A new method proves to combine desirable attributes of both thermal and nasal prong pressure means of flow sensing when detecting sleep-related breathing disorders during polysomnography.
Traditionally, thermal devices such as thermistors or thermocouples have been used in the detection of sleep disordered breathing (SDB) during polysomnography. The signal produced is a surrogate for actual patient airflow. These devices, however, have a relatively slow response time, due to their thermal mass, making the detection of more subtle SDB attributes, such as those associated with upper airway resistance syndrome, difficult. Interest in the detection and diagnosis of this degree of upper airway obstruction has led to the monitoring of nasal prong pressure (NPP).1,2
NPP may be much more sensitive to small, higher frequency changes in patient airflow, but its response is not linear. The pressure in the cannula is roughly proportional to the square of the flow. The result is that changes in airflow are exaggerated. A 50% drop in airflow is shown as a 75% drop by the NPP. Farre and colleagues3 have implemented a linearizing circuit to correct this deficiency, but such a circuit is not currently available commercially. Thurnheer et al4 observed that square root transformation may linearize the nasal pressure/airflow relationship over short time periods, but the relationship among these signals was highly variable if comparisons were extended over an entire night. Further, it is not essential for improving accuracy of apnea/hypopnea scoring compared with analysis of the nasal pressure raw signal. To avoid overestimation of the apnea-hypopnea index (AHI), Thurnheer et al suggested changing the amplitude reduction criteria for hypopnea to <25% of baseline.
In a study comparing thermistors to NPP, Series and Marc5 found that some of the events counted as apneas by the NPP method were caused when the patient changed from nasal to oral breathing and the events were not true apneas. It is then a concern that moderate to severe hypopnea events may be incorrectly scored as apnea events when using NPP.
A recently developed device may combine desirable attributes of both thermal and NPP means of flow sensing. The device utilizes polyvinylidene fluoride film (PVDF) to create a thermal sensor that has very low thermal mass. The sensor purports to have the fast response time of the NPP, while retaining the linear flow measurement of other thermal sensing methods.
In order to determine if PVDF could overcome some of the limitations of NPP and provide a more accurate differentiation of hypopneas and apneas, we compared the results of a polysomnogram study while simultaneously monitoring NPP and the new sensor on 10 patients with suspected obstructive sleep apnea (OSA) undergoing a scheduled polysomnogram.
Methods
Airflow tracings derived from monitoring NPP and a PVDF airflow sensor were recorded and digitized simultaneously during a polysomnogram. The default amplifier gain and filter settings used for both devices were as follows:
|
Gain |
Hi Pass |
Low Pass |
60Hz |
|
|
PVFD |
250 uv |
0.1 Hz |
15 Hz |
On |
|
NPP |
500 uv |
0.1 Hz |
15 Hz |
On |
During the initial physiological calibration portion of the recording, the gain settings for each device were slightly modified to allow for identical and maximal signal strength during normal breathing for each device without “pen blocking.”
A trained and experienced polysomnographic technologist then analyzed and scored all of the collected data to identify respiratory events. Respiratory events were defined as follows:
Apnea—80%-100% reduction in airflow signal amplitude.
Hypopnea—50%-80% reduction in airflow signal amplitude.
The technologist first scored the NPP data for all 10 patients. After a report for each patient’s scored respiratory data was generated, the “tagged” event indicators within the raw data were deleted. One week later, the technologist then scored the PVDF data in a randomized order without any visual evidence of what was previously scored within the NPP data relating to any specific event. A report of the NPP scored data was then generated.
Results
Comparison results relating to the total respiratory events by event category: the difference in percent of events (PVDF 54% ± 18.4%, NPP 83% ± 13.2%) scored as apneas was significant (P<.001). The difference in the total number of events was not statistically significant.
Discussion
The data indicate that in 10 out of 10 patients, the PVDF airflow sensor revealed many respiratory events consistent with hypopnea, which were presented by NPP to be apnea. In other words, the PVDF device was able to present more respiratory events within the hypopnea category as compared to NPP. This discrepancy may have clinical implications relating to potential inaccuracies within the practice of prepolysomnogram apnea screening used to estimate OSA severity for consideration of unattended diagnostic polysomnogram methodology, which is a growing trend within the sleep medicine community.
PVDF and NPP provided nearly identical results for the sum of apnea and hypopnea events. The PVDF device appears to be more sensitive to the patient’s oral/nasal airflow than NPP and will likely more accurately differentiate between true apnea or hypopnea, particularly with mouth breathing. Breathing patterns occurring during a respiratory event within the threshold of 20% to 50% of the normal respiratory waveform amplitude were present in the PVDF recording, but were not present for the same event in the NPP recording.
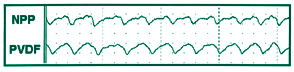
Figure 1. Sample waveforms during “normal” breathing.
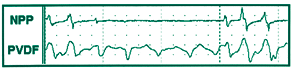
Figure 2. Sample waveforms during a “hypopnea” episode.
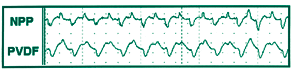
Figure 3. Sample waveforms during “flow limited” breathing.
A comparison of the wave shapes (Figures 1-3) suggests that the sensitivity of the PVDF sensor, as demonstrated during this trial, may also be advantageous to the clinician as a noninvasive method of detecting and displaying very subtle, mild changes in respiratory patterns (flow limitation), as well as respiratory patterns associated with more frank obstructive events (apnea and/or hypopnea), as compared to NPP as well as thermistor and thermocouple methods.
Todd M. Eiken, RPSGT, is director of the Metropolitan Sleep Disorders Center, St Paul, Minn.
References
1. Berg S, Haight JS, Yap V, Hoffstein V, Cole P. Comparison of direct and indirect measurements of respiratory airflow: implications for hypopneas. Sleep. 1997;20:60-64.
2. Norman RG, Ahmed MM, Walsleben JA, Rapoport DM. Detection of respiratory events during NPSG: nasal cannula/pressure sensor versus thermistor. Sleep. 1997;20:1175-1184.
3. Farré R, Rigau J, Montserrat JM, Ballester E, Navajas D. Relevance of linearizing nasal prongs for assessing hypopneas and flow limitation during sleep. Am J Respir Crit Care Med. 2001;163:494-497.
4. Thurnheer A, Xiaobin X, Block K. Accuracy of nasal cannula pressure recordings for assessment of ventilation during sleep. Am J Respir Crit Care Med. 2001;164:1914-1919.
5. Series F, Marc I. Nasal pressure recording in the diagnosis of sleep apnoea hypopnoea syndrome. Thorax. 1999;54:506-510.






