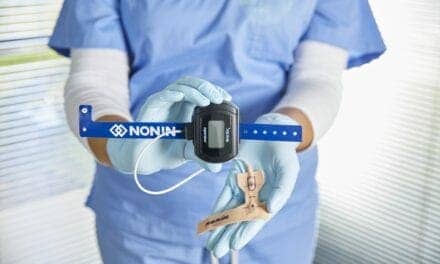
Wireless technology is now being recognized as an opportunity to expand the reach of a sleep laboratory, thereby enhancing clinical services. This may involve using wireless acquisition devices to transmit data from a patient room to the technologist workstation or transferring data from remote testing sites to the sleep laboratory via a wireless connection. Historically, the challenge had been that the size of polysomnographic (PSG) data files made the signal more difficult to transmit than voice or even image files. Early attempts involved adding an off-the-shelf wireless card and receiver to a standard PSG system, which did little to address some of the underlying challenges of data interruptions. The devices were large and heavy, making them difficult to transport. Their exorbitant energy requirements meant either they had to be plugged into a wall or fitted with multiple large batteries in order to obtain sufficient power for a full PSG. Consequently, many early advocates were left doubting whether innovations being appreciated in other fields of medicine would ever make their way to the sleep world.
These days, systems are better designed with redundant storage options and more refined signal transmission mechanisms. With some appreciation of the limitations, such as how far the patient can travel from the monitoring station, wireless PSG recorders can be just as reliable as wired connections.
How Wireless Technology Works
Wireless systems work by transmitting data via electromagnetic waves within a defined frequency. Early wireless systems were prone to transmission errors due to outside radio-frequency interference. Recent advances in wireless communication technology have allowed for the development of small and portable data acquisition systems capable of transmitting physiological data over short ranges (50 to 100 feet). This newer technology can guarantee reliable data transmission through the use of special data-encoding techniques that allow both detection and correction of errors in transmission. Further advances include the use of a technique known as frequency hopping that improves data throughput by allowing a system to dodge interference.
Choosing wireless PSG acquisition systems for new sleep laboratories has also become easier as the technology has improved. Upgrading to wireless no longer requires having an installation team come to the facility for the initial setup. The systems are designed to work right out of the box, and, with wireless, sites no longer need to connect rooms with cables hidden under carpets or fed through ceiling tiles and holes drilled in walls. More important, portable studies become much more practical because they can be done wherever there is a bed and a nearby work area for the technologist or Internet connection for remote monitoring.
Patient-Care ADVANTAGES
From a clinical perspective, the most significant advantage to wireless systems is the opportunity to expand PSG services into much-needed areas of the hospital, including intensive care units, rehabilitation units, and surgical suites. Because modern wireless systems are more compact than wired systems, they can be brought into a patient room without the need to rearrange other equipment, as is necessary to make cart systems fit. The wireless receiver and laptop computer can be positioned in the room or at a nearby nurse’s station, wherever it is safest and most accessible to the staff that will assist with the study. The system can then be networked (via the hospital’s secure wired or wireless intranet) to the PSG laboratory. The sleep technologist can monitor the signal live and, depending on staff situations, can either communicate with the nurse or respiratory therapist on the floor for assistance with lead repair or CPAP changes, or return as necessary for technical intervention.1 Since nothing needs to be plugged into the wall or mated with other components, the risk of creating electrical loops between the PSG system and other life-critical equipment is eliminated.
Wireless can also be cost effective as it allows inpatient sleep studies to be done with less added expense to the hospital. LDS Hospital in Salt Lake City, which has a three-bed sleep laboratory, reports that it increased its revenue by approximately $800,000 in 1 year when it added inpatient testing to its protocol. Plus, it increased physician awareness of the prevalence and importance of recognizing and treating OSA. This increased revenue resulted from receiving reimbursement by private payors, increasing the patient-to-technologist ratio, and doing more sleep consults and CPAP follow-up visits on patients that might otherwise have been lost to follow-up after discharge. These added fees easily offset the fact that Medicare patients (approximately 50% Medicare in this case) were not reimbursed because of diagnosis-related group (DRG) capitation issues.
(Reimbursement according to DRGs is a case-rate payment system developed by Medicare for hospital compensation. With DRGs, Medicare pays hospitals at a fixed amount according to the compensation set for the patient’s DRG, regardless of the services actually rendered to the patient.)
Challenges and Benefits
Of course, inpatient floors are not an ideal place for PSG recording. Sleep quality is likely to be impacted by the loud environment, as well as the pain or anxiety that comes with hospital admissions. Nursing staff may still need to enter the room to tend to basic care needs such as vital sign monitoring and medication administration.2 But, even without a full night of sleep, an apnea/hypopnea index (AHI) can still be derived and a diagnosis made. Though large prospective studies have not yet been completed, more immediate treatment of OSA—which is a risk factor for several serious cardiovascular and other health ailments—may lead to shortened inpatient stays and could also lead to improved CPAP compliance because of the extended opportunity for patient education. Also, the patient may more clearly see an association between sleep disordered breathing (SDB) and his or her hospital admission.
Outcome studies, most of which are conducted over the course of weeks or even months, have shown that nasal CPAP improves quality of life and may also benefit several aspects of health, including hypertension,3 atrial fibrillation recurrence, and insulin sensitivity.4 More immediate effects can also be expected. For instance, one study showed that improvements in cardiovascular function, including a rise in left ventricular ejection fraction, a decrease in left ventricular end-systolic dimension, a decrease in systolic blood pressure, and a decrease in heart rate, all occur relatively rapidly with CPAP therapy.5
Limited channel screening studies for SDB may be unsatisfactory. In the most comprehensive study on inpatient PSG done at Intermountain Health in Salt Lake City, total sleep time (TST) values were quite low relative to total recording time (TRT) because of the previously mentioned challenges. The mean TST was 3.3 hours, compared with a TRT of 5.9 hours. Had the AHI been calculated based on TRT, as is the case with most screening devices, the AHI would have been 19.4 per hour as compared with the actual, fully scored calculation with all electrophysiological measurements of 35.4.1 Also, in order for CPAP to be reimbursed by insurance companies, a full PSG is often required. Since it is inadvisable to allow medically compromised patients to become hypoxemic for long, split nights should be considered when possible. Later follow-up in-laboratory PSG studies may be necessary in order to confirm that symptom severity was not altered acutely or to ensure proper CPAP titration.
Cardiac Patients
It has been established that patients with coronary artery disease have a high prevalence of SDB. Schafer et al found OSA (AHI > 10) in 30.5% of patients with coronary artery disease as proven by angiography compared with 19.7% in normal controls.6 Up to 50% of patients with heart failure will show signs of SDB, usually sleep apnea.7 In a large retrospective study of 450 patients with symptomatic chronic heart failure (CHF), 75% of men and 47% of women were found to have SDB (AHI > 10/h). Asymptomatic left ventricular dysfunction also is associated with a higher incidence of SDB.8 Therefore, PSG can and should become an important part of the diagnostic inpatient evaluation for most cardiac patients.
Sleep Apnea in the Surgical Patient
Some facilities have very well-coordinated presurgical evaluation programs where patients undergo in-laboratory PSG prior to surgery, but those centers remain in the minority. Adverse surgical outcomes are more frequent in patients with sleep apnea, as both anesthesia and surgery further exacerbate airway instability and affect sleep architecture.9 In a retrospective evaluation of patients undergoing joint replacement surgery, up to a third of those with OSAS developed respiratory or cardiac complications that included myocardial infarction and arrhythmias or required transfer to the intensive care unit or reintubation.10 The presence of sleep apnea may first become apparent intraoperatively due to problems with intubation or maintenance of the airway, or patients may be noted to snore or have obstructive events while being cared for postoperatively. Wireless technology means that sleep laboratories can offer surgeons and anesthesiologists an opportunity to preoperatively assess SDB severity and/or more promptly evaluate and treat patients once problems arise. Again, follow-up PSG studies may still be required to confirm that SDB is chronic versus an acute response to anesthesia.
Prevalence of SDB Following Stroke
Sleep related breathing disorders are both a risk factor and a complication following stroke. Studies have shown that following stroke, SDB occurs in 60% to 70% of patients,11,12 and outcomes are associated with the severity of the breathing disorder.13 Wessendorf et al showed that using CPAP in poststroke patients significantly reduced mean nocturnal arterial blood pressure, improved subjective well-being, and increased slow wave sleep.14 The same study also showed that compliance may be less than that seen in the general population because patients are unable to handle the mask or understand the importance of the therapy. Treatment response could also be complicated by more central apneas and more mouth leak as a result of facial palsy in this population. Those stroke patients that were able to comply reported improved well-being and seemed to respond more favorably to their rehabilitation plan.
Positive Impact in Sleep Medicine
Wireless PSG technology is sure to have a positive impact on patient care as many sleep clinicians realize that bringing the sleep laboratory to the patient can improve responsiveness and staff efficiency. It could also increase physician awareness of the prevalence and impact of SDB faster and more effectively than any targeted marketing campaign.
Prasanth Manthena, MD, is the medical director of the sleep laboratory at Los Angeles Medical Center. He is board certified by the American Board of Sleep Medicine and the American Board of Neurology and Psychiatry. In addition, he is a member of the American Academy of Sleep Medicine and the American Academy of Neurology.
References
1. Farney R, Walker J, Cloward T, et al. Polysomnography in hospitalized patients using a wireless wide area network. J Clin Sleep Med. 2005;2:28-34.
2. Casey K, Lefor M. Management of the hospitalized patient with sleep disordered breathing. Curr Opin Pulm Med. 2002;8: 511-515.
3. Becker H, Jerrentrup A, Ploch T, et al. Effect of nasal continuous positive airway pressure treatment on blood pressure in patients with obstructive sleep apnea. Circulation. 2003;107:68-73.
4. Harsch IA, Schahin SP, Radespiel-Troger M, et al. Continuous positive airway pressure treatment rapidly improves insulin sensitivity in patients with obstructive sleep apnea syndrome. Am J Respir Care. 2004;169:156-62.
5. Kaneko Y, Floras J, Usui K, et al. Cardiovascular effects of continuous positive airway pressure in patients with heart failure and obstructive sleep apnea. N Engl J Med. 2003;348:1233-41.
6. Schafer H, Koehler U, Ewig S, et al. Obstructive sleep apnea as a risk marker in coronary artery disease. Cardiology. 1999;92: 79-84.
7. Jahaveri S, Parker T, Liming J, et al. Sleep apnea in 81 ambulatory male patients with stable heart failure: types and their prevalences, consequences and presentations. Circulation. 1998;97: 2154-2159.
8. Sin D, Fitzgerald F, Parker J, et al. Risk factors for central and obstructive sleep apnea in 450 men and women with congestive heart failure. Am J Resp Crit Care Med. 1999;160:1101-1106.
9. Koop R, Michota F, Jaffer A, et al. Unrecognized sleep apnea in the surgical patient: implications for the perioperative setting. Chest. 2006;129:198-205.
10. Gupta R, Parvizi J, Hanssen A, et al. Postoperative complications in patients with obstructive sleep apnea syndrome undergoing hip or knee replacement: a case-control study. Mayo Clin Proc. 2001;76: 897905.
11. Dyken ME, Somers VK, Yamada T, et al. Investigating the relationship between stroke and obstructive sleep apnoea. Stroke. 1996;27: 401-7.
12. Bassetti C, Aldrich M. Sleep apnea in acute cerebrovascular diseases: final report on 128 patients. Sleep. 1999;22: 217-23.
13. Good D, Henkle J, Gelber D, et al. Sleep-disordered breathing and poor functional outcome after stroke. Stroke. 1996;27: 252-259.
14. Wessendorf T, Wang Y, Thilmann A, et al. Treatment of obstructive sleep apnea with nasal continuous positive airway pressure in stroke. Eur Resp J. 2001;18:623-629.