Sleep Number Corp presents data as posters from two new studies using its 360 smart bed at SLEEP 2021.
Data presented at the meeting show results of a predictive model of COVID-19 infection based on sleep metrics and results from a large study analyzing overnight heart rate variability (HRV), providing evidence for the benefits of the 360 smart bed and SleepIQ technology as potential devices for evaluating population health. The 360 smart bed and its operating system, SleepIQ technology, deliver individualized sleep health evaluations and outcomes by automatically sensing and responding to the needs of sleepers. The 360 smart bed adjusts throughout the night, digitally sensing each sleeper’s movements and automatically adjusting the firmness to keep both sleepers comfortable. SleepIQ technology is embedded in every 360 smart bed.
“The research findings from these two new studies, presented at SLEEP 2021, add to the growing body of scientific research from our Sleep Number 360 smart bed,” says Annie Bloomquist, chief innovation officer, Sleep Number, in a release. “The 360 smart bed is an innovative device that offers proven quality sleep, an accurate, longitudinal data collection platform and the ability to understand real-world sleep behaviors. These data and insights are informing the development of meaningful sleep solutions.”
Longitudinal, unobtrusive, and ecologically valid sleep metric estimation from a smart bed to predict the pathology of COVID-19 (Congress Abstract ID: 651)
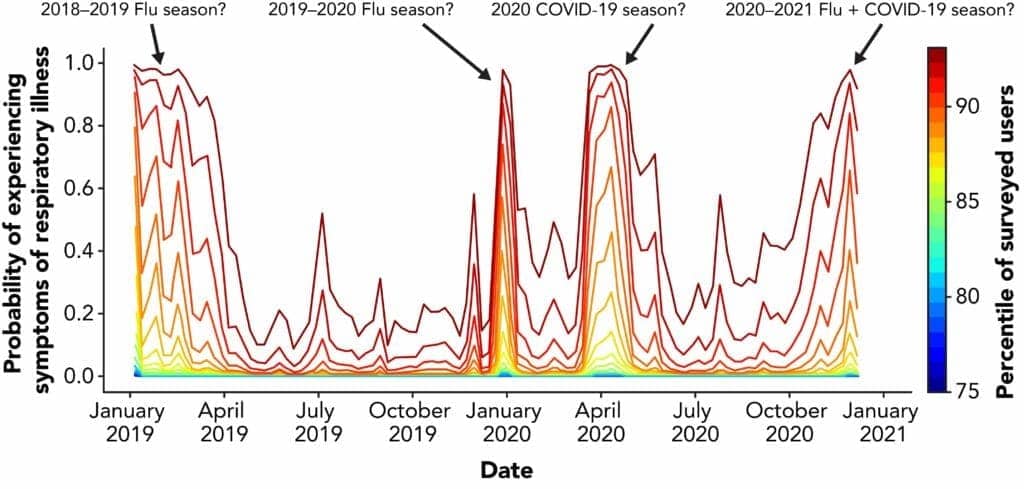
Viral respiratory illnesses such as COVID-19 may impact sleep duration, quality, and cardiorespiratory function. An analysis of real-world data collected from COVID-19 positive (n=122) and negative (n=1,603) 360 smart bed sleepers was conducted to build a predictive COVID-19 model based on unobtrusive sleep metrics. Sleep duration, sleep quality, restful sleep duration, time to fall asleep, respiration rate, heart rate, and motion level obtained from ballistocardiography data from January 2019 to October 2020 were measured in the analysis.
In the COVID-19 positive group, worsening of symptoms was associated with an increase in sleep duration, average breathing rate, average heart rate, and a decrease in sleep quality. For those in the COVID-19 negative group, no significant disruptions in sleep and cardiorespiratory metrics were observed. The evaluation of the predictive model resulted in cross-validated area under the receiving-operator curve (AUC) estimate of 0.84±0.09, similar to values reported in wearable sensors. The closer an AUC value comes to 1.0, the more accurate the model becomes. When the data set was expanded beyond the initial self-reported dates of symptom onset in the COVID-19 positive group, the AUC estimate improved to 0.93±0.05.
Sleep Number is working on expanding these capabilities to detect symptoms for illnesses such as the common cold, influenza, and SARS.
Overnight heart rate variability depends on age, gender, and day of the week: a field observation using the 360 smart bed platform (Congress Abstract ID: 249)
HRV, the variation in time between heartbeats, is commonly used to assess the activity of the autonomic nervous system (ANS), which unconsciously regulates certain essential bodily functions including breathing, heart rate, blood pressure, and others. Changes to autonomic nervous system function, reflected in HRV, can result from factors including lifestyle, aging, cardiorespiratory illnesses, sleep state, and physiological stress. HRV is lower under situations of stress, either emotional or physical, and is higher in relaxed states. While there is broad interest in researching HRV, few studies to date have established normative overnight HRV values for a large population.
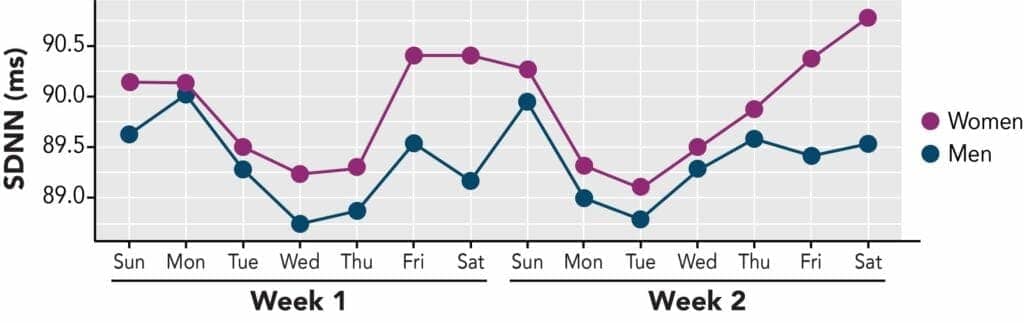
An analysis of overnight standard deviations in normal-to-normal (SDNN) heartbeat intervals from 18.2 million sleep sessions from 379,225 Sleep Number 360 smart bed sleepers was conducted to better understand population-level HRV changes. Higher SDNN numbers generally correlate with better health and cardiac response to stress, and lower SDNN numbers are an indicator of unhealthy cardiac activity. Results of the analysis found significant cross-sectional associations between overnight SDNN and age, gender and day of the week. For sleepers under 50 years old, SDNN declined at a rate of about 2.1 milliseconds/year, then leveled off for sleepers aged 50-65, and increased slightly thereafter. Women under 50 showed lower, more slowly declining SDNN values than men, but this trend reversed for sleepers over 50. Additionally, SDNN values were generally highest over the weekend and lowest at mid-week. SDNN values for women followed a U-shaped pattern, starting high in the beginning of the week, dipping mid-week, then increasing through the weekend, whereas values for men followed an L-shaped pattern, starting high in the beginning of the week, but quickly fell and stayed low through the week.
These results show measuring overnight SDNN data using the 360 smart bed may be a useful, ecologically valid device for evaluating population health models reliant on heart rate variability.






