 Studies have found no statistical differences between the rebleed rates for Coblation adenotonsillectomy and those of other techniques20,21 and a lower incidence of primary and secondary hemorrhage.22 Additionally, Coblation has been found efficacious in treating pediatric tonsillar hypertrophy, with a better quality of postoperative recovery than other methods.8,13,23 Coblation adenotonsillectomy offers surgeons the ease of use and versatility of a single device to perform tonsillectomy and adenoidectomy with an extremely low rate of serious complications.13,23,24
Ramzi Tamer Younis, MD, is professor and chief of pediatric otolaryngology at the Leonard M. Miller School of Medicine, Bascom Palmer Eye Institute, Miami. He has published several scientific articles in peer-reviewed ENT journals. He is editor of the textbook Pediatric Sinusitis and Sinus Surgery (Taylor and Francis Publishing Group, New York, 2006). He recently edited a special issue on pediatric tonsillectomy for ORL, December 2007. Younis can be reached at .
REFERENCES
- Ali NJ, Pitson DJ, Stradling JR. Snoring, sleep disturbance, and behaviour in 4–5 year olds. Arch Dis Child. 1993;68:360-366.
- Chervin RD, Archbold KH, Dillon JE. Inattention, hyperactivity, and symptoms of sleep-disordered breathing. Pediatrics. 2002;109:449-456.
- Daly JA III. Pediatric obstructive sleep apnea syndrome: not a chip off the ol’ block! [removed]www.dcmsonline.org/jax-medicine/2001journals/March2001/pediatric.html[/removed].
- Redline S, Tishler PV, Schluchter M, et al. Risk factors for sleep-disordered breathing in children. Associations with obesity, race, and respiratory problems. Am J Respir Crit Care Med. 1999;159:1527-1532.
- Rosen CL, Larkin EK, Kirchner HL, et al. Prevalence and risk factors for sleep disordered breathing in 8- to 11-year-old children: association with race and prematurity. J Pediatr. 2003;142:383-389.
- Emancipator JL, Storfer-Isser I, Taylor G, et al. Variation of cognition and achievement with sleep-disordered breathing in full-term and preterm children. Arch Pediatr Adolesc Med. 2006;160:203-210.
- Temple RH, Timms MS. Paediatric Coblation tonsillectomy. Int J Pediatr Otorhinolaryngol. 2001;61:195-198.
- Timms MS, Temple RH. Coblation tonsillectomy: a double blind randomized controlled study. J Laryngol Otol. 2002;116:450-452.
- Stoker KE, Don DM, Kang DR, et al. Pediatric total tonsillectomy using Coblation electrosurgery compared to conventional electrosurgery: a prospective, controlled single-blind study. Otolaryngol Head Neck Surg. 2004;130:666-675.
- Glade RS, Pearson SE, Zalzal GH, Choi SS. Coblation adenotonsillectomy: an improvement over electrocautery technique? Otolaryngol Head Neck Surg. 2006;134:852-855.
- Ghosh S, Roper A, Timms MS. Adenoidectomy with the Coblator: a logical extension of radiofrequency tonsillectomy. J Laryngol Otol. 2005;119:398-399.
- Chinpairoj S, Feldman M, Saunders JC, et al. A comparison of monopolar electrosurgery to a new multipolar electrosurgical system in a rat model. Laryngoscope. 2001;111:213-217.
- Chan KH, Friedman NR, Allen GC, et al. Randomized, controlled, multisite study of intracapsular tonsillectomy using low-temperature plasma excision. Arch Otolaryngol Head Neck Surg. 2004;130:1303-1307.
- Gerszten PC, Welch WC, King JT Jr. Quality of life assessment in patients undergoing nucleoplasty-based percutaneous discectomy. J Neurosurg Spine. 2006;4:36-42.
- Back LJ, Hytonen ML, Malmberg HO, et al. Submucosal bipolar radiofrequency thermal ablation of inferior turbinates: a long-term follow-up with subjective and objective assessment. Laryngoscope. 2002;112:1806-1812.
- Uribe JW. The use of radiofrequency devices for chondral debridement. Sports Med Arthrosc Rev. 2003;11:214-221.
- Marcus CL, Greene MG, Carroll JL. Blood pressure in children with obstructive sleep apnea. Am J Respir Crit Care Med. 1998;157:1098-1103.
- Larkin EK, Rosen CL, Kirchner HL, et al. Variation of C-reactive protein levels in adolescents: association with sleep-disordered breathing and sleep duration. Circulation. 2005;111:1978-1984.
- Amin R. Cardiovascular consequences of sleep apnea in children. Presented at: American Thoracic Society Conference; May 2001; San Francisco.
- Divi V, Benninger M. Postoperative tonsillectomy bleed: Coblation versus non-Coblation. Laryngoscope. 2004;115:31-33.
- Clark MP, Smithard A, Jervis P. How we do it: Coblation tonsillectomy complication rates from a single ENT department compared with the National Prospective Tonsillectomy Audit. Clin Otolaryngol. 2006;31:156-159.
- Belloso A, Chidambaram A, Morar P, Timms MS. Coblation tonsillectomy versus dissection tonsillectomy: postoperative hemorrhage. Laryngoscope. 2003;113:2010-2013.
- Patel J, Mandal S, Rachmanidou A. Paediatric Coblation tonsillectomy versus dissection tonsillectomy: a comparative study of post-operative pain and complications. Int J Pediatr Otorhinolaryngol. 2004;68:725.
- Friedman M, LoSavio P, Ibrahim H, Ramakrishnan V. Radiofrequency tonsil reduction: safety, morbidity, and efficacy. Laryngoscope. 2003;113:882-887.





