An old surgical technique is now being used from infancy to adulthood for the treatment of sleep disordered breathing
Sleep disordered breathing affects all age groups. The management of the infant to adult patient population will differ depending on the site and cause of obstruction. The role of two different surgical modalities in the treatment of these patients will be presented. Distraction osteogenesis, a technique originally described to lengthen long bones, has been used successfully in the treatment of infants, adolescents, and adults with sleep disordered breathing created by the micrognathic mandible. Developmentally, the micrognathic mandible is associated with many syndromes including, but not limited to, Pierre Robin sequence, Stickler’s syndrome, Treacher Collins syndrome, its variants, and Goldenhar’s syndrome. Distraction osteogenesis is new to the armamentarium of surgeons who perform facial and cranial osteotomies. The prime advantage of distraction osteogenesis is that it slowly stretches the soft tissues and bone, allowing for greater advancement than standard corrective techniques. Moving the bone in this manner will also allow for the airway opening to be titrated to some extent. This is similar to the titration accomplished when using an adjustable mandibular advancement device.
Distraction Devices
Distraction devices are basically two bone plates that are connected with an expansion screw. The plates stabilize the bone segments after they are separated (osteotomy), and the screw controls the degree and rate of separation of the segments. Once the osteotomy is completed and a blood clot is allowed to form between the two segments, the expansion screw is turned at a rate of 1 mm/day to push the segments apart, placing the bone and clot under tension and thereby stimulating osteogenesis. Once an end point is reached, the expansion screw is stabilized and the new bone is allowed to consolidate (calcify). Most devices allow for growth in only one direction; however, devices are also available that will allow for not only anterior to posterior movement but vertical and lateral moves as well.
Orthognathic Surgery
Corrective jaw surgery, commonly referred to as orthognathic surgery, is a technique that can be used in the adult patient population with good predictability and stability. This technique is the workhorse of skeletal facial corrections. Both distraction osteogenesis and orthognathic surgery use the principle of moving the lower and upper jaw into an anterior position, thereby taking with it the soft tissue attachments of the airway and enlarging the airway. The advancement, if large enough, prevents the collapse of the airway during sleep. These changes are documented with the appropriate sleep studies and radiographic films.
Pre- and post-operative polysomnography is necessary to document the improvement that occurs with the surgical manipulation of the jaws. Surgical protocols have been developed for corrective jaw surgery and are well documented.2,5 Distraction techniques are only recently recognized as a method of treatment for sleep disordered breathing. This has been documented in the literature as case studies.1-4
 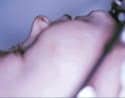 Figure 1. Pre- and post-distraction lateral photographs. Right side with consolidation rods in place. Note the advancement of the anterior mandible. |
Case 1
A 6-week-old female infant with Pierre Robin sequence was seen in consultation in the neonatal intensive care unit. Acute airway distress dictated that the surgeons manage the airway first with lip to tongue adhesions (suturing the tongue to the lip). Two attempts at stabilizing the infant’s airway this way failed. The next step was to place a tracheostomy tube.
The plastic and reconstructive surgeon had asked for consultation regarding possible distraction of the infant’s airway. Appropriate chest tomography scans of the mandible and airway and documentation of respiratory distress with desaturations to 70% were noted. An external three-dimensional distraction device was chosen to maintain control of the bilateral osteotomies that would need to be done for the mandibular lengthening process.
The infant’s airway was maintained with a nasopharyngeal airway after the surgery and advancement took place on day 3 postoperative. The mandible had advanced a total of 13 mm. As the mandible was brought into its new position, the patient’s oxygen saturation improved dramatically to 98% on room air. The distractors were left in place to allow for consolidation of the new bone and were removed once radiographic confirmation of calcification occurred at the distraction site. The patient has remained free of obstruction for the past 2 years and is growing well.
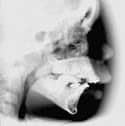  Figure 2. Pre- and post-operative lateral cephalometric films note opening of the posterior airway on film after advancement. Distraction device in place on right advanced mandible. |
Case 2
An 11-year-old male with Stickler’s syndrome was diagnosed with obstructive sleep apnea (OSA) on polysomnography. His skeletal examination revealed a cleft palate and mandibular micrognathia. He was sent for evaluation for possible mandibular advancement with distraction osteogenesis therapy; the surgical plan was to advance the mandible with bilateral intraoral distraction devices.
Bilateral mandibular osteotomies were done and the intraoral devices placed. The mandible was distracted and advanced a total of 12 mm. Noticeable clinical advancement with improvement in the sleep pattern and a decrease in snoring resulted. The patient’s new bone was allowed to consolidate for 3 months prior to removing the distraction devices. A follow-up polysomnograph was obtained, which confirmed a patent airway and resolution of his sleep disordered breathing condition. This patient has maintained the correction with normal growth for the past 3 years.
Case 3
A 48-year-old male with OSA diagnosed by polysomnography was seen to be evaluated for reconstructive jaw surgery. His RDI was 57.2 and classified as severe sleep disordered breathing. His oxygen saturations were down to 86%. Skeletal analysis revealed mandibular retrognathia with maxillary deficiency. The treatment plan was to remove the lower first bicuspids and retract the lower anterior teeth. This would set the patient up for maximum skeletal advancement with good dental function. He underwent maxillary LeFort I osteotomy with advancement of the maxilla and bilateral sagittal split advancement osteotomies of the mandible. His total advancement was 10 mm bilaterally.
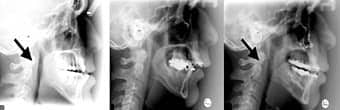 Figure 3. Lateral cephalometric analysis of pretreatment, presurgical, and postadvancement of the maxilla and mandible. Note change in the posterior airway. Both the maxilla and mandible were advanced in this patient. |
The patient’s airway has opened as seen on lateral cephalometric film. Clinically, he had oxygen saturation of 98% on room air. His polysomnogram is pending final analysis as the patient is only 2 months postoperative. His clinical symptoms of daytime somnolence have disappeared and he has stopped snoring.
Conclusion
The surgical approach selected to treat sleep disordered breathing caused by mandibular insufficiency is dependent on many factors including the age of the patient. Children and petite patients have less bone available for conventional osteotomy surgery. Mandibular growth, the development of the teeth (teeth buds), and occlusion are challenges that must be considered when designing osteotomies for advancement. Distraction osteogenesis helps to overcome many of these obstacles when applied to the entire patient population and gives us a new tool to treat pediatric patients. Most age groups can now be managed safely and predictively with mandibular advancement surgery. Distraction osteogenesis provides a valuable tool that gives us the ability to both prevent and correct the development of sleep disordered breathing.
Stephanie J. Drew, DMD, is an oral maxillofacial surgeon at The New York Center for Orthognathic and Maxillofacial Surgery, West Islip, NY.
References
1. Cohen SR, Simms C, Burstein FD. Mandibular distraction osteogenesis in the treatment of upper airway obstruction in children with craniofacial deformities. Plast Reconstr Surg. 1998;101:312-318.
2. Cohen SR, Ross DA, Burstein FD, Lefebvre JL, Riski JE, Simms C. Skeletal expansion combined with soft-tissue reduction in the treatment of obstructive sleep apnea in children: physiologic results. Otolaryngol Head Neck Surg. 1998;119:476-485.
3. Monasterio FO, Drucker M, Molina F, Ysunza A. Distraction osteogenesis in pierre robin sequence and related respiratory problems in children. J Craniofac Surg. 2002;13:79-83.
4. Li KK, Powell NB, Riley RW, Guilleminault C. Distraction osteogenesis in adult obstructive sleep apnea surgery: a preliminary report. J Oral Maxillofac Surg. 2002;60:6-10.
5. Li KK, Powell NB, Riley RW, Troell RJ, Guilleminault C. Long-term results of maxillomandibular advancement surgery. Sleep Breath. 2000;4:137-140.






