A study at the Penn Center for Sleep Disorders showed significant differences in the way men and women report symptoms of sleep apnea by using various methods of measurements
The study of gender differences in sleep apnea is a new and important area. We at the Penn Center for Sleep Disorders at the University of Pennsylvania Medical Center, Philadelphia, believe that women and men exhibit different symptoms associated with sleep apnea. It is also possible that certain symptoms of apnea are more important in women than men, and that these symptoms may confound the diagnostic process. This may help to explain why sleep apnea is still relatively underdiagnosed in females as compared to males.1
Pillar et al2 demonstrated a difference in the presentation of sleep apnea symptoms among men and women. These subjects were all referred for polysomnography. Men reported excessive daytime sleepiness symptoms (including daytime fatigue and tiredness) as most significant. Women, on the other hand, reported more symptoms of fatigue, insomnia, tension, and the use of sedatives. Therefore, it is understandable that women who have sleep apnea may be misdiagnosed with depression, a disorder that shares many of the same symptoms as the women described in Pillar’s study.2 This is especially true if such women do not complain of snoring or other classic apneic symptoms. Young and associates3 found that women reported more morning headaches, while men concentrated on classic symptoms of apnea including snoring, snorting, and gasping for breath.
Our hypothesis was that there would be significant differences in the way that men and women reported symptoms of apnea if they were studied using several reliable methods of measurement. Pillar and Young’s data2,3 support such a hypothesis. We hypothesized that men would complain of more snoring, snorting, and other classic symptoms of apnea while women would complain of more daytime sleepiness and dysfunction, difficulty sleeping, and sleep disturbances.
The Study
Data were collected from 2,757 subjects, all of who were referred for polysomnography testing at the Penn Center for Sleep Disorders. Subjects consisted of 1,799 men with a mean age of 49 ± 13.40 and 958 women with a mean age of 48 ± 14.13. Due to missing data, only 1,672 observations can be used. The mean body mass indexes (BMI=kg/m2) for men and women were 32 ±7.77 and 35 ± 11.00, respectively. There was a total of 1,933 Caucasian subjects (male N=1,383, female N=550), 713 African-American subjects (male N=347, female N=366), 46 Asian subjects (male N=31, female N=15), 34 Hispanic subjects (male N=22, female N=12), two American Indian subjects (male N=1, female N=1) and 29 subjects classified as “Other” (male N=15, female N=14). All of the subjects were asked to fill out the same questionnaires: The Multi-Variable Apnea Sleep Symptom Frequency Questionnaire (MAP),4 the Epworth Sleepiness Scale (ESS),5 and the Pittsburgh Sleep Quality Index (PSQI)6 (Tables 1-3).
After the patients underwent polysomnography tests and their diagnoses were established, they were separated by severity of respiratory disturbance index (RDI) for analysis. There were four groups of RDI levels: <5 (normals); <15 (mild apnea); 15-30 (moderate apnea); and >30 (severe apnea). Subjects were also separated by gender.
| MAP I1 | Apnea | Snorting, or gasping; breathing stops, loud snoring |
| MAP I2 | Difficulty Sleeping | Frequent awakenings; tossing, turning; morning headaches |
| MAP I3 | Daytime Sleepiness | Falling asleep at work or while driving; excessive daytime sleepiness |
| MAP I4 | Narcolepsy-like Symptons | Awaken feeling paralyzed; vivid dream-like state while falling asleep or awakening. |
| TABLE 1. Multi-Variable Sleep Symptom Frequency Questionnaire. | ||
| Situation |
Score |
| Sitting and reading Passenger in a car Lying down to rest in the afternoon Sitting and talking to someone Sitting after lunch without alcohol In a car, stopped for a few minutes in traffic Total (Normal < 10) |
|
| TABLE 2. Epworth Sleepiness Scale. | |
| PSQI 1 | Subjective Sleep Quality | Rating Sleep Quality |
| PSQI 2 | Sleep Latency | Length of time it takes to fall asleep |
| PSQI 3 | Sleep Duration | Hours of sleep time |
| PSQI 4 | Habitual Sleep Efficiency | Number of hours slept/number of hours spent in bed x 100 = % |
| PSQI 5 | Sleep Disturbances | Getting up while sleeping; cannot breathe; bad dreams; pain |
| PSQI 6 | Use of Sleep Medication | Frequency of use |
| PSQI 7 | Daytime Dysfunction | Difficulty staying awake while driving; maintaining enthusiasm |
| TABLE 3. Pittsburgh Sleep Quality Index. | ||
Multi-Variable Apnea Sleep Symptom Frequency questionnaire
All subjects filled out the MAP, designed by the Center for Sleep Disorders at the University of Pennsylvania Medical Center as a screening tool for sleep apnea based on the reporting of various symptoms of sleep apnea and other sleep disorders plus age, body mass index, and gender.4 The MAP variables focus on typical symptoms of apnea including snoring, snorting, difficulty sleeping, and daytime sleepiness (Table 1).
MAP I1
The first variable, MAP I1, is a measure of traditional apneic symptoms: apneas, snoring, and snorting. In our study, there were no significant differences between the way that women and men answered this question, but the results were found to be dependent on RDI. A linear trend was found showing that as severity of apnea increased, so did the frequency and severity of these symptoms (Figure 1).
MAP I2
In the second variable, MAP I2, there were significant differences in the way that women answered these questions. This variable examines difficulty sleeping— specifically, frequent awakenings; tossing, turning, or thrashing; difficulty falling asleep; legs feeling jumpy or jerky; and morning headaches. While the results were not dependent on RDI severity, women had a significantly higher score on this question than men (P<0.05). So, while male and female normals had no significant difference in score (the same at all RDI levels), the answers of men and women in general showed a difference (Figure 2).
MAP I3
Answers in the third MAP variable (MAP I3) were not significantly different between genders. The measurement of daytime sleepiness (falling asleep when at work or school, falling asleep when driving, and excessive sleepiness during the day) did not demonstrate gender-
related differences, but there were differences associated with RDI severity. The trend showed a steady increase in scores as apneic severity increased (with a small drop for women between the <5 – >5 group), and then a large jump for the severe apneic group (Figure 3).
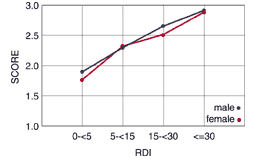
Figure 1. MAP I1.
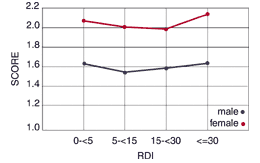
Figure 2. MAP I2.
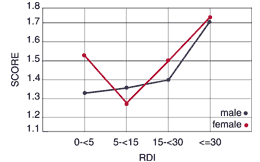
Figure 3. MAP I3.
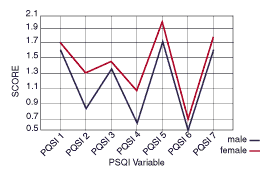
Figure 4. PSQI Gender Diferences.
Epworth Sleepiness Scale
The second method of measurement was the ESS, a self-administered eight-item questionnaire. The ESS has been proven to be a simple and reliable measure of daytime sleepiness in adults.5 The ESS asks the patient to rate their likelihood of falling asleep at a given time. The scale is 0-3: 0=never, 3=always (Table 2, page 32).
Our data found that severity of apnea had the greatest correlation with the ESS measure of overall sleepiness in adults. Results showed that as RDI increased, so did overall sleepiness. Gender had no significant impact on these symptoms.
Pittsburgh Sleep Quality Index
The third questionnaire used as a measure was the PSQI. The PSQI is designed to measure sleep quality and disturbance retrospectively over a month period using a self-report method.5 The PSQI has served as a measure of subjective sleep quality in elderly and psychiatric patients and has seven main variables (Table 3, page 32).7,8 All of the PSQI variables showed significant differences in the scores between men and women (P<0.05) (Figure 4).
In the PSQI 1, women had significantly higher scores than men (P<0.05). This measure would mean that women rated their overall sleep quality as better. Significant differences among RDI levels were also found (P<0.05). While scores increased across levels of RDI from mild to severe apnea, normals had a higher score than all other groups indicating that they thought they had the best sleep quality.
On variable PSQI 2, a measure of sleep latency, women scored significantly higher than men (P<0.05). These differences indicate that women take a longer time to fall asleep than men. However, based on the scores from PSQI 3, a measure of sleep duration, women actually thought that they slept significantly longer than men (P<0.05).
On the PSQI 4, which measures sleep efficiency (time spent in bed/time spent sleeping), women scored significantly higher than men (P<0.05). This is consistent with the earlier finding that women consider their sleep to be of better quality than men. We also measured the frequency and severity of sleep disturbances on the PSQI 5. Women scored significantly higher than men (P<0.05) on this variable. Although women reported significantly worse sleep disturbances, they actually thought that their sleep was of significantly higher quality.
When measuring the use of sleeping medications (PSQI 6), women scored significantly higher than men. It is also interesting to note that use of sleeping medications differed significantly between RDI levels (P<0.05). Subjects considered normals (RDI < 5) used significantly more sleeping medications than all apneic subjects, and apneics in the mild (RDI 5-15) category used sleeping medications more frequently than moderate (RDI 15-30) and severe (RDI > 30) apneics. The severe apneics used significantly more sleeping medications than moderate apneics (P<0.05). The interaction between gender and RDI also proved to be significant (P<0.05). These data indicate that the frequency of use of sleeping medication increased across RDI levels, and was greater in females, and there was also a significant difference between the use of sleeping medications among men and women within each RDI category (P<0.05). Normal women used more sedatives than normal men. Mildly apneic women used more sleeping medications than men of the same category. Moderately apneic men used more sleeping medications than moderately apneic women, and women with severe apnea had a higher instance of use than males with severe apnea. Again, as stated earlier, normals of both genders used sleeping medications more frequently than men and women in all other categories.
On variable PSQI 7, which measures daytime dysfunction, women noted that their symptoms were significantly worse than men (P<0.05), suggesting that even though their sleep quality was good, it may not be good enough.
Findings
There are a number of important findings in this study. First and foremost, the prevalence of significantly higher scores of apneic symptoms for women than men demonstrate that women do experience certain symptoms of apnea differently than men. The data from Pillar et al1 support these findings. They demonstrated gender-specific symptom profiles of women with suspected apnea. Women complained more of fatigue and consumed more sleeping pills. Their findings also were independent of the level of apnea and were most likely more related to environmental factors. Millman et al8 found a relationship between patients diagnosed with apnea and depression. Forty-five percent of the apneic patients interviewed were depressed according to a self-report questionnaire. Considering similarities between the symptoms associated with depression and sleep apnea (fatigue, lack of motivation, and loss of vital energy), this is not surprising. Eleven of these patients who were treated with continuous positive airway pressure (CPAP) no longer fit the DSM-IV criteria for depression.
Conclusion
When separating the subjects by gender, women reported more difficulty sleeping on the MAP and PSQI; longer sleep latency and duration as well as better sleep efficiency on the PSQI; and greater sleep disturbances on the MAP and PSQI. Women and men demonstrated no differences in excessive daytime sleepiness (EDS). However, women had higher scores on some symptoms associated with EDS, such as maintaining enthusiasm. When separated by severity of apnea, classic apnea symptoms increased across all levels of RDI breakdown, as well as sleep disturbances and daytime sleepiness.
Gender differences in apnea symptoms require further research. Studies need to focus on the effect of socioeconomic status and ethnicity in the presentation of sleep apnea. Quality of life measures associated with sleep apnea need to be examined for possible gender bias and modifications need to be made in the screening tools for apnea since our data demonstrate that women with sleep apnea respond differently than men. In addition, there may be differences in the anatomical structure of the upper airway of men and women, which could affect the diagnosis of this very common disorder.
Jessica J. Runyon is clinical research coordinator; Greg Maislin, MA, MS, is director of biostatistical core; and Richard J. Schwab, MD, is director of medicine and assistant professor, all at the Penn Center for Sleep Disorders, Philadelphia.
References
1. Schwab RJ. Sex differences and sleep apnoea. Thorax. 1999;54:284-285.
2. Pillar G, Lavie P. Psychiatric symptoms in sleep apnea syndrome: effects of gender and respiratory disturbance index. Chest. 1998;144:697-703.
3. Young T, Hutton R, Finn L, Badr S, Palta M. The gender bias in sleep apnea diagnosis: are women missed because they have different symptoms? Arch Intern Med. 1996;156:2445-2451.
3. Maislin G, Pack A, Kribbs N, et al. A survey screen for prediction of apnea. Sleep. 1995;18:158-166.
4. Johns MW. Reliability and factor analysis of the Epworth Sleepiness Scale. Sleep. 1992;15:376-381.
5. Buysse DJ, Reynolds C III, Monk TH, Berman SR, Kupfer DJ. The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res. 1989;28:193-213.
6. Carpenter JS, Andrykowski MA. Psychometric evaluation of the Pittsburgh Sleep Quality Index. J Psychosom Res. 1998;45:5-13.
7. Gentili A, Weiner DK, Kuchibhatla M, Edinger JD. Test-retest reliability of the Pittsburgh sleep quality index in nursing home residents [letter]. J Amer Ger Soc. 1995;43:1317-1318.
8. Millman RP, Fogel BS, McNamara ME, Carlisle CC. Depression as a manifestation of obstructive sleep apnea: reversal with nasal continuous positive airway pressure. J Clin Psychiatry. 1990;51:309-310.






