By Janice East, RPSGT, R. EEG T.,
The Board of Registered Polysomnographic Technologists (BRPT) has a long-standing commitment to ensuring that the RPSGT credentialing process and the credential itself remain relevant and responsive to the community of sleep technologists. In 2004 and again in 2007, we reached out to RPSGTs with an online survey asking our credential holders to tell us about their day-to-day working lives, their perception of the value of their credential, their feelings about the credentialing examination process, and their sense of how their profession was perceived within the broader allied health universe. Last year was also the 30th anniversary of the RPSGT credential, and as we celebrated that remarkable milestone, it seemed appropriate to connect with our credential holders to update our survey findings.
THE METHODOLOGY
The 2009 30th Anniversary Survey of RPSGTs was conducted online as a 53-question survey with a mixture of closed and open-ended questions. Invitations to participate were extended to RPSGTs only. The survey was made available in August 2009 to 8,074 RPSGTs with current e-mail addresses in their RPSGT profile at BRPT. The survey, which closed in early September 2009, generated 967 responses: a solid 12% response rate, statistically projectable against the universe of RPSGT credential holders.
OBJECTIVES
While we hoped to learn more about RPSGT attitudes toward the credential, the examination process, and technologists’ working lives and their perception of the place their profession holds among the allied health disciplines, we were particularly interested in comparing trends in responses to the results of the 2004 and 2007 survey of RPSGTs. How are attitudes toward the credential and the profession changing? How are RPSGTs feeling about the future of their profession? How do RPSGTs feel about the need for other credentials in the field?
A VALUED CREDENTIAL; A STRONGER PROFESSION
More than 90% of the RPSGTs completing the survey were very satisfied or satisfied with the credential, holding steady since 2007. Only 9% expressed dissatisfaction with the credential. Nearly 60% of respondents are currently working in AASM-accredited sleep facilities, a 6% increase from the 2007 survey; 8% are working in facilities holding an accreditation through another accrediting body. The percentage of respondents working in nonaccredited facilities dropped from 40% to 28%. And, while a majority of RPSGTs continue to work with sleep technologists who are not credentialed in sleep, the percentage has decreased since 2007 from 85% to 78%. More impressively, that figure has decreased from 94% of respondents in 2004 who reported working with technologists who were not credentialed.
The percentage of respondents who “strongly agreed” that “sufficient education/training/preparation options exist to prepare for the RPSGT exam” stood at 72%, up from 63% in 2007 and up a dramatic 31 percentage points from 2004. Nearly 80% of respondents reported membership in a professional organization: the American Association of Sleep Technologists (AAST) (45%), the American Academy of Sleep Medicine (AASM) (20%), or the American Association for Respiratory Care (AARC) (15%). About 41% of respondents hold another allied health credential. The survey found a 2% increase in the number of credential holders with an associate’s degree (34%) and a 4% increase in RPSGTs holding a bachelor’s degree (27%).
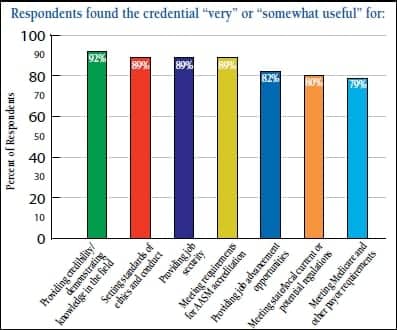
Despite a challenging economic environment, 50% of respondents felt that RPSGTs remain in great demand, due in large part to an overall shortage of credentialed sleep technologists, and nearly an equal percentage (49%) felt that, while the job market varies by region across the country, the market for credentialed technologists is good in their area. The survey also showed a strong awareness of—and pride in—the RPSGT credential (see chart).
Asked about the demand for an advanced credential in sleep technology, 50% of respondents to the 30th Anniversary Survey saw a demand for such a credential—a 6% drop from the 2007 survey. However, the percentage of respondents who felt there was no demand for an advanced credential also declined, from 24% to 22%. Respondents who saw the need for an advanced credential for technologists were most interested in a general advanced credential, an advanced scoring credential, and a sleep educator credential. Respondents expressed less interest in an advanced credential in geriatrics or a management credential.
THE COMMON THEMES
As the BRPT leadership reviewed the 30th Anniversary Survey, some very encouraging trends emerged. Some of the key findings from the 30th Anniversary Survey, particularly responses showing a growing commitment to education, training, and professionalism in our field, came into play as we worked with the AAST and AASM on the development of the Certified Polysomnographic Technician (CPSGT) certificate exam. The exam has been put in place to guide individuals new to the field on to the path toward earning the RPSGT credential. Certificate holders are bound by the RPSGT code of conduct, and are required to earn 10 continuing education credits each of the 3 years in which the CPSGT certificate may be held. The CPSGT exam reflects our discipline’s growing commitment to professionalism in the field of sleep technology.
THE COMMON CONCERNS
The 30th Anniversary Survey tool was developed to give RPSGTs an opportunity to both identify and rank perceived threats to the growth and continued development of the sleep technology field. For the first time, RPSGTs were asked questions about the perception of the sleep technology field as a distinct allied health discipline among legislators and other allied health professions: 64% of respondents felt that legislators and regulators do not view sleep technology as a distinct allied health discipline; 62% felt that the field was not seen as a distinct discipline among the other allied health disciplines.
Home and portable monitoring was perceived as a threat to the field by 42% of survey respondents, up from 16% in 2007. Non-health care management takeovers were seen as a threat by 42% of survey participants, a significant increase from 16% in 2007; hiring of noncertified technologists was seen as a threat to the profession by 35% of respondents, up from 28% in 2007 (noting that respondents in previous surveys chose only one significant threat, but could rank numerous threats on the most recent survey.)
The survey also showed us that technologists in our field are getting slightly older: only 12% of respondents to the most recent survey were under 30 years, compared to 20% in 2007. A quarter of respondents were between 30 and 39 years, down from a third in 2007. While 30% were between 40 and 49 years, the same percentage as in 2007, another third were over 50 years, compared with just 17% in 2007.
There was also a perceived need for consumer education materials addressing sleep disorders and the role of the sleep technologist. There was a demand for education materials geared toward physicians and addressing the critical importance of physician/technologist cooperation. There was also significant demand for an on-the-job training manual for supervisors training entry-level sleep technologists, highlighting the great majority of RPSGT candidates (more than 70%) who come to the RPSGT exam following Pathway #1 (18 months of paid clinical experience).
A STRATEGY FOR THE FUTURE
The threats identified by 30th Anniversary Survey respondents are real, but there is a positive note simply in the fact that the threats have been recognized and clearly articulated by so many RPSGTs. That underscores a growing awareness of our field as an evolving, distinct discipline, and a commitment to responding to perceived threats as a cohesive, united allied health care discipline, on par with the other disciplines within the allied health community. And it’s important to note that many of the threats identified by survey respondents are shared by the broader health care community, particularly the challenges of non-health care management takeovers and the “graying” of our workforce. Awareness of portable monitoring has grown dramatically since our 2007 survey, though as a force in our field it remains something of an unknown, and may ultimately represent new and different opportunities for sleep technologists.
We have a clear challenge as a discipline in continuing to define our particular place in the allied health care landscape—to consumers, to our allied health peers, and to state and federal legislative and regulatory bodies. The growing commitment to professionalism in our field, which we can clearly see among the survey respondents, is a critical part of that process.
We have a responsibility as a discipline to work toward the development of educational resources (instructive materials and classroom, clinical, and distance-learning programs) that will open the opportunity to enter our profession to an increasing number of aspiring young technologists.
Speaking from my perspective as a volunteer leader with BRPT, I believe each of us in the field has a role to play in strengthening our profession. There are volunteer opportunities available in each of the sleep-related professional organizations. Together and separately, your professional organizations work to shape the broader agenda for our field, and I encourage you to be part of that process. And each of us, technologists and managers alike, has an opportunity to serve as an ambassador for our discipline within the sleep community, and within the broader allied health community, and to individuals interested in a career in sleep. SR
Janice East, RPSGT, R. EEG T., is president of the Board of Registered Polysomnographic Technologists (BRPT). East is also the director of sleep disorders, neurodiagnostics, and rehabilitation services for Morton Plant Mease Health Care.






