A Diplomate walks those less familiar with the process step-by-step through oral appliance therapy.
Oral appliance therapy (OAT) provides an alternative treatment option for those with upper airway resistance syndrome and obstructive sleep apnea (OSA). The patient’s treatment journey begins with the referring physician, who will have administered a sleep test, and, either due to the patient’s noncompliance with CPAP or the patient’s preference, sends the patient to a dental sleep medicine practitioner for an oral appliance.
The dentist’s job in properly treating a sleep apnea patient with an oral appliance involves a set of processes that are undertaken with the goal of identifying the patient’s specific needs, the condition of their mouth and throat, and their systemic health. Once the patient has been thoroughly evaluated, the appropriate device can be selected and fitted, allowing the patient to begin their treatment and follow-up.
Outlined here is the standard process used in my office to guide the patient from initial consultation to successful treatment. While each dentist runs his or her office slightly differently, this patient journey is usually followed with the goal of selecting the appropriate appliance and treating the patient’s OSA long-term.
The Initial Appointment
In this appointment, the sleep test is reviewed and interpreted to confirm the patient’s suitability for oral appliance therapy. Disqualifiers for OAT include physical conditions that would make it extremely uncomfortable for the patient to wear an appliance, such as acute temporomandibular joint distress, or gum or dental issues that would prohibit the device’s adherence to the teeth or dental implants.
In addition to administrative and procedural paperwork, I also have my patients fill out a CPAP intolerance form. Many dental sleep medicine practitioners use similar forms, which generally serve to gather detailed information about the patient’s reason for intolerance to CPAP and their decision to turn to an oral appliance for sleep apnea treatment. On the form in my office, patients may check boxes that include an inability to get the mask to fit properly, claustrophobia, and disturbed/interrupted sleep caused by presence of the device.
Records Appointment
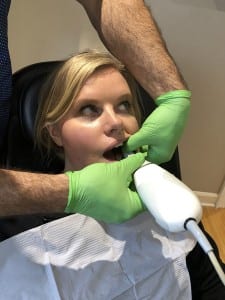
If the patient is ready to move forward with treatment during the initial appointment, a digital scan or standard impression is administered by a sleep assistant. Alternatively, these records may be taken during a secondary appointment if the patient indicates during the initial consultation that s/he would like to think about the options, doesn’t have time to have records taken during the initial appointment, or wants to discuss the options with a partner. Additionally, records may be taken at a secondary appointment if the patient has yet to be diagnosed with OSA or has not received treatment for a significant length of time and needs to be retested.
The purpose of taking scans/impressions is two-fold: to thoroughly scan the teeth in order to provide a full picture of the mouth, soft tissue, and throat, and to gather information that will help properly fit the appliance. The decision to use either a digital scan or standard impression will largely depend on the patient as well as the dental sleep medicine practitioner’s preference, though there are some qualifying conditions that may dictate one method over another. If the patient is prone to gagging, for example, a digital scan will reduce discomfort and be easier to complete; if the patient has a small mouth, impressions are recommended, as the scanner on many existing cameras is too large for small mouths.
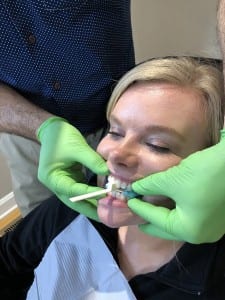
After impressions are gathered, a bite record is taken. In my office, the preferred method of gathering a bite is the George Gauge. George Gauge bites are taken with a 2 mm, 3 mm, or 5 mm fork depending on how much the bite should be opened.
Selecting an Oral Appliance
With records taken, an informed decision can be made about which appliance will most appropriately treat the patient. This decision is based on several factors, including the patient’s body mass index (BMI), apnea-hypopnea index (AHI), range of motion, gender, and medical history.
In most cases, appliance selection is straightforward. Some examples of special appliance selection cases include an edentulous patient, who would benefit from a tongue retaining device, or a patient with material sensitivities, who may benefit from a device with no metal, or patients who are pilots or commercial drivers, who would benefit from an appliance with an objective compliance tracking chip.
Once the decision about the appropriate appliance is made, the information is then sent to the lab, where the appliance is developed.
Fitting and Delivery
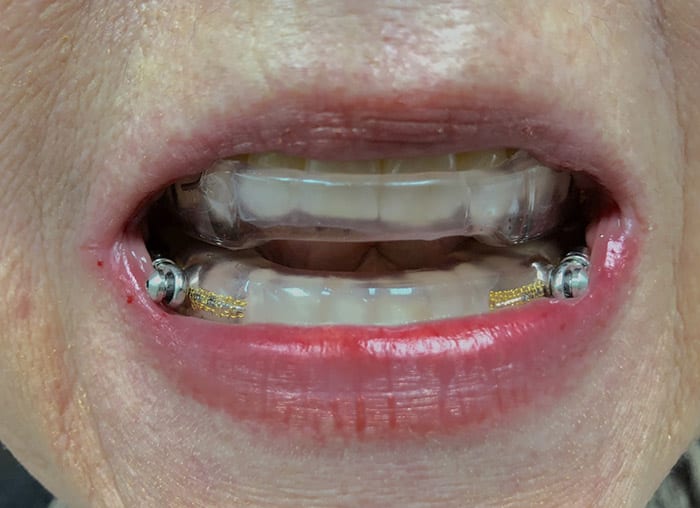
Assuming the records appointment was accurate, the fitting appointment should go fairly smoothly. Once the model is returned from the lab, bite position is checked against the position provided to ensure they are a match. If not matched, generally the appliance has to be remade to ensure accuracy. My office also checks that the appliance has the maximum amount of retention the patient can tolerate. While a good amount of generalized retention is important, also important is the absence of localized pressure areas. If pressure spots are not relieved, orthodontic movement can occur, which all good dental sleep medicine practitioners try to avoid. Adjustments are made accordingly during this appointment to maximize patient comfort while maintaining good clinical retention.
At delivery, most offices also provide each patient with information about home care for the device and morning jaw exercises, which help maximize comfort and may reduce the chance of bite change over time. A few examples of jaw exercises my office encourages patients to do are:
- The Thinker Position, in which the patient rests their elbow on a table or countertop and places their chin in their palm, letting the weight of their head rest on their hand, and then opens and closes their mouth. The patient alternates this movement with a side-to-side movement of the jaw.
- The AM Aligner, in which the patient takes the AM aligner provided to them at delivery and holds one end in their hand, biting slowly until the jaw feels normal.
- The Chewing Gum, in which the patient takes a pack of sugarless, soft gum with them in the shower. The hot water of the shower helps relax the muscles, and the chewing helps return the jaw to a normal position.
During delivery, my office also shows the patient how to adjust their appliance and provides them with an oral appliance calibration chart, which allows the patient to track how many turns to the right, left, and center are issued each night. In the interest of total health, my office also educates the patient about good sleep hygiene such as keeping consistent bed and wake times, maintaining a cool sleep environment, and reducing caffeine consumption.
Follow-Up
Finally, regular check-in is conducted to ensure the patient is comfortable and receiving appropriate treatment. In my office, beginning with their one-week follow-up, at each appointment the patient completes the Epworth Sleepiness Scale to measure daytime sleepiness, and the appliance is adjusted as needed for patient comfort. Our follow-up timeline is as follows: phone check-in: 2-3 days post-delivery; 1-week follow-up; 1-month follow-up; 3-month follow-up; 6-month follow-up (usually only for severe cases); and annual follow-up.
All improvement reported is forwarded to the patient’s referring physician. At this point in the patient’s treatment journey, all that is left is continual follow-up to ensure treatment is successful, that the appliance is working as it should, and that the patient is enjoying restored sleep.
Jeff Rodgers, DMD, DABDSM, has been in private practice for over 20 years, specializing in both general dentistry (primarily restorative, implant, and cosmetic dentistry) and dental sleep medicine. A Diplomate of the American Board of Dental Sleep Medicine (ABDSM), Rodgers is a board-certified expert in sleep, treating patients who suffer from sleep-breathing disorders at his practice in Dunwoody, Ga. He provides seminars locally and nationally throughout the year on sleep issues and oral appliance therapy as a treatment option to raise awareness for the common, but often undiagnosed, condition of sleep apnea. Rodgers earned a BS in biology from Lee University in Cleveland, Tenn, and is a 1995 graduate of the University of Alabama School of Dentistry.








Great article, Dr. Rodgers-thank you for sharing. Follow up after treatment is so key for patient experience. The 3 day follow up after delivery is so important! I am curious what type of questions you are asking your patients during that call?
Great article, Dr. Rodgers, thanks for taking the time to pen it!
I am curious which questions you are asking during that 2-3 post delivery day follow up?
Keep fighting the good fight!
Hey Rob,
Thanks for your kind comments.
The 2-3 day conversation is really very simple. It’s just things like –
How Well are you doing?
Have you been able to sleep all night withbit yet? That’s fantastic.
And then just be a cheerleader. This call is really a patient management call as much as anything else.
Let me know any other way I can help.
Regards,
Jeff
Ps. This is from my phone so forgive any typos.
Hello Dr. Rogers, good article. Just curious on on of your wording “or gum or dental issues that would prohibit the device’s adherence to the teeth or dental implants.” What’s your position on an appliance on an implant? As far as I know, it doesn’t cause any negative effects. Also, when and where do you teach your seminars? would be interested in attending. Steve Rowe (U of AL, 1986)
Hello Dr. Rodgers–I know that your article is over two years old, but it just showed up on my feed this morning. I hope that you are still able to comment!
It’s an interesting article, though I’m a bit confused by the lack of post-delivery testing. You report “asking questions” and giving the patient the highly subjective Epworth Sleepiness Scale questionnaire at each follow-up appointment, but where is the objective evaluation of the efficacy of the appliance that has been prescribed? If we were to treat patients by subjective investigation only, how could we possibly evaluate the extent or severity of OSA? Or, how could we verify to the patient that our appliances are performing?
If we were to compare this approach to OSA to that used for, let’s say, diabetes, would we “ask questions” about how the patient was feeling as the basis for our follow-up to therapy? Would we adjust their medication if the patient still “felt like their sugar was high/low”? Something seems to be missing the here–I have concerns that this subjective approach to care lacks substantive information that would protect the unwary practitioner and patient if there were an untoward outcome, or worse yet, if the patient were to succumb to the disease.
Would a plaintiff attorney, look at your records and say, “Oh, well you asked the patient about his/her nocturnal symptoms (of which the patient is completely unaware, of course), so I guess there’s no case here.”? I find it disheartening that OAT practitioners can prescribe an appliance, rest (and charge the patient accordingly) on the basis that it is a “medical device” and not include post-delivery objective investigation of the appliance efficacy. It has always been my opinion that relying on the patient to “return to their PCP or sleep specialist for PSG after completion of care” is absurd and shirking of responsibility. How can we know that our treatment is complete without an evaluation of the titration of the appliance? I may be incorrect, but somehow, I fear the approach presented in your essay lacks medicolegal fortitude.
Just like the “one and done” results of PSG testing. Why is there no testing of the diagnostic hypothesis that leads the patient to be labeled (normal, mild, moderate, severe)? I would never accept a one-time “diagnosis” of insulin-dependent diabetes without a follow-up blood draw to verify the consistency of the finding. Why is there no routine objective data collected in your approach to care?
Thanks for your consideration and consul,
Scott
Dear Dr. Bobbitt,
Thanks for your very thoughtful comments and questions. To a degree you are correct and I agree but your analogy to diabetes and testing I disagree with.
I will try and address your concerns and questions as much as possible.
My patients are always referred back to their sleep physician for appropriate follow-up. Appropriate follow-up is determined by the physician. With that said, part of my informed consent with every patient is that they are agreeing to follow-up sleep testing. And we remind them of that on a regular basis.
I assume you are aware, however, that follow-up testing is not indicated in all cases. Because of that we do not refer them back for ‘testing’ and instead tell each patient that their sleep physician is the quarterback and, in collaboration with you, they will determine appropriate follow-up which in many cases includes testing.
The diabetes analogy falls apart at that stage. You only know blood sugar levels through testing. However, if a mild case is referred to me for treatment and we alleviate symptoms then follow-up testing is not always indicated. The literature is clear that mild, asymptomatic, OSA shows no increase in morbidity or mortality.
I understand why you might make an assumption that there is ‘no routine objective data collected in my (your) approach to care. I would ask that you please allow for the fact that a 2 page quick article is not an all encompassing dissertation on systems in place or involved when a patient is under my care.
Hopefully the above explains a portion of why I leave diagnosis to the sleep physician, and that includes follow-up testing when indicated. Conversely I am not sure why you would require a follow-up test in all cases when it isn’t indicated. And are you the one making that decision or do you leave room for the sleep physician?
Sincerely,
Jeff