Collaborating with dentists can help physicians treat obstructive sleep apnea patients who are otherwise failing PAP therapy.
The field of sleep dentistry is becoming widely recognized among healthcare professionals, but the full impact of dentistry on the treatment of obstructive sleep apnea (OSA) has not been recognized by most clinicians in the field of sleep.
To overcome this shortsightedness, dentists first need to become more knowledgeable on the variety of treatments for OSA, and specifically on the medical therapeutic option of positive airway pressure (PAP). Dentists will benefit if they understand how they can assist in the care of patients who are PAP intolerant and in whom oral appliance therapy alone is not sufficient to treat their condition.
Similarly, physicians need to recognize that the temporomandibular joint (TMJ) is the “joint of the airway,” and mandibular stabilization and its proper positioning can be critical for optimal PAP therapy.
National statistics on PAP compliance have shown discouraging results, with nightly utilization as low as 51% in some studies but up to 80% in others.1,2 Clearly some groups have found ways to enhance their PAP usage, and those clinicians who closely follow up on their PAP patients recognize that finding the right interface or mask can be the cornerstone between failure versus success.
Common PAP Pitfalls
Recognizing some common PAP pitfalls can help steer management to a more successful outcome. Frequently during PAP titration studies, patients are placed on full face masks (FFMs) from the beginning of the night to prevent difficulties related to oral pressure leakage, which can occur from the pressure gradient when opening the mouth while on PAP. In other instances, the sleep study starts with a nasal mask but the technologist quickly transitions to a FFM when oral pressure leakage occurs, without attempting to use a chinstrap or employ PAP features such as a lower pressure on exhalation (for example, ResMed’s EPR or Philips Respironics’ C-Flex). Or a patient may be titrated with a nasal mask the entire titration night but when experiencing therapy difficulties at a later date be switched to a FFM, under the assumption that the optimal pressure identified while wearing the nasal mask will also be the optimal pressure on the FFM.
In any of these common scenarios, patients ultimately find themselves on FFMs. But clinicians may not realize that a relaxed mandible during sleep can cause problems unique to FFMs in certain patients.
While an advantage of the FFM is the elimination of a pressure gradient between the nose and the mouth, FFMs have added complexities because of their larger surface area, which requires a pressure seal with the skin to prevent leakage, and because the mask must withstand movement of the mandible without a loss of the pressure seal that would otherwise create pressure leakage.
When the mandible becomes relaxed during sleep, pressure can leak from the FFM around the mouth or chin. Then, to overcome the leakage, patients may tighten the lower straps to improve the seal—but this frequently worsens the airway obstruction by moving the mandible posteriorly.
From our clinical experience, the pressure levels needed to prevent obstruction with a nasal mask are not always the same as with a FFM. Frequently higher pressures are needed with FFMs. This higher pressure requirement is likely the result of changes in the upper airway brought on by tightening of the lower FFM strap, thus bringing the mandible posteriorly. This problem typically goes unrecognized as a contributing factor in PAP failures with FFMs.
Solutions to PAP Failures Caused by an Unstabilized Mandible

The FCM is a full face mask made from an impression of the patient’s face and includes a connected oral appliance that stabilizes the mandible.
To overcome the difficulties with FFM failures, I (Simmons) studied a boil-and-bite dental appliance, designed for treating snoring and sleep apnea, and found that its function in mandibular stabilization improved outcomes in FFM failure patients.3 Moving the mandible posteriorly, also known as “distalization of the mandible,” is associated with tightening the lower straps of a FFM. But an oral appliance stabilizes the mandible so when the FFM is strapped on tight, the airway is not compromised through distalization of the mandible.
This type of combination therapy—when the oral appliance is used at the same time as PAP but without physical integration of the mask with the oral appliance—is sometimes referred to as “dual therapy.” Any dentist who currently provides oral appliance therapy can offer this combination therapy option to patients as a solution to failed mono-therapies with PAP oral appliances. The oral appliances that are most effective for dual therapy are those that do not allow the lower jaw to open passively. It is the mandibular stabilization that is critical to the success of this type of combination therapy.
A second and emerging type of PAP-oral appliance combination therapy is sometimes referred to as “integrated therapy.” In integrated therapy, the PAP is physically attached to the oral device, eliminating the need for straps for anchoring the mask and providing mandibular stabilization.
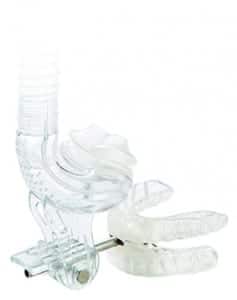
An example of integrated therapy, the TAP PAP CS attaches a nasal pillow PAP mask to an oral appliance.
One type of integrated combination therapy device attaches a nasal pillow PAP mask to an oral appliance. An example is the TAP PAP CS, which adds a post to a TAP appliance that is attached to an interface that holds a nasal pillow cushion in place. The combination type brings the mandible forward to the desired degree while the nasal pillows are securely held in position by anchoring to the teeth by way of the appliance. This is more stable than any nasal mask with straps because the nasal pillows maintain a fixed relationship with the head as the head moves; whereas with straps, as the head moves, the nasal pillows tend to move slightly as the strap tension changes with the movement on the pillow. This type of configuration works well typically for PAP pressures less than 15 cm H2O. The post breaks the lip seal and with higher pressures, from our clinical experience, there can be leakage alongside the oral device.
For patients who need higher pressures, or who have an uncontrolled tendency to open their mouth, there is a newer integrated therapeutic approach that consists of an integrated combination oral appliance with a FFM. Originally designed by Keith Thornton, DDS, this approach utilizes a custom PAP full face mask made from an impression of the patient’s face.4 This custom fabricated facial mask attaches to a post similar to the TAP PAP CS described earlier, which protrudes from an oral appliance that anchors both upper and lower teeth, stabilizing the mandible. Ronald Prehn, DDS, has implemented these concepts into the new Fusion Custom Mask (FCM). The FCM is anchored in place by the teeth, so no straps are needed to keep it in place. The FCM utilizes the same principles as previously recognized by Simmons in his study demonstrating improved performance of FFMs by providing mandibular stabilization. The dental sleep medicine practitioner will need additional training in order to provide this therapeutic option for their patients and sleep physician (see “Integrated Therapy Training Opportunities”). Patients who benefit the most from the FCM design are typically the more challenging ones who require high pressures and tend to suffer from intolerance of PAP therapy, many who have also failed oral appliance therapy alone.5
The authors (Simmons and Prehn) have been collaborating for over 15 years and frequently handle challenging OSA patients by using the FCM integrated therapeutic approach. Patients are referred from Comprehensive Sleep Medicine Associates for FCMs if they encounter difficulties with PAP after exhausting other PAP-adherence strategies, such as nasal masks with chin strips or mono-therapy full face masks. While many patients use PAP therapy successfully, Simmons thinks most patients would do better by utilizing a treatment that consists of mandibular stabilization as part of the overall airway management.
Integrated Therapy Training Opportunities
The Sleep Education Consortium, a 501(c)(3) nonprofit organization, will hold an upcoming course on combination therapy approaches. It will take place in Houston on Oct 12-14 and will provide 24 hours of continuing education credits for dentists; 12 hours of continuing medical education credits are provided by the Texas Medical Association for physicians, who will attend lectures alongside their dental colleagues in the same classroom learning the same material on Oct 13-14 . The conference is in its 13th year. Physicians will learn about complex cases and about when to request combination therapy for OSA patients. For more information, visit www.dentalsleepconference.com or www.sleepeducation.net. Education specifically focused on the Fusion Custom Mask can be found at www.fusioncustommask.com.
The authors are writing articles such as this one and teaching classes so as to promote collaboration as the next wave of enhancement in sleep medicine.
[sidebar]
Upcoming Combination Therapy Courses
The authors teach courses in combination therapy. To learn more or to sign up, visit:
[/sidebar]
Jerald H. Simmons, MD, is triple board certified in neurology, epilepsy, and sleep medicine. In 2006, he founded and continues to direct Comprehensive Sleep Medicine Associates, which has four locations in Texas. In 2004, he established the Sleep Education Consortium, a 501(c)(3) nonprofit organization that holds continuing education conferences with a mission to enhance the knowledge of healthcare professions on sleep disorders. Ronald S. Prehn, ThM, DDS, is the owner of Restore TMJ & Sleep Therapy in The Woodlands, Tex. He is a member of the American Academy of Orofacial Pain and the American Academy of Dental Sleep Medicine, is president-elect of the American Board of Dental Sleep Medicine, and is on the board of the Sleep Education Consortium. He is president of Fusion Sleep Solutions, LLC, which teaches courses in combination therapy including how to employ the Fusion Custom Mask.
References
1. Weaver TE, Grunstein RR. Adherence to continuous positive airway pressure therapy: the challenge to effective treatment. Proc Am Thorac Soc. 2008;5(2):173–8.
2. Gay P, et al. Evaluation of positive airway pressure treatment for sleep related breathing disorders in adults. Sleep. 2006;29(3):381–401.
3. Simmons JH. Improved outcome of full face mask CPAP treatment with mandibular stabilization using a dental appliance. Journal of Sleep and Sleep Disorders Research SLEEP Abstract Supplement. 33, abstract no. 0478 (June 2010): A158.
4. Prehn R, Colquitt T. Fabrication technique for a custom face mask for the treatment of obstructive sleep apnea. J Prosthet Dent. 2016;115(5):551–555.
5. Prehn RS, Swick T. A descriptive report of combination therapy (custom face mask for CPAP integrated with a mandibular advancement splint) for long-term treatment of OSA with literature review. Journal of Dental Sleep Medicine. 2017;4(2):29–36.
TOP PHOTO: The Fusion Custom Mask is an example of integrated therapy. The PAP is physically attached to the oral appliance, eliminating the need for straps.






Great article wonderful to see the combination and collaboration!
Sleepwell!
There certainly is a place for integrated therapy, but its major problem is that, if the patient decides to remove the CPAP during the night, they will necessarily remove the oral component with it. Then they completely lose the oral appliance benefit. This is particularly important if you consider that unrestricted sleep breathing provides the greatest cardiovascular benefit during REM sleep, and the largest block of REM sleep typically occurs just before rising. With dual therapy, uncomfortable patients typically remove only the CPAP mask and leave the oral appliance in place until morning.
Great point Roy. There are three considerations. One is that with over 500 FCM patients, I have not had that experience yet. Two is that remember one indication for combination therapy is OAT failure. Therefore, their airway would not be protected even if they took off the mask and the OA remained. Three is that CPAP patients have to take off the CPAP to go to the bathroom (common in this population). Since the FCM is so comfortable and with no hassle to put on (no straps), our patients most often put the CPAP back on.