By Martin A. Denbar, DDS, Greg K. Essick, DDS, PhD, and Preetam Schramm, PhD, RPSGT
A 37-year-old nonobese male with a diagnosis of severe obstructive sleep apnea (OSA), moderate central sleep apnea (CSA), and periodic limb movements in sleep (PLMS) is scheduled for Army deployment and needs to have his sleep-disordered breathing (SDB) under control. Trials of continuous positive airway pressure (CPAP), bi-level PAP, and auto-CPAP and adaptive servo-ventilation bi-level PAP (ASV-BiPAP) combined with mandibular advancement were attempted. The therapies did not fully resolve the patient’s sleep-disordered breathing, although the patient’s intolerance to PAP therapy was addressed satisfactorily when combined with an oral appliance. Retrospective novel analyses of the patient’s PSG data based on cardiopulmonary coupling (CPC) revealed that sleep quality was impaired by the presence of both refractory complex sleep apnea and PLMS.
DIAGNOSIS AND THERAPY HISTORY
In November 2007, the patient was diagnosed with severe sleep apnea and significant periodic limb movements following a split-night study protocol (Table 1). The respiratory events were more dominant in non-REM sleep (approximately x2) than in REM sleep. Pulse oximetry showed saturation remained within normal limits with a mean of 95% and nadir at 91% Spo2. CPAP administered up to 10 cm H2O reduced the hypopnea index (HI), central apnea index (CAI), and snoring from 66 to 3 events/hr. At home, the patient was unable to tolerate a full face mask, and a nasal mask proved ineffective due to mouth breathing.
A second sleep study in April 2008 demonstrated that bi-level positive airway pressure (BiPAP) with inspiratory and expiratory pressures of 16 and 12 cm H2O, respectively, and backup rate of 10 breaths/minute reduced his HI and CAI (Table 1).
In May 2010, the patient reported an inability to tolerate the BiPAP therapy. In addition, the mask and hose restricted his movements, made him claustrophobic, and caused an unconscious need to remove the mask, and the therapy seemed ineffective. His overseas Army deployment was set to take place in July and he was required to have his sleep-disordered breathing under control.
MEDICAL HISTORY
The patient is a 5’6″, 200 lb male in excellent physical condition. His medical history was unremarkable except for asymptomatic ulcerative colitis and sleep apnea. He was unmedicated and reported occasional nasal stuffiness at night, gasping upon arousals from sleep, excessive daytime sleepiness, and tiring easily. He was not under treatment by a physician for periodic limb movements or restless leg syndrome. His Epworth Sleepiness Scale score was 19 of 24, indicative of moderate-to-severe daytime sleepiness1 and his Fatigue Severity Scale score was 42 of 63, indicative of a clinically significant fatigue.2
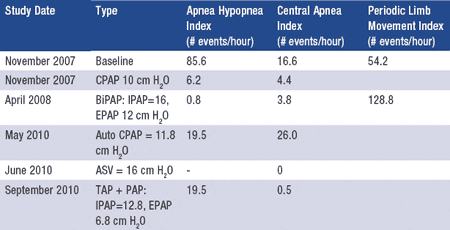
Table 1. Summary of patient’s respiratory events and periodic limb movement indices during sleep. Abbreviations: ASV = adaptive servo ventilation; CPAP = continuous positive airway pressure; EPAP and IPAP = expiratory and inspiratory positive airway pressure, respectively; TAP = Thornton Adjustable Positioner.
OROFACIAL EXAMINATION
Upon extraoral examination, the patient’s head, eyes, ears, nose, throat, and neck were within normal limits. The temporomandibular joints were found to be normal and asymptomatic as were the muscles of mastication. The patient exhibited normal jaw opening and protrusive capabilities. Intraoral examination of the soft tissues revealed a low tongue with mildly scalloped lateral borders, Class 1 Mallampati classification,3 Grade 1 tonsils,4 and unremarkable uvula and soft palate.
Examination of the teeth revealed a Class I occlusion with attrition of the posterior teeth, suggestive of active or prior bruxism and clenching. Large mandibular tori were present bilaterally. The periodontium was healthy. Radiographic examination based on a pretreatment panorex was normal.
TREATMENT PLAN AND DELIVERY
The treatment plan involved i) mandibular advancement and stabilization with an oral appliance, and ii) the addition of positive airway pressure using nasal pillows. Dental impressions and an interocclusal bite record were taken. In 4 days, the patient returned for delivery of a Thornton Adjustable Positioner (TAPIII) oral appliance. The jaw position was set at roughly 1 mm past his active maximum protrusion. The upper component of the appliance was modified to provide physical support and positional stability for nasal pillows using an assembly kit (TAP-PAP Chairside, Airway Management Inc, Dallas). The result was such that no ancillary headgear was required to hold and stabilize the oral appliance and nasal pillows together (Figure 1). The patient was lent an auto-titrating CPAP machine (REMstar Auto-CPAP with C-Flex; Respironics, Murrysville, Pa).
TREATMENT PROGRESS AND ASSESSMENT
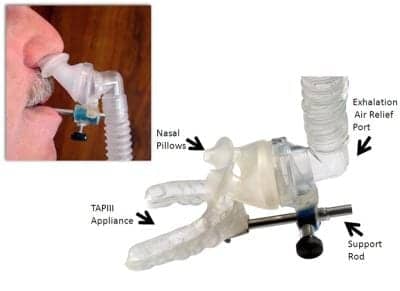
Figure 1. The TAP-PAP Chairside assembly, showing modification of the upper component of the oral appliance to support nasal pillows. The lower component of the oral appliance (not shown) is not modified. Inset shows TAP-PAP in mouth.
Over the initial period of wear from May 27, 2010 through June 22, 2010, the data recorded by the PAP machine indicated that therapy was used an average of 6 hours, 17 minutes per night indicating good adherence.5 The average CPAP pressure delivered was 11.8 cm H2O. There were no major leaks, attesting to the three-dimensional positional stability of the nasal pillows against the external nares. However, the number of obstructive apneas + hypopneas averaged 19.5/hr and the CAI averaged 26/hr (Table 1). With increasing pressure, the frequency of central events decreased; however, the patient’s frequency of obstructive apneas and hypopneas combined remained the same.
On June 28, 2010, the patient underwent a laboratory sleep study with the aim of determining a pressure regimen that would normalize his sleep respiration with the hybrid therapy. The patient exhibited a high frequency of arousals (RERAs) in non-REM sleep. In general, the frequency of central events increased and RERAs decreased with increases in the PAP inspiratory pressure (Figure 2). With adaptive servo-ventilation and a pressure of 16 cm H2O, the central respiratory events were eliminated according to standard scoring practice (Table 1). With BiPAP, ASV, and pressures within the range of 9 to 11 cm H2O, no central events were observed, although the patient continued to have RERAs.
The patient was deployed on schedule. Correspondence indicated that the initial symptoms of excessive daytime sleepiness, nighttime gasping, and tiring, and his quality of life, had significantly improved with therapy use. The September 2010 data from his BiPAP machine indicated that the hybrid therapy was used for an average of 7 hours, 12 minutes. The average respiration rate was 14.4 breaths/min, 84.2% of which were patient initiated. The 90th percentile EPAP was 6.8 cm H2O. An average 6 cm H2O pressure was added during inspiration, corresponding to an IPAP of 12.8 cm H2O. Therapy response showed negligible obstructive and central apnea indices, although significant hypopneas persisted (Table 1).
CARDIOPULMONARY COUPLING ANALYSIS
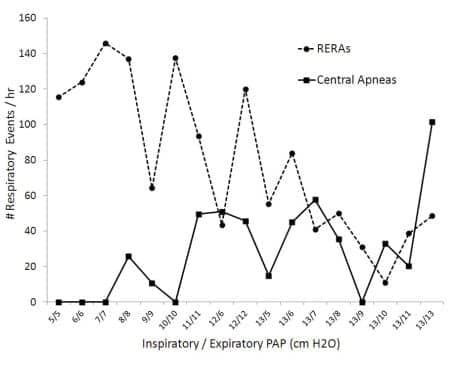
Figure 2. Polysomnography results conducted in June 2010. Shown are the RERA index and central apnea index at different inspiratory (IPAP) and expiratory (EPAP) pressures that were used in an attempt to eliminate the patient’s sleep-disordered breathing (PAP titration). No obstructive apneas or hypopneas were observed at these pressures.
CPC analysis used as an adjunct to standard PSG scoring criteria is an automated method that phenotypes sleep-disordered breathing and objectively measures sleep quality in patients with SDB. The ECG-based algorithm estimates the coupling of heart rate variability and R-wave amplitude variations induced by respiration.6 The high frequency coupling (HFC, 0.1-0.4 Hz) band is associated with physiological respiratory sinus arrhythmia, stable sleep, and respiration. Low frequency coupling (LFC, 0.01-0.1 Hz) is associated with unstable sleep or periodic sleep behaviors including sleep apnea. The algorithm can detect putative strong chemoreflex modulation of sleep-breathing and complex SA.7 The spectral biomarker for complex SA is elevated LFC narrow band coupling.
A retrospective assessment of the ECG from the PSG data using CPC analysis was performed (Table 2). HFC or stable sleep was decreased across all studies compared to expected normal adult values.8 LFC or unstable sleep was elevated in all studies compared to expected normal adult values. Very low frequency coupling (VLFC) was within normal limits. The putative spectral biomarker for periodic type events, e-LFC narrow band was present in all PSG studies. For each sleep study, contributions to the e-LFC narrow band were observed from both central apnea events and PLMS (Figure 3). Elevated-LFC broad band is a subset of LFC that is associated with fragmented sleep of various etiologies and was high in all studies. The HFC/LFC ratio, a metric of sleep quality, was below expected normal adult values.
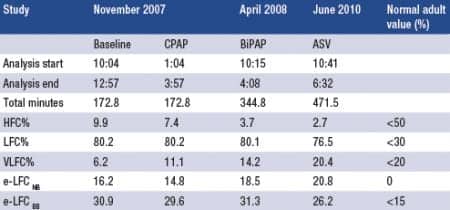
Table 2. Summarized cardiopulmonary coupling data. Abbreviations: HFC = high frequency coupling band (0.1 – 0.4 Hz); LFC = low frequency coupling band (0.01-0.1 Hz); VLFC = very low frequency coupling band (0.0039 – 0.01 Hz); e-LFC = elevated-low frequency coupling (0.006 – 0.01 Hz); NB = narrow band; BB = broad band.
DISCUSSION
Patients with sleep-disordered breathing have predominate obstructive apnea without (84%) or with (15%) a central component.9 Unlike the patient in this report, the central component is usually not observed until CPAP is instituted and the terms “treatment-emergent central apnea” or “complex sleep apnea” have been coined to describe this clinical phenomenon.9,10 Some clinical investigators have argued that complex sleep apnea represents only a side effect of PAP therapy.11 Others have maintained that complex sleep apnea is a distinct disease.12,13 Because the patient in this report experienced central sleep apnea before any therapy initiation and was validated by the presence of e-LFC narrow band on baseline PSG, the latter position gains support. Similar findings of e-LFC narrow band during diagnostic PSGs prior to PAP therapy were identified by Thomas et al as individuals with complex sleep apnea prior to therapy.7
Such individuals exhibit high upper airway resistance/obstruction and dysregulation of respiratory control. Even subtle increases in ventilation can potentially drive the PaCO2 below the breathing (apnea) threshold level, resulting in loss of the impetus to breathe.14-17 Unlike most patients with pure obstructive disease, these individuals often exhibit more severe obstructive disease, short cycles of obstructive apnea, disordered breathing predominantly in non-REM sleep rather than REM sleep, less severe oxygen desaturations, an incomplete response to positive airway pressure, and arousals during sleep that are difficult to suppress with PAP.9,12,17 It is worth noting that the patient described in this report exhibited all of these previously reported characteristics.
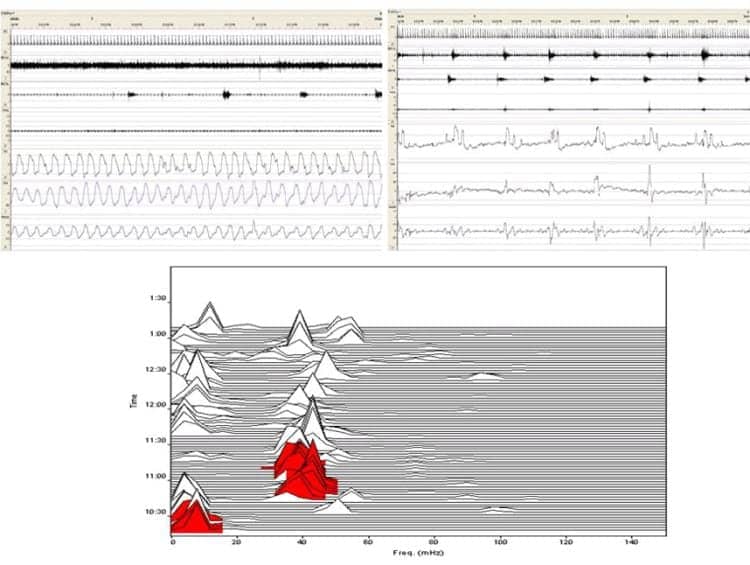
Figure 3. The lower panel illustrates the low frequency cardiopulmonary coupling (CPC) band sleep spectrograph in a 90° view generated from the patient’s ECG data recorded during the April 2008 sleep study. The X-axis has the coupling frequency in mHz, and clock time in hours is on the Y-axis. At about 10:54 PM, the spectrographic biomarker shows putative strong chemoreflex modulation of sleepbreathing indicated by the elevated low frequency narrow band coupling at a frequency of 39 mHz (red peaks). The top right panel shows the PSG airflow and respiratory effort channels with CSA occurring at this time during the administration of BiPAP. From top to bottom, the channels are EKG, EMG-chin, EMG-Anterior Tibialis left and right, airflow, respiratory effort thoracic and abdominal. The coupling frequency is faster when chemoreflex influences are strong, reminiscent of the short respiratory event cycles of altitude-induced periodic breathing. The top left panel shows the PSG trace at about 10:30 PM with an absence of CSA but with periodic limb movements in sleep on the left EMG-Anterior Tibialis channel. The periodicity is captured and displayed as red peaks at a coupling frequency of <20 mHz in the spectrogram.
In clinical practice, identification of an effective therapy for complex sleep apnea is largely empirical and often involves, in turn, trials of CPAP, BiPAP, and O2 supplementation or ASV with a backup rate of respiration.18-20 It has been suggested that therapy directed at minimizing hypocapnia, such as the use of lower positive airway pressures and benzodiazepines to suppress arousals that can evoke hyperventilation, should be considered as it more directly targets the underlying pathophysiology.12,17,21 To this end, lower CPAP pressures have been shown to reduce alveolar and arterial levels of CO2 less than higher CPAP pressures.22,23 Thus, one would predict a general utility of mandibular advancement splints in concert with positive airway pressure therapies for patients who are susceptible to hypocapnic central apnea.24-26
Even though the patient was adherent to the final therapy, none of the PAP therapies proved effective in normalizing the patient’s sleep respiration or eliminated e-LFC narrow band coupling. However, the low moderate level of residual hypopneas that persists (total AHI = 20.8 events/hr) contrasts favorably to the patient’s intolerance to PAP and baseline AHI of 102.2 events/hr prior to treatment with the hybrid therapy. PLMS remained existent and CPC analysis confirmed their negative effect on sleep quality. Additional study is indicated to evaluate pharmacological intervention for treating PLMS in combination with TAP-PAP therapy for treating his upper airway resistance.
This is the first reported case of complex SA with PLMS identified with CPC analysis showing separate frequencies for CSA and PLMS associated with unstable sleep. Congestive heart failure patients with CSA and OSA show a respiratory rate with a frequency of 0.031 Hz.27 The PLMS in this case had a lower frequency of <0.02 Hz resulting in a PLM index of 72 events/hr, which would approximate the patient’s mean of 91 events/hr from the two recordings in which movements were counted.
Martin A. Denbar, DDS, is with Austin Apnea and Snoring Therapy, Austin, Tex; Greg K. Essick, DDS, PhD, is with the Department of Prosthodontics and Center for Neurosensory Disorders, School of Dentistry, University of North Carolina, Chapel Hill; and Preetam Schramm, PhD, RPSGT, is with Arbeitsgemeinschaft Wissenschaftliche Psychotherapie-Freiburg, Freiburg, Germany. The authors would like to recognize Jennifer York, MD, of Texas Neurology Center, Austin, for collaborating on a sleep study, and Jonathan Weisner and Thomas Pardue for assistance with preparation of the report.
References
- Johns MW. A new method for measuring daytime sleepiness: the Epworth Sleepiness Scale. Sleep. 1991;14:540-545.
- Krupps LB, LaRocca NG, Muir-Hash J, Steinberg AD. The Fatigue Severity Scale: application to patients with multiple sclerosis and systemic lupus erythematosus. Arch Neurol. 1989;46:1121-1123.
- Mallampati S, Gatt S, Gugino L, et al. A clinical sign to predict difficult tracheal intubation: a prospective study. Can Anaesth Soc J. 1985;32:429–34.
- Friedman M, Tanyeri H, La Rosa M, et al. Clinical predictors of obstructive sleep apnea. Laryngoscope. 1999;109:1901-1907.
- Department of Health and Human Services, Centers for Medicare & Medicaid Services. Decision memo for continuous positive airway pressure (CPAP) therapy for obstructive sleep apnea (OSA). CAG#0093R. March 13, 2008.
- Thomas RJ, Mietus JE, Peng CK, Goldberger AL. An electrocardiogram-based technique to assess cardiopulmonary coupling during sleep. Sleep. 2005;28:1151-61.
- Thomas RJ, Mietus JE, Peng CK, et al. Differentiating obstructive from central and complex sleep apnea using an automated electrocardiogram-based method. Sleep. 2007;30:1756-1769.
- Yang AC, Yang CH, Hong CJ, et al. Sleep state instabilities in major depression disorder: detection and quantification with electrocardiogram-based cardiopulmonary coupling analysis. Psychophysiology. 2010;Jul 6, Epub.
- Morgenthaler TI, Kagramanov V, Hanak V, et al. Complex sleep apnea: is it a unique clinical syndrome? Sleep. 2006;29:1203-1209.
- Javaheri S, Smith J, Chung E. The prevalence and natural history of complex sleep apnea. J Clin Med. 2009;5:205-211.
- Malhotra A, Bertisch S, Wellman A. Complex sleep apnea: it isn’t really a disease. J Clin Sleep Med. 2008;4:1-2.
- Gilmartin GS, Daly RW, Thomas RJ. Recognition and management of complex sleep disordered breathing. Curr Opin Pulm Med. 2005;11:485-93.
- Gay PC. Complex sleep apnea: it really is a disease. J Clin Sleep Med. 2008;4:403-405.
- Dernaika T, Tawk M, Nazir S, Younis W, Kinasewitz G. The significance and outcome of continuous positive airway pressure-related central sleep apnea during split-night sleep studies. Chest. 2007;132:81-87.
- Dempsey JA. Crossing the apnoeic threshold: causes and consequences. Exp Physiol. 2004;90:13-24.
- White DP. Pathogenesis of obstructive and central sleep apnea. Am J Respir Crit Care Med. 2005;172:1363-1370.
- Suzarla SM, Thomas RJ, Abramson ZR, Kaban LB. Biomechanics of the upper airway: changing concepts in the pathogenesis of obstructive sleep apnea. Int J Oral Maxillofac Surg. 2010;39:1149-1159.
- Thomas RJ, Daly RW, Weiss JW. Low-concentration carbon dioxide is an effective adjunct to positive airway pressure in the treatment of refractory mixed central and obstructive sleep-disordered breathing. Sleep. 2005;28:69-77.
- Becker K, Wallace JM. Central sleep apnea. eMedicine Medscape. 2010. emedicine.medscape.com/article/304967-overview. Accessed April 22, 2011.
- Issa FG, Sullivan CE. Reversal of central sleep apnea using nasal CPAP. Chest. 1986;90:165-171.
- Thomas RJ. Effect of added dead space to positive airway pressure for the treatment of complex sleep disordered breathing. Sleep Med. 2005;6:177-8.
- Bjurstedt H, Rosenhamer G, Lindborg B, Hesser CM. Respiratory and circulatory responses to sustained positive-pressure breathing and exercise in man. Acta Physiol Scand. 1979;105:204-214.
- Ellingsen I. The influence on the breathing pattern in man of moderate levels of continuous positive and negative airway pressure and of positive end-expiratory pressure during air and CO2 inhalation. Acta Physiol Scand. 1990;138:273-282.
- El-Solh AA, Moitheennazima B, Akinnusi ME, Churder PM, Lafornara AM. Combined oral appliance and positive airway pressure therapy for obstructive sleep apnea: a pilot study. Sleep Breath. May 2011;15(2):203-208. Epub 2010 Nov 10.
- Thornton WK. Combined CPAP-oral appliance therapy. Sleep Review. 2002. www.sleepreviewmag.com/issues/articles/2002-01_09.asp. Accessed April 22, 2011.
- Denbar MA. A case study involving the combination treatment of an oral appliance and auto-titrating CPAP unit. Sleep Breath. 2002;6:125-128.
- Ryan CM, Bradley TD. Periodicity of obstructive sleep apnea in patients with and without heart failure. Chest. 2005;127:536-542.






