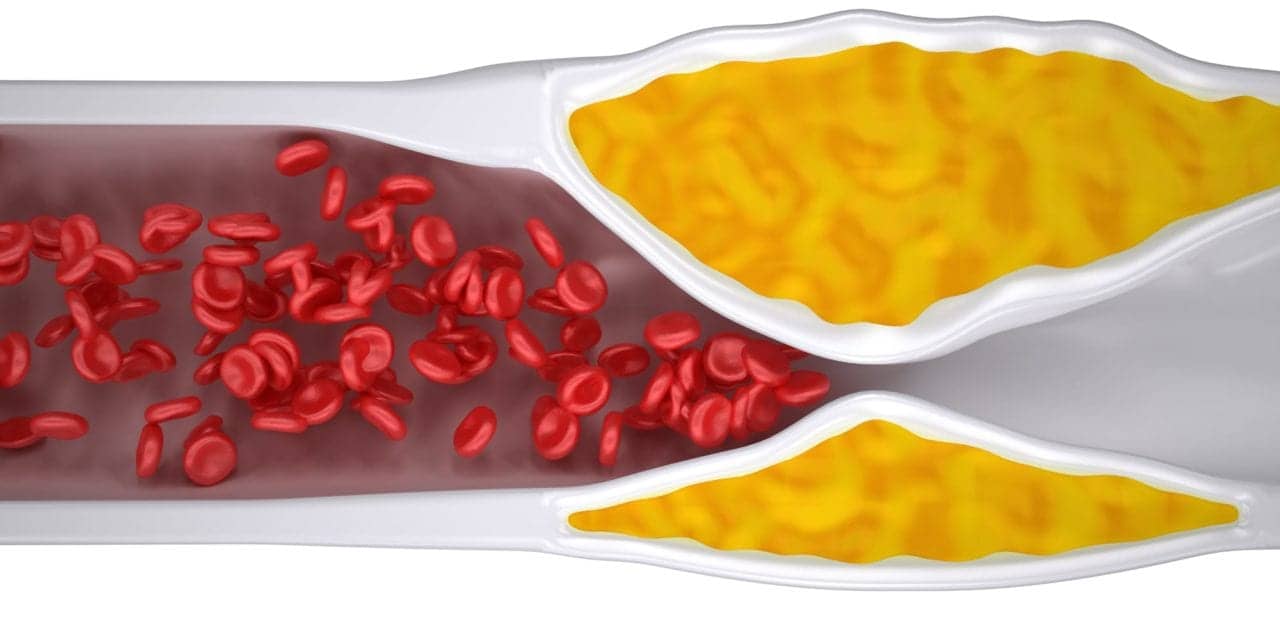
UC Berkeley sleep scientists have begun to reveal what it is about fragmented nightly sleep that leads to the fatty arterial plaque buildup known as atherosclerosis, which can result in fatal heart disease.
“We’ve discovered that fragmented sleep is associated with a unique pathway—chronic circulating inflammation throughout the blood stream—which, in turn, is linked to higher amounts of plaques in coronary arteries,” says study senior author Matthew Walker, PhD, a UC Berkeley professor of psychology and neuroscience, in a release.
The findings, published June 4 in the journal PLOS Biology, adds poor sleep as a key risk factor for cardiovascular disease, which ranks as the top killer of Americans.
“To the best of our knowledge, these data are the first to associate sleep fragmentation, inflammation, and atherosclerosis in humans,” says study lead author Raphael Vallat, PhD, a postdoctoral researcher in Walker’s Center for Human Sleep Science at UC Berkeley.
Established risk factors for cardiovascular disease in humans include poor diet, lack of exercise, obesity, high blood pressure, and smoking.
Using statistical modeling, the researchers analyzed the diagnostic data of more than 1,600 middle-aged and older adults using a national dataset known as the Multi-Ethnic Study of Atherosclerosis.
To isolate the effect of sleep quality on heart health, the study controlled for age, ethnicity, gender, body mass index, sleep disorders, blood pressure, and high-risk behaviors such as smoking.
The researchers then tracked the results of the study participants, analyzing their blood tests, their calcium scores that can gauge plaque buildup, as well as several different measures of sleep, including actigraphy-assessed sleep across a week and a night in a sleep laboratory that measured electrical brainwave signals.
The final outcome clearly linked disrupted sleep patterns to higher concentrations of circulating inflammatory factors and, specifically, of white blood cells known as monocytes and neutrophils, which are key players in atherosclerosis.
“In revealing this link with chronic inflammation, the findings suggest a missing middleman that is brokering the bad deal between fragmented sleep and the hardening of blood vessels,” Walker says.
The polysomnography (PSG)-measured link was not as robust as the actigraphy-measured link, though it remained significant after correcting for some but not all contributors, a difference the authors suggest may be due to the shorter duration of PSG (a single night) versus actigraphy (one week). No association was found for subjectively reported poor sleep, in which subjects were asked to recall the quality of their sleep, a finding which suggests that asking patients about the sleep may not be a useful tool for assessing their sleep-related risk of heart disease.
Vallat says, “Indeed, these associational results in humans mirror recent data in which experimentally manipulated sleep disruption in mice led to higher levels of circulating inflammation that caused atherosclerotic lesions in the rodents.”
The findings linking poor sleep to atherosclerosis via chronic inflammation have major public health implications, the researchers say.
For example, atherosclerosis often begins in early adulthood. “Unfortunately, this process goes largely unnoticed until the plaque buildup, in middle or old age, suddenly blocks arterial blood flow to the heart, lungs, brain and/or other organs, hence its moniker, ‘silent killer,'” Vallat says.
“The insidious nature of the disease requires that we pay attention to our sleep hygiene, even starting in early to midlife,” says study co-lead author Vyoma Shah, a doctoral student in Walker’s lab.
To more accurately gauge one’s sleep quality, the researchers recommend the use of clinical grade sleep trackers because the study found that people’s subjective assessments of their sleep were not reliable.
“If you track your sleep patterns using objective measures, the same way you track your weight, blood pressure, or cholesterol, you can make modifications to your sleep habits, which could make a tangible difference to later life health outcomes,” Shah says.
With chronic inflammation shaping up to be a bridge connecting poor sleep to cardiovascular disease, it’s worth exploring its role in a plethora of other diseases where inflammation is known to be a possible factor, the researchers said.
“This link between fragmented sleep and chronic inflammation may not be limited to heart disease, but could include mental health and neurological disorders, such as major depression and Alzheimer’s disease,” Walker says. “These are new avenues we must now explore.
“Improving sleep may offer a novel way to reduce inflammation and thus reduce the risk of atherosclerosis. These findings may help inform public health guidelines that seek to increase the continuity of sleep as a way to improve health and decrease the burden of heart disease on society.”