Many medications have the potential of affecting sleep, and thus, the polysomnogram. A number of medications are specifically designed to influence sleep, while for others the influence over sleep is considered a side effect. Generally, these medications can be grouped as follows: those specifically indicated for the induction and maintenance of sleep; those with other indications that also significantly alter sleep; and medications that indirectly interfere with sleep (eg. an ill-timed diuretic). Understanding the basics of these various sleep effects is essential to a thorough and accurate interpretation of an overnight sleep study.
 |
| Click on picture for larger version. |
MEDICATIONS AND SLEEP: BASIC PRINCIPLES
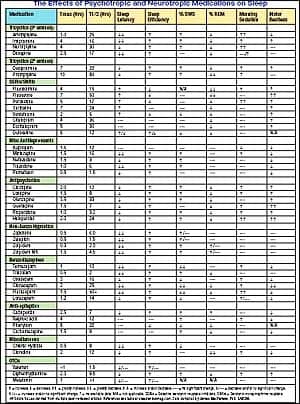
A number of factors need to be considered when determining how a medication is influencing sleep. One of these factors, Tmax, is defined as the time taken for a drug to reach a peak plasma level and thus the onset of action. It is an important consideration with regard to instructing a patient as to when to take a medication. The timing of administration will determine when the drug is providing the most profound effect (or side effect).
The rate of elimination of a drug is measured as a time-constant based on plasma concentration. T1/2 is defined as the time taken for a drug to reach exactly half of the original peak plasma level. The net result of these various kinetic properties determines the duration of action of a drug.
Besides considering duration of action, sleep medicine professionals should also consider how medications influence sleep latency, sleep efficiency, percentage of slow wave sleep, percentage of rapid eye movement, morning sedation, and motor restlessness. The effect that psychotropic and neurotropic medications have on these parameters is shown in the table.
Sleep-wake effects are often a major consideration when optimizing pharmacological interventions. Maximizing desirable effects and minimizing side effects can often be a function of appropriate medication dosing and dose timing. The overnight sleep laboratory investigation provides a unique opportunity to take a medication inventory. Careful confirmation and documentation of medications by the technicians can provide some of the most important data in the comprehensive investigation of disordered sleep.
James MacFarlane, PhD, DABSM, is assistant professor, Departments of Paediatrics and Psychiatry, University of Toronto. He is also director of education at the Toronto Sleep Institute.
BIBLIOGRAPHY
- Hardman JG, Limbird LE, Goodman AG, eds. Goodman & Gilman’s The Pharmacological Basis of Therapeutics. 11th ed. New York: McGraw-Hill; 2006.
- Compendium of Pharmaceuticals and Specialties—CPS (2008), Canadian Pharmacists Association, National Library of Canada.