Although sex, aging, and obesity are the main factors associated with obstructive sleep apnea (OSA), research has shown that larger tongue, lateral pharyngeal walls, tonsils, soft palate, and total pharyngeal soft tissue volumes can also be considered OSA risks. Prior research has largely relied on calipers, which are used to measure the oral cavity and craniofacial dimensions of subjects, but there are limited data on reproducibility, and the process is generally considered cumbersome and unpleasant.
Researchers from the Center for Sleep & Circadian Neurobiology aimed to reproducibly quantify pharyngeal structures by using digital morphometrics based on a laser ruler and to assess differences between subjects with OSA and control subjects and associations with apnea-hypopnea index (AHI). This method would be a more cost-effective solution to expensive imaging like MRI and CT scans.
The study aimed to reproducibly quantify pharyngeal anatomy of 318 control subjects with AHI and 542 subjects with OSA and determine the differences. Using overnight polysomnography, a laser ruler, and morphometric photographs, researchers found that digital morphometrics could be used to assess the differences between subjects with OSA and control subjects and associations with AHI. Results showed that a digital camera and laser ruler can be used to quantify intraoral anatomy, particularly for measures of the tongue and mouth, airway visibility, and Mallampati score. This study also showed that measures of the tongue were larger in subjects with OSA versus control subjects in unadjusted models and controlling for age, sex, and race. Similar results were also found in patients with AHI severities.
“Digital morphometrics is an accurate, high-throughput, and noninvasive technique to identify anatomic OSA risk factors,” says Richard J. Schwab, MD, lead researcher and professor of medicine at the Hospital of the University of Pennsylvania, in a release. “Morphometrics may also provide a more reproducible and standardized measurement of the Mallampati score.”
Further information from the study can be found in the journal CHEST.

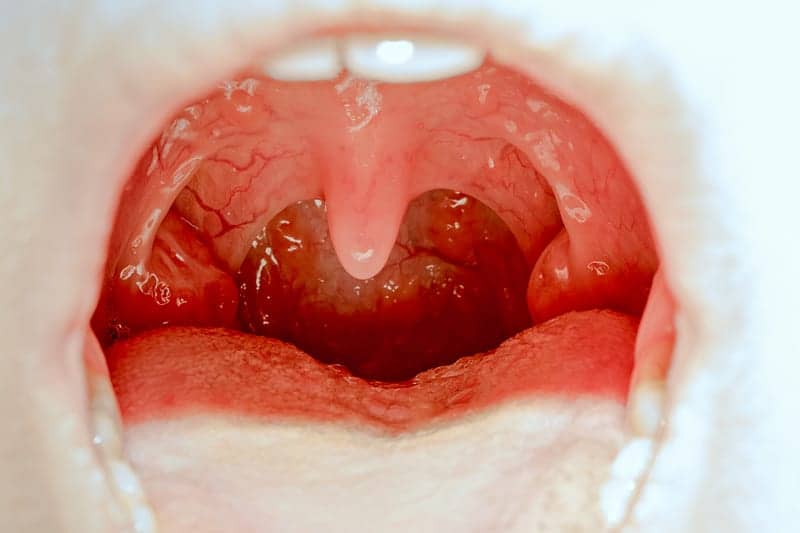






Mid face lack of development due to breathing dysfunction and postural lip and tongue habits)and then restriction (with traditional orthodontics)is responsible for the lack of space for the the tongue and pharyngeal soft tissues. If the midface is restrained from growing forward from birth to age 11, the entire complex is set back(including the soft palate). Then once teeth start to wear, more dimension is lost inside of the mouth. This is a pretty easy concept. If only physicians would realize that the mouth (and surrounding structures) is actually the most important area of the body.