With more than 90 different oral appliances on the market, and the treating physician ultimately responsible for the outcomes of treatment, it only seems reasonable that the physician should be actively involved in oral appliance therapy. Prescribing a well-researched appliance, titrating the appliance in the sleep lab or doing a follow-up study after oximetry titration, and collaborating with the dentist on long-term follow-up of the patient should be the standard of care. The case of a male obstructive sleep apnea (OSA) patient who could not tolerate CPAP illustrates how a specific patient management algorithm and proper use of mandibular protrusion can lead to successful, long-term management of OSA with an oral appliance.
PATIENT HISTORY
A 31-year-old male with a chief complaint of snoring initially sought treatment from an otolaryngologist in September 1991. A screening overnight pulse oximetry test utilizing Profox software recorded a desaturation event index (DEI) of 55, mean saturation of 91.1%, time less than 90% saturation (T90) of 21.7% of the night, and a low saturation of 61%. With suspected severe obstructive sleep apnea, he was referred to an AASM-boarded sleep specialist for evaluation in October 1991.
Records show that his chief complaints were snoring and nocturnal arousals. The patient stated that he had snored for approximately 10 years. Anyone sleeping near him during that time complained of very loud and disruptive snoring. His fiancée complained of his snoring over the last year and reported pauses and gasps in his breathing. He had a history of bronchial asthma, which was exacerbated by smoking during his college years. He had not smoked for 4 years, and his symptoms improved. Also, in college he gained 50 pounds, which he thought had contributed to his problem. He stated that he usually felt rested in the morning; however, in the afternoon while on the job, he experienced mild to moderate daytime sleepiness. The result of his Epworth Sleepiness Scale (ESS) was 12, which was moderately sleepy.
The patient used aspirin as needed but used no prescription medication. He drank two cups of coffee and two cups of tea per day.
His medical history revealed orthodontic treatment with removal of four bicuspid teeth. His nose had always been congested, and he carried a diagnosis of allergic rhinitis. He stated that he had always been a mouth breather.
PHYSICAL EXAM
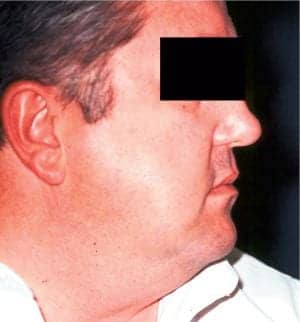
Patient in 1999. Note 23-inch neck size.
Physical exam revealed a well-developed male in no distress. His height was 6′ 2″ weight 275 pounds. Blood pressure was 144/92. Pulse was 80 and regular. Examination of the upper airway revealed a Mallampati grade III. The tongue was slightly oversized in relationship to the floor of the mouth. The neck was bull-like with a circumference of 19 inches. The remainder of the exam, including respiratory, cardiovascular, and neurologic survey, was within normal limits.
The patient underwent a polysomnogram in December 1991. The test revealed that the patient had an AHI of 57 with the nadir being 74%. The following evening, the patient underwent an initial trial of nasal CPAP. The report demonstrated that the patient’s abnormal respiratory events were well corrected at a pressure of 8.0 CMW. The patient was prescribed CPAP.
The patient returned to the sleep physician stating that he was not adherent to CPAP therapy due to numerous reasons, including removing the mask at night, dry mouth, leakage, eye irritation, and disturbance of his bed partner. He was referred back to the otolaryngologist for evaluation for surgery.
Due to his long soft palate and narrowed airway, an uvulopalatopharyngoplasty (UPPP) was performed in March 1992. His recovery was unremarkable. The patient stated that within a week his snoring had stopped and he was feeling much better. He continued to have good success with the procedure for 2 years. At that point, he started to snore and became tired and fatigued. He returned to the otolaryngologist in January 1999 with complaints of snoring, increased fatigue, and headaches. He was referred to our clinic at that time for an evaluation and possible treatment with a mandibular advancement device.
In the interim 8 years since his initial diagnosis and therapy, the patient had gained approximately 150 pounds and weighed 425 pounds. His BMI was 54.6. He developed hypertension and was prescribed two medications. His blood pressure on presentation was 142/89. Physical exam revealed a neck size of 23 inches, a very high, vaulted palate, a large, scalloped tongue, and a narrow crowded lower and upper arch. His ESS was 21, which was a significant increase from 12 in 1991. He felt that he still could not tolerate CPAP and wanted to try an oral appliance.
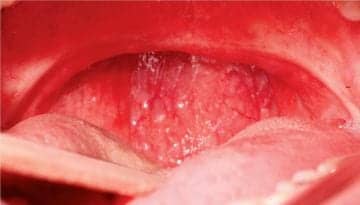
Oral cavity showing high palate, large, scalloped tongue, and UPPP.
DIAGNOSIS
Since he was already diagnosed with severe obstructive sleep apnea, a baseline, overnight oximetry study was obtained. The DEI was 87, mean saturation of 84.2%, T90 of 73.3% of the night, and a nadir of 50%. All of these results indicated a significant increase in the severity of the patient’s disease.
TREATMENT
A TAP® mandibular advancement device was fitted to the patient. His maximum voluntary or active protrusion (MAP) was 14 mm. His mandible could be passively stretched to 16 mm. Initially, his protrusion with the appliance was set at 13 mm, which was 92% of his maximum protrusion. Such an aggressive position was warranted in light of his severe apnea. A follow-up overnight oximeter study performed the next night after the delivery of the appliance showed an immediate treatment response. His DEI dropped to 38; T90 was 30%, mean saturation of 89.9%, and an oxygen nadir of 63%.
Over the next 5 months, the patient titrated himself to 19 mm protrusion or 136% of initial maximum protrusion. Three oximetry reports were accomplished during the 5 months, each one at an advanced position. All showed a dose response to the advanced position from the previous one. The final results were a DEI of 13, T90 of .4%, mean saturation of 93.4%, and a nadir of only 86%. The patient’s ESS was 5. He stated that he no longer had headaches and was not fatigued. His wife reported only “heavy breathing” but no snoring. Hypertensive medication was reduced with his blood pressure at the final appointment being 126/82. The goal of treatment was to reduce the T90 below 1% of the night. With the elimination of symptoms and the T90 at .4%, the patient was well treated with the oral appliance.
FOLLOW-UP
The patient has continued to follow up with his therapy for the last 11 years with yearly reevaluations and overnight oximetry tests. He continues to be adequately treated with the TAP appliance. However, he has titrated himself to 23 mm protrusion or 164% of initial maximum. During this time, his occlusion has remained stable. He has no pain or dysfunction of his stomatognathic system.
This case history shows the great improvement in the protrusive range of motion in an accommodation period of 5 months. The patient self-titrated to his final treatment position based solely on his symptoms and objective results with an overnight oximeter study. Over the next 11 years, the patient continued to self-titrate, which increased his range of motion to 164% of his initial protrusion. In severe patients, it is not uncommon for the apnea to increase beyond the capability of the oral appliance to manage the disease. If the T90 increases above 1% of the night, then the patient will be referred to a sleep physician for a definitive sleep test and discussion of further treatment including combination therapy, which shows great promise.1
DISCUSSION
Interest in oral appliances for the treatment of sleep apnea is growing exponentially, among both dentists and sleep physicians. Although oral appliances have been advocated for mild and moderate sleep apnea, many patients with severe apnea cannot wear CPAP. In a recent study examining compliance rates from 12 clinical trials, researchers reported that between 46% and 83% of patients are nonadherent to CPAP treatment.2 In another study, researchers showed that more than 6 hours of sleep with CPAP was required for elimination of all symptoms.3 In most cases, successful treatment of a chronic disease such as OSA requires a patient to continue treatment indefinitely. Since OSA tends to progress and get worse over time, it is important that patients return to their treating physician for regular follow-up. If they do not follow up regularly, there is a high likelihood that the patient will not be adequately treated long-term.
This case history is an example of a more than 20-year treatment of severe obstructive sleep apnea that has progressed over the years. The success with an oral appliance to this point can be attributed to a specific management algorithm. The first step is to obtain a diagnosis from a sleep physician. The present standard according to the AASM is to treat the severe patient with CPAP unless the patient can’t or refuses to wear one or prefers an oral appliance.4 The choice of an appliance for any patient should be based on independent peer-reviewed literature, preferably comparing the specific oral appliance to the gold standard, CPAP. Almost all oral appliances are different, based on the mechanism for protrusion, amount of protrusion, patient adjustability, material, fit, retention, ease of fit, skill level of practitioner required, and cost. According to the 2006 AASM guidelines, “Research is needed to clarify design characteristics most beneficial in given patient groups, so that device selection is driven by data that are more precise.”4
Today, those design characteristics have been well defined by the literature. In a randomized, parallel study comparing CPAP to the TAP oral appliance, Hoekema et al found that the oral appliance was not “inferior” to CPAP. In the study, 82% of mild to moderate patients were successfully treated by oral appliance therapy while 80% were successful with CPAP. For severe patients, the oral appliance was only 15% less effective than CPAP.5 According to the authors, “Non-inferiority of oral appliance therapy was supported by a lack of significant differences in most polysomnographic and all neurobehavioral outcomes.” The authors concluded that noninferiority could be attributed to the ability of the device to protrude the mandible, and patients’ involvement in titrating themselves to the most effective position. The author’s titration method included multiple PSGs with advancement before each PSG.
A seminal study by Holley et al6 found a higher OA success rate than reported in previous studies. According to the authors, “The AASM Guidelines and a recent review both quote a summary success rate from the literature, using AHI <10, of just over 50%. Our population’s success rate using the same criteria was 73.6%. The largest studies performed to date quote success rates of 54%, 51%, and 49.1% using an AHI <10, and 36% using an AHI <5 as the definition for success, all considerably lower than our rates. Our success rate for patients with severe disease was also higher than previously seen.” Their titration method was to have the patients accommodate and titrate themselves to a treatment position and then do a final titration in the sleep lab. The appliance can be adjusted in the mouth by either the technician, which was done in this study, or the patient. However, one of the limitations of the study was titrating only to the patient’s initial maximum voluntary or active protrusion.7
In the author’s experience, mandibular protrusion can be significantly improved over a period of time. Protrusion is typically measured at a maximum voluntary or active protrusion. Assisting the patient by applying pressure to the angle of the mandible can assist them in protruding to a greater extent or maximum passive protrusion (MPP). Kato et al8 and Isono et al9 have shown that protrusion is dose dependent. In a study by Roberts et al,10 titration of the appliance in a sleep lab to MPP with an average of 2.4 mm over MAP resulted in a decrease of 13 RDI. The average initial RDI was 44, MAP 28, and MPP 15.
These three studies, the experience of the author, and the protocol of most studies would seem to indicate that an accommodation period is necessary for optimum success with mandibular protrusion. During this time, a significant increase in range of motion, and therefore decrease in RDI, is routinely observed. Also, objective testing of the actual appliance in a sleep lab leads to the best outcomes, although titration using a pulse oximeter may be used.
W. Keith Thornton, DDS, is founder and chief technology officer of Airway Management Inc (AMI). Thornton founded AMI in order to market and supply TAP products, custom-made, patient-adjustable oral appliances, both domestically and internationally through dental laboratories. The author can be reached at [email protected].
REFERENCES
- White JR, Boota A, Essick G. Efficacy and tolerance of combination therapy using MAS supported nasal pillows. In: American Academy of Dental Sleep Medicine Annual Meeting (Awarded: Poster, Abstract of the Year); 2011; Minneapolis.
- Weaver T, Chasens E. Continuous positive airway pressure treatment for sleep apnea in older adults. Sleep Med Rev. 2007; 11:99–111.
- Weaver TE, Maislin G, Dinges DF, et al. Relationship between hours of CPAP use and achieving normal levels of sleepiness and daily functioning. SLEEP. 2007;30:711-719.
- Kushida CA, Morgenthaler TI, Littner MR, et al. Practice parameters for the treatment of snoring and obstructive sleep apnea with oral appliances: an update for 2005. SLEEP. 2006;29:240-243.
- Hoekema A, Stegenga B, Wijkstra PJ, et al. Obstructive sleep apnea therapy. J Dent Res. 2008;87:882-887.
- Holley AB, Lettieri CJ, Shah AA. Efficacy of an adjustable oral appliance and comparison to continuous positive airway pressure for the treatment of obstructive sleep apnea syndrome. Chest. 2011;140:1511-6. Epub June 2, 2011.
- Lettieri CJ, Paolino N, Eliasson AH, Shah AA, Holley AB. Comparison of adjustable and fixed oral appliances for the treatment of obstructive sleep apnea. J Clin Sleep Med. 2011;7:439-445.
- Kato J, Tanaka A, Watanabe T, Araki D, Tanzawa H, Nishino T. Dose-dependent effects of mandibular advancement on pharyngeal mechanics and nocturnal oxygenation in patients with sleep-disordered breathing. CHEST. 2000;117:1065-1072.
- Isono S, Tanaka A, Sho Y, Konno A, Nishino T. Advancement of the mandible improves velopharyngeal airway patency. J Appl Physiol. 1995;79:2132-2138.
- Roberts DH, Becker PM, Jamieson AO. Determining efficacy of a split night OA and CPAP titration protocol using PSG. Sleep. 1998;21(supplement):97.






