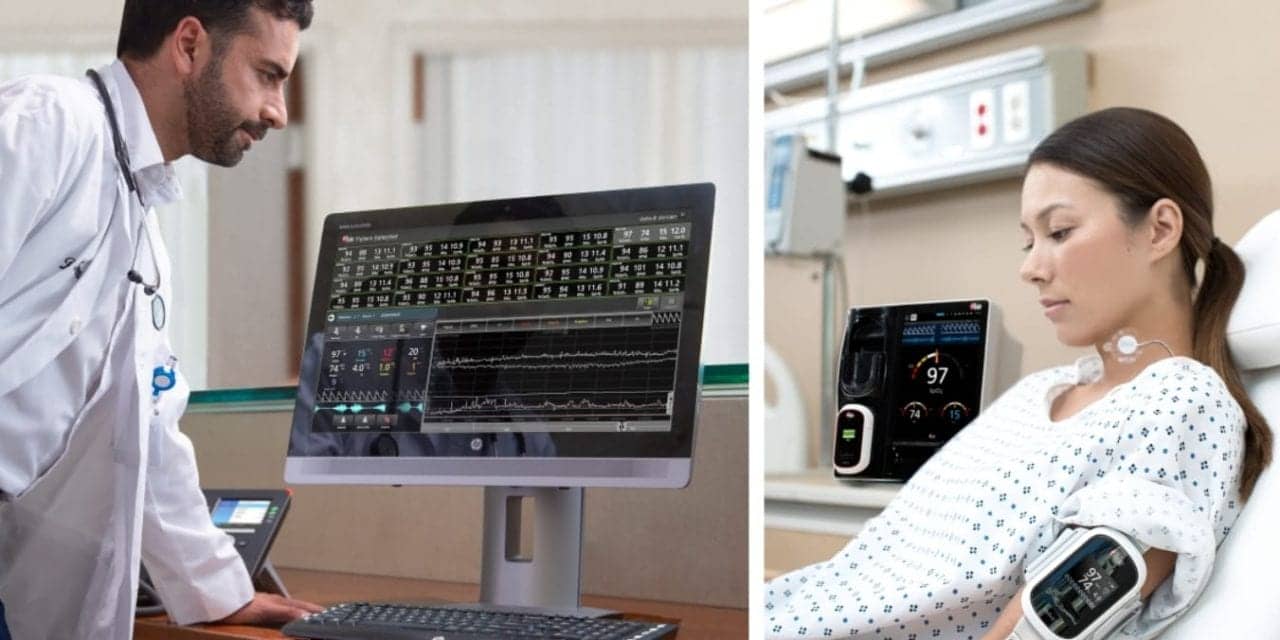
In a study recently published in the Journal of Clinical Monitoring and Computing, researchers at Nippon Medical School in Tokyo, Japan, used Masimo Patient SafetyNet and rainbow Acoustic Monitoring (RAM), acoustic respiration rate monitoring with RRa, as a centralized continuous monitoring system to identify the incidence and predictors of desaturation and bradypnea in postoperative patients. They concluding that “use of monitoring systems might provide a safety net for postoperative patients.”
Patient SafetyNet is a supplemental remote monitoring, patient surveillance, and clinician notification system that works in conjunction with Masimo and third-party bedside monitoring devices to display near real-time data at central stations. RAM with RRa uses an acoustic transducer positioned on the patient’s neck to provide noninvasive continuous respiration monitoring.
Hypothesizing that postoperative desaturation and bradypnea might occur even in non-ICU patients without serious complications, and in patients who did not undergo major surgery, Drs Masashi Ishikawa and Atsuhiro Sakamoto set up a centralized postoperative monitoring system in the general ward to investigate how common these events are for such patients (and what might predict them). They analyzed demographic and monitoring data from 1,064 adult patients who underwent general anesthesia for various surgical procedures over a 4-month period. The patients were monitored using a pulse oximeter and an RRa sensor for at least 8 hours after surgery, data which were automatically transferred to Patient SafetyNet.
From the data stored on the Patient SafetyNet, the researchers were able to retrospectively analyze the incidence of desaturation (defined as SpO2 10 seconds) and bradypnea (defined as respiratory rate 2 minutes). They found that 12.1% of patients exhibited desaturation (244 events among 129 patients), with most occurring after the termination of oxygen administration, and 50.8% of the events occurring more than 8 hours after surgery. They found that 5.1% of the patients exhibited bradypnea (112 times among 54 patients), with 72.3% of the events occurring during oxygen supplementation, and with the greatest incidence within the first hour after surgery. Age, body mass index, and current smoking status were significant risk factors for desaturation. Sleep apnea syndrome and postoperative opioid administration were significant risk factors for bradypnea. Age and postoperative opioid administration were significant risk factors for the combination of desaturation and bradypnea.
The researchers concluded, “Our study suggests that use of a continuous and centralized respiratory monitoring system for overnight postoperatively is desirable for postoperative management in the general ward, which would likely improve the safety of postoperative patients, especially those with risk factors for respiratory depression.”
The researchers commented on a number of methods of respiratory rate monitoring, stating, “Continuous and centralized monitoring of oxygen saturation and respiratory rate can detect respiratory depression before it results in critical events such as cardiac arrest. Several methods of respiratory rate monitoring are currently used, including manual counting of breaths by a caregiver, capnography, and transthoracic impedance measurement. Manual counting of breaths (such as auscultation) is an intermittent, labor-intensive and unreliable method. Capnography provides accurate and continuous monitoring, but requires a nasal or facial interface, which can be uncomfortable and may lead to failure if the interface is moved. Transthoracic impedance is non-invasive and can detect respiratory efforts, but is unable to detect alveolar hypoventilation caused by airway obstruction.”
Additionally, the researchers commented on RAM with RRa, the respiratory rate monitoring method used in the current study, and referenced another study in which RRa and capnography were compared, stating: “RRa is an acoustic monitoring device that continuously measures respiratory rate, and is as accurate as capnography in extubated patients. Patient activities, such as talking, coughing, and crying, affect the results of both RRa and capnography. The measurement errors during these activities are, however, not clinically relevant because they require that the patients are awake and breathing. Further, the RRa sensor appears to be well-tolerated and no more subject to error than capnography. RRa was found to be a reliable device and had fewer complications in this study.”