More than a century ago, scientists demonstrated that sleep supports the retention of memories of facts and events. Later studies have shown that slow-wave sleep is important for transforming fragile, recently formed memories into stable, long-term memories. Now, in an Opinion article published today in Trends in Neurosciences, part of a special issue on Neuroimmunology, researchers propose that slow-wave sleep may also strengthen immunological memories of previously encountered pathogens.
“While it has been known for a long time that sleep supports long-term memory formation in the psychological domain, the idea that long-term memory formation is a function of sleep effective in all organismic systems is in our view entirely new,” says senior author Jan Born of the University of Tuebingen, in a release. “We consider our approach toward a unifying concept of biological long-term memory formation, in which sleep plays a critical role, a new development in sleep research and memory research.”
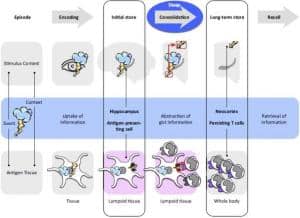
This graphic shows a model of memory formation in the central nervous system and the immune system. Image courtesy Westermann et al/Trends in Neurosciences 2015
The immune system “remembers” an encounter with a bacteria or virus by collecting fragments from the bug to create memory T cells, which last for months or years and help the body recognize a previous infection and quickly respond. These memory T cells appear to abstract “gist information” about the pathogens, as only T cells that store information about the tiniest fragments ever elicit a response. The selection of gist information allows memory T cells to detect new pathogens that are similar, but not identical, to previously encountered bacteria or viruses.
Studies in humans have shown that long-term increases in memory T cells are associated with deep slow-wave sleep on the nights after vaccination. Taken together, the findings support the view that slow-wave sleep contributes to the formation of long-term memories of abstract, generalized information, which leads to adaptive behavioral and immunological responses. The obvious implication is that sleep deprivation could put your body at risk.
“If we didn’t sleep, then the immune system might focus on the wrong parts of the pathogen,” Born says. “For example, many viruses can easily mutate some parts of their proteins to escape from immune responses. If too few antigen-recognizing cells [the cells that present the fragments to T cells] are available, then they might all be needed to fight off the pathogen. In addition to this, there is evidence that the hormones released during sleep benefit the crosstalk between antigen-presenting and antigen-recognizing cells, and some of these important hormones could be lacking without sleep.”
Born says that future research should examine what information is selected during sleep for storage in long-term memory, and how this selection is achieved. In the end, this research could have important clinical implications.
“In order to design effective vaccines against HIV, malaria, and tuberculosis, which are based on immunological memory, the correct memory model must be available,” Born says. “It is our hope that by comparing the concepts of neuronal and immunological memory, a model of immunological memory can be developed which integrates the available experimental data and serves as a helpful basis for vaccine development.”







I’d be curious to untangle whether dysregulation of the HPA related to sleep deprivation would negatively impact immunological memory formation and retention. My guess is that it would…