Oral appliance efficacy studies are paving the way for greater utilization of the sleep apnea therapy.
While oral appliances have been used to treat mild to moderate obstructive sleep apnea (OSA) for several decades, they continue to be prescribed much less frequently than CPAP. One reason is basic: Oral appliances aren’t efficacious in all patients. But oral appliance manufacturers, plus makers of oral appliance success-predicting technologies, are striving to change that via efficacy studies.
Zephyr Sleep Technologies has developed a method, the MATRx system, that can determine the likelihood of success and predict which patients will be successful using an oral device. John Remmers, MD, chief medical officer for Zephyr Sleep Technologies, says there are currently 90 systems in use with about a 93% overall success rate. Studies are further evaluating the efficacy of the system.
Another new oral appliance success predictor is prefab device ApneaRX by ApneaSciences, which is patient-titrated and, per a feasibility study, accurate in predicting patients who will respond positively to oral appliances.1
Zephyr’s Remmers knows there is still an uphill climb to make oral appliances more widely prescribed, but he is “cautiously optimistic” that with the success of the MATRx system, and numerous studies that have measured the efficacy of oral appliances, oral appliance use is at a tipping point for greater use and acceptance.
“Changing the practice of medicine is hard, but the conventional way that sleep medicine is practiced is too cookie cutter,” Remmers says. “The modern approach needs to be what is optimal for the patient, but that’s not what we do today in sleep medicine.”
Measuring Patient Preference

A study using a SomnoMed appliance showed important health outcomes were similar after 1 month of optimal oral appliance and CPAP treatment in patients with moderate-severe OSA.
Conventional wisdom has it that patients prefer oral appliances over CPAP. Thanks to a recent study using its SomnoDent device, SomnoMed has evidence to back up this claim.2
“The outcomes of treatment for OSA depend on two factors: one is how effective the treatment is and the second is how compliant is the patient with treatment,” says Jagdeep Bijawadia, MD, SomnoMed’s chief medical officer. “CPAP may be extremely effective, but if the patient does not use the CPAP, it will not have impact on health outcomes. With the new microrecorder technology, we can now, for the first time, objectively measure compliance with the oral appliance.”
And with regard to effectiveness, two recent studies using the SomnoDent device show the health benefits patients receive from using an oral appliance.
A study published in the American Journal of Respiratory and Critical Care Medicine examined the efficacy and health benefits of oral appliances compared to CPAP across the range of sleep apnea severity from mild to severe OSA patients.2
“The study found that our oral appliance was associated with similar health outcomes across a whole range of health outcomes—driving simulator, blood pressure, arterial stiffness, and quality of life,” Bijawadia says.
A second study, which appeared in the journal Respirology, examined the cardiovascular mortality in patients with moderate to severe OSA who had failed CPAP.3
“The investigators found no difference in the mortality of the groups that used CPAP versus the ones that used oral appliances in terms of cardiovascular mortality—and both groups did much better than untreated patients,” Bijawadia says.
For Bijawadia, the tipping point for oral appliance use may be happening now.
“A combination of three factors is currently occurring: new outcome-based evidence for oral appliances; new technologies—the microrecorder for compliance and predictive tools like the MATRx system; and the economics—over a period of 3 to 5 years, oral appliances are more cost-effective than CPAP.”
Driving Research
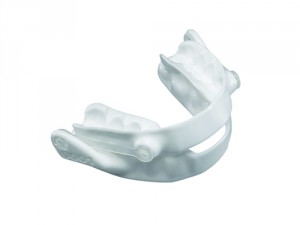
In addition to the Orcades study, ResMed’s Narval has been utilized in a number of other key studies.
Recognizing the need for extensive clinical data, ResMed is driving what it says is the largest French oral appliance study to date. The ongoing Orcades Study is a prospective 28-center observational cohort study providing long-term data on 300 OSA patients treated with a ResMed custom-made Narval CC MRD (mandibular repositioning device).
Preliminary data have shown a high success rate (79%) regardless of OSA severity. The breakdown of patients by severity from mild to moderate to severe was 16%, 41%, and 42%, respectively.4
At the 3- to 6-month assessment, AHI was, respectively, <5 and <10/h in 38% and 66% of patients, leading researchers to conclude that Narval CC is an effective therapy for moderate to severe OSA and can be used for patients refusing or noncompliant with CPAP, according to ResMed.
While ResMed offers CPAP, the ongoing investigation of the efficacy of oral appliances is important in providing optimal treatment to patients.
“With CPAP as the gold standard in sleep apnea therapy, it is important to be able to offer similar success metrics in additional modes of therapy,” says Annie McBride, America’s dental sleep product manager for ResMed. “Physicians and dentists need confidence that an oral appliance like Narval CC is treating the patients’ chronic OSA optimally….Simply knowing that a patient is wearing an oral appliance is not enough. There are a number of stakeholders, including doctors, dentists, payors, associations, and patients who need objective efficacy data to make decisions around what appliances to use in their practice, which patients are candidates, and what appliances to reimburse.”
Making a Strong Impression
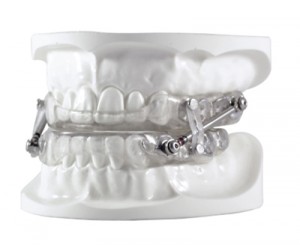
Strong Dental has donated its oral appliances to researchers for studies and plans to do its own studies in the future.
Strong Dental has yet to begin efficacy studies of its SUAD family of FDA-cleared oral sleep appliances, although this is definitely on the drawing board for the future. It is especially interested in creating a study that shows the strength and durability of the SUAD device.
“Although there are no studies that were specifically conducted for our appliances, we have donated our Herbst model to certain companies and corporations that have conducted recent studies on this specific style of mandibular repositioning devices,” says Patrick J. Strong, DD, FCAD, president and CEO of Strong Dental.
The importance of compliance is a key factor in proving the efficacy of oral appliances for Strong Dental.
“We have found that the manufacturer, the prescriber, the treating doctor, as well as the patient have all held an interest in the efficacy of oral appliances’ compliance measurement, which has been used in sleep therapy for years with numerous benefits,” Strong says. “Extending those benefits into oral appliance therapy would be beneficial for all. Furthermore, showing efficacy levels the playing field for oral appliance therapy. With the number of practitioners we see getting more involved, it’s only a matter of time before the insurance payors require monitoring just as in CPAP therapy.”
Efficacy studies will be the tipping point to get the support of a key player in the oral appliance equation, Strong says. “We believe that more efficacy studies will act as a catalyst for several insurance companies that do not currently cover the cost of oral appliances to change their rates,” he says.
Advancing NonCustom Devices

Airway Management’s “Precision Fit” technology allows for accurate molding without bite registration and lab fabrication. The company is in talks with researchers to collect clinical data on the device.
“While CPAP is easy and the gold standard,” says Alastair McAuley, consultant to Airway Management, compliance is poor. “It’s only about 40% to 50% long-term,” he says.
There are a number of reasons why only about 4% to 5% of patients are being treated using an oral appliance. Among the biggest barriers is the cost.
Airway Management is hoping to change this with its myTAP device. The noncustom oral appliance debuted in late 2013 and, according to McAuley, has the “fit and feel” of a custom device. “However, it’s not a custom device by definition, because a mold of the patient’s teeth isn’t being made,” he says.
The device also comes with a 30-day satisfaction guarantee, similar to a CPAP mask guarantee, according to McAuley.
Built off the work of the company’s founder Keith Thornton, DDS, and its earlier TAP custom device, the myTAP is a low-cost customizable device that could give oral appliances the push they need for wider clinical acceptance, according to McAuley. “You’ll increase patient access, if you decrease the cost,” he says.
But a low-cost device isn’t enough. The company wants to get clinical data, another of the necessary tipping points, McAuley says, to demonstrate the device’s efficacy. McAuley has recently had meetings with researchers in New Zealand and Australia to discuss implementing studies of the myTAP device.
The Australian researcher had a prediction about the myTAP device during the meeting, according to McAuley: “It’ll be disruptive if it works.” SR
C.A. Wolski has been writing for Sleep Review since 2001. He has seen firsthand the difficulties family members have had using CPAP devices, and, in the wake of his research for this article, is going to recommend that they investigate the use of oral appliances.
REFERENCES
1. Hwang D, et al. Feasibility Pilot Evaluating the Use of Pre-Fabricated Titratable Mandibular Advancement Device for Management of Obstructive Sleep Apnea. Poster presented at SLEEP 2014.
2. Phillips CL, Grunstein RR, Darendeliler MA, et al. Health outcomes of continuous positive airway pressure versus oral appliance treatment for obstructive sleep apnea: a randomized controlled trial. Am J Respir Crit Care Med. 2013;187(8):879-87.
3. Anandam A, Patil M, Akinnusi M, Jaoude P, El-Solh AA. Cardiovascular mortality in obstructive sleep apnea treated with continuous positive airway pressure or oral appliance: an observational study. Respirology. 2013;18(8):1184-90.
4. Vecchierini MF, et al. Orcades, Aaprospective multicentre cohort study of obstructive sleep apnea (OSA) patients treated with a custom-made mandibular repositioning device (MRD); 6 month data. Poster presented at SLEEP 2014.






