The aftermath of the CMS decision to approve portable monitoring hasn’t even come close to the initial hype that came with the announcement. Shifts away from in-lab polysomnography have been scarce, but researchers are starting to chip away at the scientific uncertainty that has resulted in the sluggish adoption of home testing. If new findings are met with changes in reimbursement, the enthusiasm for portable monitoring could be reignited.
On the research front, Samuel T. Kuna, MD, chief of the pulmonary, critical care and sleep section at the Philadelphia VA Medical Center, found that those who performed sleep testing in their homes with portable monitors showed similar improvements in daytime function after 3 months of treatment with continuous positive airway pressure (CPAP) as compared to patients who underwent overnight testing in a sleep center. Furthermore, patient adherence to CPAP over the first 3 months of treatment was similar in patients with OSA who received home versus in-lab testing.
“These findings represent a possible turning point for both patients with sleep-disordered breathing and the clinicians who treat them,” said Kuna. “One of the biggest and most insurmountable barriers to treatment is the need for overnight testing in a sleep laboratory. Our research suggests that this may no longer be mandatory for diagnosis.”
|
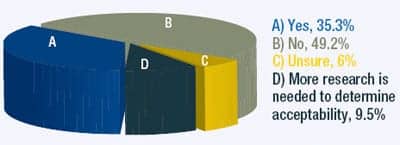
| WEB POLL: Are home tests an acceptable alternative to in-lab polysomnography? |
Scientifically, this study could serve as a turning point for portable monitoring, but in terms of reimbursement, cost-effectiveness, and standardization of home testing devices, more needs to be done. “We have a problem with lack of standardization of portable monitors,” says Kuna. “We still don’t know what signals are the best to record and that may differ from one patient population to another.” He also adds, “There is no reimbursement code for home autoCPAP titration. If there is going to be a true ambulatory management pathway, there needs to be a reimbursement fee to allow people to do it.”
Kuna is doing his part on the cost front; medical care costs were examined in the study, but they are still being analyzed. He hypothesized about the results, stating, “We believe that they will show that home portable monitor testing is less expensive than in-laboratory testing.”
Such a result, combined with the equivalent results of portable monitor testing in terms of health-related outcomes, would tackle some of the key barriers to implementation of home testing. While much hinges on reimbursement, the push for home testing is regaining some of its momentum.
—Franklin A. Holman
[email protected]



